What is Shockwave Therapy?
Shockwave Therapy is a non-invasive treatment procedure that essentially involves creating a series of short energy acoustic wave pulsations that are directly applied to an injury. It uses a pneumatic generator to physically deliver the shock wave through the skin, into the body. The short-energy acoustic waves that are transmitted through the surface of the skin are spread spherically into the body and the body responds with increased metabolic activity around the pain area. It is a fast and alternative solution to surgery.
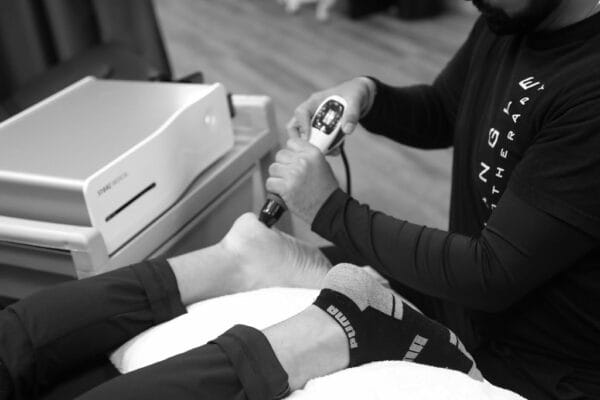
Shockwave Therapy was originally invented for the treatment of kidney stones to blast the rigid tissues into smaller pieces, making it easier to pass. After the effectiveness of that treatment was established, researchers began studying the effects of the machine at different settings and used it to treat calcific tissue and scar tissue in the body. Their findings indicate that this treatment is extremely effective for the treatment of most musculoskeletal conditions in the body.
Benefits of Shockwave Therapy
- Success rate up to 90% in the treatment of soft tissue disorders, including:
- calcific tendinitis of the shoulder,
- plantar fasciitis,
- tennis elbow, and
- piriformis muscle.
- It is an excellent cost-effective treatment
- Helpful in the treatment of chronic pain including:
- shoulder,
- back,
- heel,
- knee, or
- elbow
- No anesthesia or drugs are required
- Varied application in many fields including orthopedics, rehabilitation, and sport medicine
- Latest medical research shows that it can have a positive impact on acute pain
How does shockwave therapy work?
Shockwave Therapy is also known as extracorporeal shock wave therapy [ESWT]. It is a method that is being used more commonly in physiotherapy. Using much lower energy compared to other medical applications, it is primarily used to treat connective tissues such as ligaments and tendons.
Your physiotherapist will evaluate your condition and determine if Shockwave Therapy is appropriate for you. They will also educate you on your condition and recommend additional activities such as activity modification, tennis elbow exercises, acupuncture, massage, and posture correction to help with your healing process.
During the treatment, the therapist will direct the shockwaves into the affected area through the skin, causing no pain. The therapy is typically performed in several sessions and is a safe, non-invasive, and drug-free solution for chronic pain in the shoulder, back, heel, knee, or elbow. The latest medical research also shows that it can have a positive impact on acute pain. Shockwave Therapy is widely used in fields such as orthopedics, rehabilitation, and sports medicine.
Book an appointment for Shockwave Therapy here.
Shockwave therapy is a non-invasive treatment used to accelerate healing and reduce pain in conditions like plantar fasciitis, tendonitis, and other musculoskeletal disorders. It works by delivering high-energy sound waves to the affected area, stimulating blood flow and promoting tissue regeneration. Triangle Physiotherapy offers this treatment across various locations in the GTA, including Physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, and Liberty Village.
Derived from the Greek word spondylo means spine and listhsis stand for slipping down a slippery path. Spondylolisthesis is a disorder of the spine that results in a forward or backward slippage of one vertebra on an adjacent one. Spondylolisthesis usually happens in the lower back region, also known as the lumbar area. Spondylolisthesis has an adverse impact on the daily lifestyle and therefore it is suggested to visit a good physiotherapist in such a condition. You can visit our Physiotherapy clinics in GTA to reduce the pain and impact of Spondylolisthesis.
Types of Spondylolistheses
Spondylolisthesis can be categorized into five major types –
1. Isthmic Spondylolisthesis – This is caused by a defect in pars interarticularis – a part of the vertebra. This condition usually leads to the vertebrae slipping forward.
2. Degenerative Spondylolisthesis – This condition is usually caused when the joints lose their capacity to keep the spine alignment at the normal position. This may result in the vertebrae slipping forward.
