Starting over in a new country isn’t easy – especially in your later years. For many refugee seniors, the journey to Canada comes with more than cultural adjustments. It often brings physical pain, limited mobility, and emotional stress. At Triangle Physiotherapy, we understand that healing means more than treating an injury. It’s about restoring comfort, independence, and dignity.
That’s why we’re proud to offer physiotherapy services tailored to the unique needs of refugee seniors living in Oakville and Etobicoke.
The Overlooked Health Needs of Refugee Seniors
Older adults arriving as refugees may face several health challenges:
- Chronic pain from years of physical labor, injury, or untreated conditions
- Limited mobility due to joint stiffness, arthritis, or neurological issues
- Post-traumatic stress or anxiety that impacts movement and daily function
- Lack of access to previous care or rehabilitation in their home country
These factors, combined with language barriers and unfamiliar health systems, often leave many seniors suffering in silence.
How Physiotherapy Can Help

Physiotherapy isn’t just for athletes or people recovering from surgery. For seniors, it’s often the difference between staying active – or becoming dependent.
At Triangle Physiotherapy, we support seniors with:
- Pain relief techniques for arthritis, back pain, and joint issues
- Balance and fall prevention exercises to improve confidence and safety
- Mobility training using walkers, canes, or tailored movement routines
- Gentle strengthening to improve stamina and independence
- Education and support on posture, body mechanics, and safe movement
Whether it’s walking to the grocery store, playing with grandchildren, or simply getting up from a chair with ease – our goal is to help every senior move with less pain and more freedom.
Care That Respects Culture and Communication
We understand that many refugee seniors come from cultures where pain is quietly endured or healthcare is approached differently. Our physiotherapists take time to build trust and communicate with patience and clarity.
We use plain language, visual aids, and interpreter support when needed – ensuring every senior understands their care and feels heard. We believe healing should never be lost in translation.
Accessing Support Through IFHP
Our Oakville and Etobicoke clinics offer care for seniors covered under the Interim Federal Health Program (IFHP). We’ll help guide you or your loved ones through the process – so accessing physiotherapy feels simple, not stressful.
Aging with Dignity
Growing older doesn’t have to mean living in pain or giving up independence. At Triangle Physiotherapy, we stand with our newcomer and refugee communities – offering care that empowers, respects, and uplifts.
If you or a loved one is a refugee senior living with mobility challenges or chronic pain, we’re here to help you take the next step – literally and figuratively.
Contact Triangle Physiotherapy Oakville or Etobicoke to book your first session.
Headaches and migraines are common conditions that can significantly impact quality of life. For many people, these conditions can become chronic, leading to frequent discomfort and reduced quality of life. While medication may provide temporary relief, it often doesn’t address the underlying causes of the pain. This is where physiotherapy comes in. Specifically, those in Etobicoke can benefit from a comprehensive, holistic approach to managing headaches and migraines through physiotherapy.
Understanding the Root Causes of Headaches and Migraines
Headaches and migraines can arise from various factors, including:
- Muscle Tension: Chronic muscle tension in the neck, shoulders, and jaw can contribute to headaches.
- Poor Posture: Poor posture can lead to misalignment of the spine, straining muscles and nerves.
- Stress and Anxiety: Emotional stress can trigger or exacerbate headaches.
- Temporomandibular Joint (TMJ) Disorder: Problems with the jaw joint can cause headaches and facial pain.

How Physiotherapy Can Help
1. Postural Correction
Many headaches are caused by poor posture, particularly when sitting for long periods. Physiotherapists in Etobicoke work on posture correction, educating patients on proper alignment and offering exercises to strengthen muscles that support a healthy posture.
2. Manual Therapy
Manual therapy techniques, such as soft tissue massage, joint mobilizations, and trigger point therapy, can help release muscle tension and improve mobility in the neck and shoulders, reducing the frequency and intensity of headaches.
3. Cervical Spine Alignment
Misalignment in the cervical spine can contribute to headaches and migraines. Physiotherapists in Etobicoke can assess the spine and provide treatments to realign vertebrae, decreasing nerve irritation and reducing headaches.
4. Stress Management Techniques
Stress is a common trigger for both headaches and migraines. Physiotherapy includes relaxation techniques, breathing exercises, and even guided stretches that help reduce stress, promoting relaxation and decreasing the likelihood of headache onset.