3. Congenital Spondylolisthesis – Congenital health issues are the ones that are present in a person since birth. Sometimes there is an abnormal formation of spinal bones during pregnancy at the time of development of the baby. Here the spinal discs slip due to misalignment and malformation.
4. Traumatic Spondylolisthesis – This is caused as a result of any injury or trauma leading to slipping of the spinal discs. It is important to note that here the term traumatic indicates an injury causing damage to the spinal discs.
5. Pathologic Spondylolisthesis – This disorder is a result of a disease affecting the healthiness of the spinal bones thereby weakening the same. Diseases like osteoporosis can cause Pathological Spondylolisthesis.

Causes of Spondylolisthesis

When it comes to patient care, it is important to understand the different severities of injuries. This classification is important as it helps the medical practitioners to address and prioritize the efforts. Here, we are going to talk about the difference between injury and trauma and help you understand how does physiotherapy help in the treatment of both.
Unfortunately, the injuries caused due to trauma are very severe and require need complex medical treatment and longer recovery time. Therefore, anyone who undergoes a traumatic injury must consult the experts for their condition and avail the best physiotherapy treatment to ensure maximum and fastest recovery.
What is an injury?

What Is An InjuryIn simple terms, any instance that causes harm to the body can be classified as an injury. Injuries can be divided into different ranges, depending upon the severity and impact on the body. Some injuries might require immediate medical attention while some can heal naturally with minimum or less care. Some examples of injuries are cuts, burns, scrapes, minor concussions, broken bones and sprains. What may look like a minor injury could require urgent and special medical care. Therefore, it is suggested to visit a trained and experienced physiotherapist or practitioner in case of an injury.
What is a trauma?
Trauma can be explained as a more serious, possibly life-threatening injury, requiring urgent medical attention. A trauma is a critical injury and therefore most hospitals have a trauma center to attend and treat sensitive and urgent cases like these. Some of the examples of the trauma includes road accidents, severe cuts, burns, blunt-force trauma, serious falls, multiple broken bones, head injury, major concussions or stab wounds. Though the minor cuts or wounds can be handled by an effective first-aid kit or stitches, serious trauma like burns, bleeding artery or head injury may require extensive surgery followed by rehabilitation for a proper recovery.
Physiotherapy and Injury
When it comes to the recovery stage, physiotherapy is extremely beneficial. Many people believe that the road to recovery in injury passes through physiotherapy and the recovery can never be complete without physiotherapy. If a person has suffered from an injury from a broken bone or a sprained limb, he will face major challenges in routine activities. Simple tasks like walking or driving can be become arduous. This is where physiotherapy comes into picture. Physiotherapy provides the direction to exercise and mobilize specific muscles and tissues so that the body heals from the injury.
If a person suffers from an injury – major or minor, it is suggested that he should consult with the doctor about the recovery plan that must include physiotherapy. It is important to note that even a minimal physiotherapy helps in regaining strength and functionality post the injury. Injury recovery is not possible with a focused and dedicated physiotherapy program. For cases involving broken bones or sprains, physiotherapy is very useful to stretch and comfort the affected area and expedite the healing. Preventive physiotherapy is also beneficial for elderly patients and people at risk of injury. It helps in ensuring and maintaining balance, strength, agility and a complete range of motion while preventing injuries.
Physiotherapy and Trauma
Trauma injuries usually require more extensive and immediate surgery to fix the damage. Traumatic cases have extensive long recovery process. Patients suffer mental and physical anguish in injuries involving surgery. Based on the extent and severity of the injury, the recovery process may be anywhere from a few days to several years. In some unfortunate cases, some patients are never able to recover despite optimal surgery.
The time immediately after the injury and the subsequent surgeries is the most crucial one for people who have suffered a big physical trauma. It is this period that plays one of the biggest deciding roles in the duration and pace of the recovery. Therefore, it is suggested to consult an experienced and trained medical practitioner for the injury. Based on the injury and medical history, the doctor/medical practitioner prepares a recovery plan which starts immediately and involves a comprehensive active recovery like physiotherapy. Physiotherapy can be a painful and difficult process, but helps in regaining strength and mobility post traumatic injuries. They are a part of the recovery process in complicated cases like brain injuries and physical trauma.