5. Exercise Prescription
Targeted exercises strengthen the muscles of the neck, shoulders, and upper back, helping patients develop a more resilient posture and reducing muscle tension that can lead to headaches. Home exercise programs are often prescribed to maintain these benefits between sessions.\
6. Dry Needling
This technique involves inserting thin needles into trigger points, which are areas of muscle tension or knots. Dry needling can help reduce pain and improve muscle function.
FAQs About Physiotherapy for Headaches and Migraines
Can physiotherapy really help with headaches and migraines?
Yes, physiotherapy in Etobicoke offers a holistic treatment plan that addresses the underlying musculoskeletal causes of headaches and migraines, providing relief and helping to prevent future episodes.
How many physiotherapy sessions will I need?
The number of sessions varies based on the severity of your condition and how well your body responds to treatment. Most patients start to notice significant improvements within 4-6 sessions, but a more personalized plan will be created during your assessment.
Do I need a doctor’s referral to see a physiotherapist?
In most cases, you do not need a doctor’s referral to start physiotherapy in Etobicoke for headaches or migraines. However, it’s always a good idea to check with your insurance company.
What can I expect during my first physiotherapy session?
During your initial visit, the physiotherapist will perform a comprehensive assessment, reviewing your medical history, posture, and muscle function. Based on the findings, a tailored treatment plan will be designed to target your specific symptoms.
Headaches and migraines are often a result of underlying musculoskeletal problems, poor posture, and stress. A holistic approach to physiotherapy in Etobicoke not only alleviates the symptoms but also addresses the root causes, offering long-term relief. By working with a trained physiotherapist, you can significantly reduce the frequency and intensity of your headaches and enjoy a higher quality of life.
If you’re tired of dealing with chronic headaches or migraines, consider physiotherapy in Etobicoke as a natural and effective solution to your pain. Reach out to a qualified physiotherapist to begin your journey toward better health and wellness today.
Spinal fusion surgery is a medical procedure used to permanently join two or more vertebrae in the spine, eliminating motion between them. The goal of the surgery is to reduce pain, correct deformities, or improve stability in the spine.
When would I need Spinal Fusion Surgery?
Spinal fusion surgery is typically recommended for various spine conditions, including:
- Degenerative disc disease: When the discs between vertebrae break down, causing pain.
- Spondylolisthesis: When one vertebra slips forward over the one below it.
- Spinal stenosis: Narrowing of the spinal canal, leading to nerve compression.
- Scoliosis: Abnormal curvature of the spine.
- Fractures: Vertebrae that are broken or dislocated.
- Tumors: Removal of tumors that affect spinal stability.
- Infections: Infections that have caused damage to the vertebrae.
When do I start physiotherapy after surgery?
The timing of when to start physiotherapy after spinal fusion surgery depends on several factors, including the specifics of the surgery, the patient’s overall health, and the surgeon’s recommendations.
What does post-surgery rehab involve?
Immediate Postoperative Period (0-6 Weeks)
- Initial Phase: Physiotherapy may start in the hospital within a day or two after surgery. The focus is on gentle movements and exercises to improve circulation and prevent complications.
- Activities:
- Breathing exercises to prevent lung complications.
- Gentle leg movements like ankle pumps to improve blood flow.
- Log rolling technique for safe movement in and out of bed.
- Short, frequent walks to promote circulation and reduce stiffness.
Early Rehabilitation Phase (6-12 Weeks)
- When: Typically, more structured physical therapy begins around 4 to 6 weeks after surgery, depending on the surgeon’s assessment.
- Goals: Gradually increase mobility, start gentle strengthening exercises, and improve functional movements.
- Activities:
- Range of motion exercises.
- Gentle strengthening exercises for the core and lower extremities.
- Walking programs to gradually increase distance and duration.
- Education on proper body mechanics and posture.
Late Rehabilitation Phase (3-6 Months)
- When: Around 3 months post-surgery, assuming there are no complications.
- Goals: Restore full function, enhance strength and endurance, and improve posture and body mechanics.
- Activities:
- More advanced strengthening exercises using resistance bands or light weights.
- Low-impact aerobic exercises like swimming or cycling.
- Balance and coordination exercises.
- Functional training for daily activities.
Long-Term Rehabilitation Phase (6-12 Months)
- When: After 6 months, the patient should continue with physiotherapy based on individual progress and goals.
- Goals: Achieve optimal strength, flexibility, and functional ability, and prevent recurrence of symptoms.
- Activities:
- Progressive resistance training.
- Gradual reintroduction of higher-impact activities, if appropriate.
- Sport-specific training for athletes.
- Ongoing education on maintaining spine health.
Key Points to Consider
- Surgeon’s Recommendations: Always follow the specific guidelines and timelines provided by the surgeon, as they know the details of the surgery and individual patient needs.
- Listen to Your Body: Avoid pushing through pain. Pain is a signal that something might be wrong, and it’s important to communicate any discomfort to the physiotherapist or surgeon.
- Individual Variation: Each patient’s recovery is unique. Factors such as age, overall health, and the complexity of the surgery will influence the timing and intensity of physiotherapy.
Starting physiotherapy at the right time is crucial for a successful recovery, and adhering to a structured rehabilitation program can significantly enhance outcomes after spinal fusion surgery.
Click here to book an appointment for post-surgery rehab with a physiotherapist at one of our eight locations.
- Physiotherapy Etobicoke – Triangle Physiotherapy Etobicoke
- Oakville Physiotherapy Clinic – Triangle Physiotherapy Oakville
- Physiotherapy North York – Triangle Physiotherapy North York
- Mississauga Physiotherapy Clinics – Triangle Physiotherapy Mississauga
- Downtown Physiotherapy Clinics – Triangle Physiotherapy King West
- Uptown Physiotherapy Clinics – Triangle Physiotherapy Lawrence Park
- Physiotherapy Clinic Downtown Toronto – Triangle Physiotherapy Queens Quay
- Physiotherapy Clinics Mississauga – Triangle Physiotherapy Erin Mills
General Information: The information provided on this blog is for general informational purposes only. While we strive to ensure the accuracy and relevance of our content, we make no guarantees about the completeness, reliability, or accuracy of the information.
Not Professional Advice: The content on this blog does not constitute professional advice. It is not a substitute for professional medical, legal, financial, or other professional advice. Always seek the guidance of a qualified professional with any questions you may have regarding your specific situation.
Recovering from spinal fusion surgery requires careful physiotherapy to restore mobility and strength. Whether you need physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, or Liberty Village, there are expert physiotherapists available to guide your recovery journey and help you regain your quality of life.
Hiking is a fantastic way to enjoy the great outdoors and stay fit, but it can also pose some risks. Whether you’re new to hiking or a seasoned backpacker, there are numerous factors to take into account before heading out on the trails. You need to evaluate your backpack’s weight, choose appropriate footwear, plan your food and hydration, check the weather, and map out your routes. Additionally, since hiking often takes you off the beaten path, it’s essential to take precautions against three common hiking injuries: knee pain, ankle sprains, and sore feet.
Is it necessary to warm up before hiking?

Yes, it is necessary to warm up before hiking. Warming up helps prepare your muscles and joints for physical activity, reducing the risk of injury. Here are some reasons why warming up is important before hiking:
Benefits of Warming Up Before Hiking
- Increases Blood Flow: A proper warm-up increases blood flow to your muscles, delivering oxygen and nutrients that help them perform better.
- Enhances Flexibility: Warming up loosens your muscles and increases your range of motion, making it easier to navigate uneven terrain.
- Reduces Injury Risk: Warm muscles are less prone to strains, sprains, and other injuries.
- Prepares Your Heart: Gradually increasing your heart rate helps prepare your cardiovascular system for the more strenuous activity of hiking.
- Improves Performance: A good warm-up can improve your overall performance, making your hike more enjoyable and less exhausting.
What are some effective warm up exercises to do before hiking?
Effective Warm-Up Exercises
- Walking or Light Jogging: Start with 5-10 minutes of brisk walking or light jogging to get your blood flowing.
- Dynamic Stretches: Perform dynamic stretches like leg swings, arm circles, and torso twists to loosen up your muscles and joints.
- Ankle Rotations: Rotate your ankles in circles to prepare them for the uneven terrain.
- Hip Circles: Rotate your hips to loosen the hip joints, which are crucial for hiking.
- Calf Raises: Perform calf raises to warm up your calves, which are heavily used during hiking.
Taking a few minutes to warm up before you start your hike can make a significant difference in your overall hiking experience and help prevent injuries.
What are the most common hiking injuries?