Physiotherapy in GTA
Physiotherapy and rehabilitation care services can come in various forms based on the severity of the injury and medical history of the patient. For example, someone suffering from Tennis Elbow or Stress Fracture may need Shockwave Therapy Treatment, while someone who gets a head injury might need Vestibular Rehabilitation to cure dizziness and provide stability and balance to the mind. It is important to know that every situation is unique in its own way and therefore needs a different recovery plan and timeline. That is why one should be patient and adhere to the recovery plan chartered by the physiotherapist to get optimal results. At Triangle Physiotherapy, we offer a host of services aimed to provide relief from the pain and ensure preventive care for overall strength and well-being. Some of our services include –
- Pelvic Floor Physiotherapy – To encourage patients to successfully treat pelvic issues
- Vestibular Rehabilitation – To improve balance and reduce problems related to dizziness
- Shockwave Therapy – To reduce pain and promote healing shock waves are delivered to the injured soft tissues
- Chiropody – To lower the pain in the lower limbs and feet and cure mobility issues and infections
- Chiropractic – To treat the muscles, joints, bones and nerves through a non-invasive and conservative approach
- Naturopathic Medicine – To treat the root cause rather than covering up the symptoms using non-pharmacological interventions
- Massage Therapy – To promote deep relaxation, release tension and provide optimal well-being by working on the superficial and deep tissues
- Custom Bracing – To increase joint stability, improve alignment and reduce excessive movements
- Acupuncture – To help the body heal naturally by activating trigger points to relive muscle tightness
- Fascial Stretch Therapy – To achieve optimal strength, flexibility, performance and pain relief using table-based assisted stretching exercises
At Triangle Physiotherapy, we our trained and experienced physiotherapists will work with you to provide a comprehensive recovery program based on your conditions and medical history. Our services are tailor-made to provide relief and assistance to any type of injury or trauma and we ensure that you get the best recovery following our program. Our patients are our topmost priority and all our efforts are directed at providing them care and relief.
Click HERE to book an appointment with a physiotherapist at one of our eight locations.
- Physiotherapy Etobicoke – Triangle Physiotherapy Etobicoke
- Oakville Physiotherapy Clinic – Triangle Physiotherapy Oakville
- Physiotherapy North York – Triangle Physiotherapy North York
- Mississauga Physiotherapy Clinics – Triangle Physiotherapy Mississauga
- Downtown Physiotherapy Clinics – Triangle Physiotherapy King West
- Uptown Physiotherapy Clinics – Triangle Physiotherapy Lawrence Park
- Physiotherapy Clinic Downtown Toronto – Triangle Physiotherapy Queens Quay
- Physiotherapy Clinics Mississauga – Triangle Physiotherapy Erin Mills
If you are dealing with an injury or trauma, seeking professional physiotherapy can help you recover safely and effectively. Whether you’re located in physiotherapy Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, or Liberty Village, there are physiotherapy clinics available to provide specialized care and personalized treatment plans to support your recovery journey.
What is Osteoarthritis?
Osteoarthritis (OA) is the most common form of arthritis. It is a degenerative joint disease which occurs most frequently in the hands, hips, and knees. It results from the breakdown of cartilage which could cause the ends of bones to rub together, causing pain, stiffness and decreased mobility. In some cases it also causes disability and reduced function.There is no known cure for osteoarthritis but much can be done to reduce its impacts. The cornerstones of treatment for Osteoarthritis are physiotherapy and exercise but knee braces for osteoarthritis and inserts could also help.

What are the different types of knee braces for osteoarthritis?
- Prophylactic knee brace for osteoarthritis helps in prevention of injury especially during sports.
- Offloader or Unloader knee brace for osteoarthritis provide stability, pain relief, and support relief by reducing pressure on key areas.
- Rehabilitative knee brace for osteoarthritis limit movement of a joint to allow time for healing.
- Functional or supportive knee brace for osteoarthritis offers support to the knee joint to help reduce pain and discomfort.
What are the benefits of knee braces for osteoarthritis?
- A knee brace for osteoarthritis aides in the reduction of pressure and relief of discomfort by providing support on the surrounding areas on the knee cap.
- A knee brace for osteoarthritis provides compression which is very beneficial in the reduction of swelling which occurs with arthritis.
- A knee brace for osteoarthritis helps increase joint space in knee joints.
- A knee brace for osteoarthritis provides compression to reduce swelling which is one of the common symptoms in Osteoarthritis.
- A knee brace for osteoarthritis helps by shifting your weight off the most affected portion of the knee joint thus providing reduction of pain and discomfort.
- A knee brace for osteoarthritis allows more mobility while providing comfort and support.
When should I start wearing a knee brace for osteoarthritis?
Once you get diagnosed with knee osteoarthritis, book an appointment with one of our health practitioners who can assess you and recommend the best knee brace for osteoarthritis.