Some of the most common hiking injuries are:
- Knee Pain
- Ankle Sprain
- Foot Pain
Knee Pain when Hiking
Knee pain is a common issue among hikers, especially on longer or more challenging trails. Here’s a comprehensive approach to understanding, preventing, and managing knee pain when hiking:
Causes of Knee Pain While Hiking
- Overuse and Strain: Continuous stress on the knee joint from uphill climbs, downhill descents, or long sessions of hiking.
- Improper Biomechanics: Poor hiking technique, such as improper foot placement or stride, can strain the knee joint.
- Previous Injuries: Past knee injuries or conditions like arthritis can flare up during hiking.
- Improper Gear: Worn-out or inappropriate footwear lacking proper cushioning and support.
Ankle Sprain when Hiking
An ankle sprain can be a painful and frustrating injury, especially when hiking in rugged terrain. Here’s how to understand, prevent, and manage ankle sprains while hiking:
Causes of Ankle Sprains While Hiking
- Uneven Terrain: Stepping on uneven surfaces, rocks, or roots can twist or roll the ankle.
- Fatigue: Muscles that support the ankle can become tired, leading to less stability and increased risk of injury.
- Inadequate Footwear: Wearing shoes or boots without proper ankle support or that are worn out.
Foot Pain when Hiking
Foot pain while hiking can be uncomfortable and distracting. Here’s how to understand, prevent, and manage foot pain effectively:
Causes of Foot Pain While Hiking
- Improper Footwear: Shoes or boots that are too tight, loose, worn out, or lacking proper cushioning and support.
- Overuse or Strain: Prolonged walking or hiking, especially on challenging terrain, can strain the muscles and joints of the feet.
- Blisters: Friction from improperly fitting shoes or moisture buildup can lead to painful blisters.
If you get injured while hiking, consult one of our physiotherapists who can help you with treating the injuries as well as advise and educate you on prevention so you can enjoy your outdoor activities without pain and discomfort.
Click here to book an appointment with a physiotherapist at one of our eight locations.
- Physiotherapy Etobicoke – Triangle Physiotherapy Etobicoke
- Oakville Physiotherapy Clinic – Triangle Physiotherapy Oakville
- Physiotherapy North York – Triangle Physiotherapy North York
- Mississauga Physiotherapy Clinics – Triangle Physiotherapy Mississauga
- Downtown Physiotherapy Clinics – Triangle Physiotherapy King West
- Uptown Physiotherapy Clinics – Triangle Physiotherapy Lawrence Park
- Physiotherapy Clinic Downtown Toronto – Triangle Physiotherapy Queens Quay
- Physiotherapy Clinics Mississauga – Triangle Physiotherapy Erin Mills
A rotator cuff tears are common injuries to the shoulder, involving a tear in one or more of the tendons of the rotator cuff muscles. It is one of the leading causes of shoulder pain and disability. The rotator cuff is a group of four muscles and their tendons that stabilize the shoulder and allow for its wide range of motion.
Understanding Rotator Cuff Tears: Causes and Symptoms
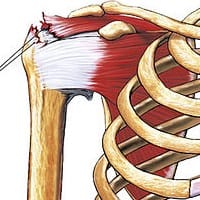
The rotator cuff is a group of four muscles and their tendons that stabilize the shoulder and allow for its wide range of motion. These muscles are:
- Supraspinatus
- Infraspinatus
- Teres minor
- Subscapularis
Types of Rotator Cuff Tears
- Partial Tear: This type of tear damages the tendon but does not completely sever it.
- Complete Tear: Also known as a full-thickness tear, this type involves the tendon being split into two pieces or pulled completely off the bone.
Causes
- Acute Injury: Sudden injuries, such as a fall on an outstretched arm or lifting something heavy with a jerking motion.
- Degenerative Wear and Tear: Gradual wear over time due to aging, repetitive stress from activities (like sports or certain jobs), or poor shoulder mechanics.
Symptoms
- Pain at rest and at night, particularly if lying on the affected shoulder
- Pain when lifting and lowering your arm or with specific movements
- Weakness in the shoulder
- Crackling sensation when moving the shoulder in certain positions
Importance of Physiotherapy in Rotator Cuff Tear Treatment
Physiotherapy plays a crucial role in the treatment and rehabilitation of rotator cuff tears. It can help in several ways, whether as a primary treatment for less severe tears or as a post-surgical rehabilitation strategy for more significant injuries. Here are some key points highlighting the importance of physiotherapy in rotator cuff tear treatment:
Pain Reduction
- Manual Therapy: Techniques such as massage and joint mobilization can help reduce pain and improve shoulder function.
- Modalities: Use of heat, ice, ultrasound, and electrical stimulation can help manage pain and inflammation.
Restoring Range of Motion
- Stretching Exercises: Specific stretches help maintain and gradually improve shoulder flexibility.
- Mobilization Techniques: Gentle mobilization can help increase the range of motion without causing further injury.
Strengthening Shoulder Muscles
- Strengthening Exercises: Focused on the rotator cuff and surrounding muscles, these exercises help restore strength and function to the shoulder.
- Progressive Resistance: Gradual increase in resistance helps to build muscle strength over time.
Improving Shoulder Stability
- Proprioceptive Training: Exercises that improve the body’s ability to sense the position and movement of the shoulder, enhancing stability.
- Functional Training: Exercises tailored to improve stability during daily activities and specific movements required in sports or work.
Enhancing Surgical Outcomes
- Pre-Surgical Physiotherapy (“Prehabilitation”): Strengthening and conditioning the shoulder before surgery can lead to better post-surgical outcomes.
- Post-Surgical Rehabilitation: Structured physiotherapy is essential to restore function, strength, and range of motion after surgery. It also helps minimize scar tissue formation and adhesions.
Preventing Further Injury
- Education: Teaching proper shoulder mechanics and ergonomic principles to avoid movements that can exacerbate the injury.
- Exercise Regimen: Developing a long-term exercise plan to maintain shoulder health and prevent future injuries.
Tailored Rehabilitation Programs
- Individualized Plans: Physiotherapists create personalized treatment plans based on the specific nature of the tear, the patient’s overall health, and their functional goals.
- Goal Setting: Setting realistic and progressive goals to keep the patient motivated and track progress.
Long-Term Shoulder Health
- Maintenance Exercises: Developing a routine of exercises to be continued even after formal physiotherapy ends to maintain shoulder health.
- Lifestyle Modifications: Advice on modifications to daily activities and sports techniques to protect the shoulder.
In summary, physiotherapy is an integral part of the comprehensive management of rotator cuff tears, offering a non-invasive approach to pain relief, functional restoration, and long-term shoulder health. It provides a structured and supportive environment for recovery, whether used alone or in conjunction with surgical treatments.
Click here to book an appointment with a physiotherapist at one of our eight locations.
- Physiotherapy Etobicoke – Triangle Physiotherapy Etobicoke
- Oakville Physiotherapy Clinic – Triangle Physiotherapy Oakville
- Physiotherapy North York – Triangle Physiotherapy North York
- Mississauga Physiotherapy Clinics – Triangle Physiotherapy Mississauga
- Downtown Physiotherapy Clinics – Triangle Physiotherapy King West
- Uptown Physiotherapy Clinics – Triangle Physiotherapy Lawrence Park
- Physiotherapy Clinic Downtown Toronto – Triangle Physiotherapy Queens Quay
- Physiotherapy Clinics Mississauga – Triangle Physiotherapy Erin Mills
“Rotator cuff tears require expert treatment and rehabilitation to restore function and reduce pain. Triangle Physiotherapy offers specialized care across the GTA. Whether you’re seeking Physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, or Liberty Village, our experienced team is here to help you on your recovery journey.”
The choice between physiotherapy and massage therapy depends on your specific needs, goals, and health conditions. Here’s a detailed comparison to help you decide which might be better for you:
Physiotherapy

What it is:
- A healthcare profession focused on diagnosing, managing, and preventing movement disorders.
- Uses exercises, manual therapy, education, and modalities like ultrasound and electrical stimulation.
Benefits:
- Rehabilitation: Effective for recovering from injuries, surgeries, and chronic conditions like arthritis.
- Pain Management: Addresses the root cause of pain through various techniques and exercises.
- Improved Mobility: Helps restore function and movement, particularly after injury or surgery.
- Preventive Care: Offers strategies to prevent future injuries or manage chronic conditions.
- Customized Treatment: Tailors plans based on individual assessments and needs.