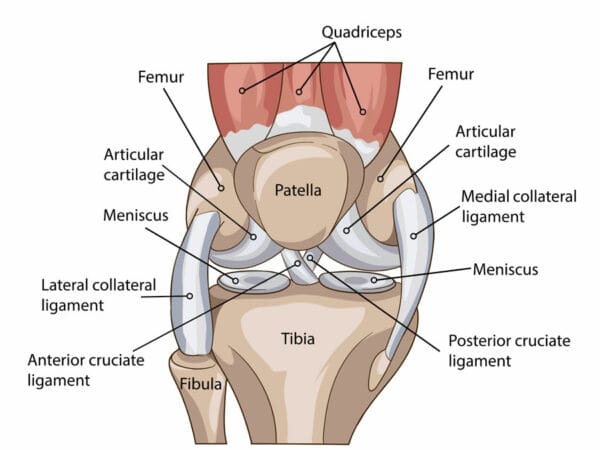
Knee pain is a very common complaint. It is something that can originate from many different structures in and around the knee. The knee joint is made up of the interaction between the femur (thigh), the tibia (shin), and the patella (kneecap). All the tissues around these areas can be contributing to your knee pain.

Common structures that can be contributing to your knee pain include but are not limited to: Ligamentous support around the knee (ACL, PCL, MCL, LCL), Meniscus Patellar Surfaces, Bursa Patellar or Quadriceps tendon. Pain in the knee could also be referral from other structures in the body such as the low back, or soft tissues further up or down the kinetic chain. Because of this, it is important to speak to a knowledgeable physiotherapist or chiropractor who can provide a detailed assessment.
People with knee pain commonly complain of inability to perform physical activity, pain when walking, standing, going up or down stairs, along with stiffness and lack of range of motion. A lot of these people are able to return to previous levels of physical function with a graded rehab program provided by a skilled practitioner. With a proper program, they are able to exceed their prior levels of function.
Physiotherapists are trained to assess, diagnose and treat musculoskeletal conditions, including knee pain. They use a variety of techniques and exercises to help alleviate pain, improve function, and prevent further injury. Some common techniques used by physiotherapists for knee pain include manual therapy, stretching and strengthening exercises, taping, and the use of modalities such as heat, cold, and electrical stimulation. Additionally, physiotherapists may provide education on proper body mechanics, ergonomics, and lifestyle modifications to help prevent future injury.
If you are struggling with knee pain, be sure to seek out a physiotherapist or certified FRC practitioner who can help you reach your physical activity goals.
Femoroacetabular impingement (FAI) is a condition in which structural abnormalities develop on the bones of the hip, resulting in premature contact (impingement) during movement. The hip is a ball and socket joint. The “ball” is the rounded top of the femur or thigh bone, and the “socket” is the concave portion of the pelvis called the acetabulum. When abnormal bone growth forms on the femoral head, it is called CAM impingement, and when on the acetabulum, it is called pincer impingement.
Like other joints, the surfaces of these bones are covered by articular cartilage which creates a smooth, low friction surface that helps the bones glide across each other during movement. The acetabulum has an an additional ring of fibrous cartilage called the labrum, that helps deepen and strengthen the joint. The excessive contact caused by the bony growths can damage the cartilage and labrum, resulting in pain.

The pain associated with FAI is usually insidious and develops gradually over time. It is more common in young and middle-aged adults, especially those with exposure to repetitive and often high impact sports at a young age.
Symptoms of FAI
FAI symptoms commonly include some of the following:
- chronic, deep, or aching anterior groin pain
- motion or position related pain in hip or groin
- clicking, catching, or giving way in hip
- restricted range of motion
- pain may also be felt in back, buttock or thigh
FAI can occur bilaterally, and severity of symptoms do not necessarily correlate with more tissue damage. A thorough evaluation by a Physiotherapist is recommended to assess signs and symptoms, activity history and a physical examination to look for alternate causes of anterior groin pain. If FAI is suspected, a radiograph can be done to confirm the diagnosis.
FAI can be managed conservatively with modification of activities and physiotherapy treatment, taking into account unique patient goals, symptom severity and the impact on daily living.
If you think you might have Femoral Acetabular Impingement, contact us to book an appointment with one of our Physiotherapists today!
Griffin, D. R., et al. "The Warwick Agreement on femoroacetabular impingement syndrome (FAI syndrome): an international consensus statement." British journal of sports medicine 50.19 (2016): 1169-1176.
Palmer, Antony JR, et al. "Arthroscopic hip surgery compared with physiotherapy and activity modification for the treatment of symptomatic femoroacetabular impingement: multicentre randomised controlled trial." bmj 364 (2019).