Common Conditions Treated:
- Musculoskeletal injuries (e.g., sprains, fractures)
- Neurological conditions (e.g., stroke, multiple sclerosis)
- Cardiopulmonary issues (e.g., chronic obstructive pulmonary disease)
- Post-surgical rehabilitation
Massage Therapy

What it is:
- A practice involving the manipulation of soft tissues (muscles, tendons, ligaments) to enhance well-being.
- Uses techniques like stroking, kneading, and applying pressure.
Benefits:
- Relaxation: Promotes overall relaxation and stress relief.
- Pain Relief: Alleviates muscle tension and pain.
- Improved Circulation: Enhances blood flow, which can aid in healing.
- Flexibility: Increases range of motion and reduces stiffness.
- Mental Health: Can improve mood and reduce symptoms of anxiety and depression.
Common Conditions Treated:
- Muscle tension and soreness
- Stress-related conditions
- Chronic pain (e.g., back pain, fibromyalgia)
- Sports injuries
- Headaches and migraines
Which is Better for You?
- For Injury Rehabilitation or Chronic Conditions:
- Physiotherapy is typically more suitable as it provides a structured approach to recovery, addressing the underlying causes of your condition.
- For Stress Relief and Muscle Tension:
- Massage Therapy can be highly effective if your primary goal is relaxation and relief from muscle tightness.
- For Pain Management:
- Both can be effective, but the choice depends on the cause of the pain. Physiotherapy is often better for pain related to injury or chronic conditions, while massage therapy can be great for muscle-related pain.
- For Improved Mobility and Function:
- Physiotherapy focuses on restoring function and movement, making it the better choice for mobility issues.
- For Preventive Care:
- Physiotherapy provides long-term strategies to prevent injuries and manage chronic conditions.
- For Overall Well-being and Relaxation:
- Massage Therapy is beneficial for enhancing general well-being, reducing stress, and promoting relaxation.
Combination of Both:
- In some cases, a combination of physiotherapy and massage therapy can be beneficial. For example, physiotherapy can address the underlying issues, while massage therapy can help manage symptoms and improve overall well-being.
Conclusion:
Consult with a healthcare professional to get a personalized recommendation based on your specific health needs and goals. They can help you decide the best course of action and whether one or a combination of both therapies is ideal for you.
Click here to book an appointment with a physiotherapist and massage therapist at one of our eight locations.
- Physiotherapy Etobicoke – Triangle Physiotherapy Etobicoke
- Oakville Physiotherapy Clinic – Triangle Physiotherapy Oakville
- Physiotherapy North York – Triangle Physiotherapy North York
- Mississauga Physiotherapy Clinics – Triangle Physiotherapy Mississauga
- Downtown Physiotherapy Clinics – Triangle Physiotherapy King West
- Uptown Physiotherapy Clinics – Triangle Physiotherapy Lawrence Park
- Physiotherapy Clinic Downtown Toronto – Triangle Physiotherapy Queens Quay
- Physiotherapy Clinics Mississauga – Triangle Physiotherapy Erin Mills
Choosing between physiotherapy and massage therapy depends on your specific needs and health goals. Both can be beneficial for pain relief and overall wellness. For those looking for physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, or Liberty Village, there are skilled practitioners available to help you decide the best approach for your situation.
Physiotherapy can be highly beneficial for individuals suffering from knee osteoarthritis (OA) by addressing pain, improving function, and enhancing the overall quality of life.
What is Knee Osteoarthritis (OA)?
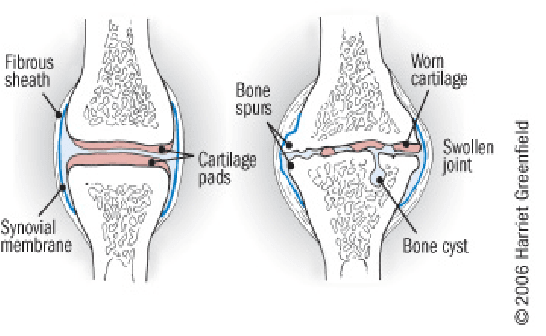
Knee OA is a degenerative joint disease that is typically a result of wear and tear and causes progressive loss of the articular cartilage of the joint.
What are the causes of Knee OA?
Knee osteoarthritis (OA) is a complex condition influenced by a variety of factors. Here are the primary causes and contributing factors:
1. Aging
- Natural Wear and Tear: As people age, the cartilage that cushions the knee joint gradually wears away, leading to OA.
- Decreased Ability to Heal: Older cartilage has a reduced ability to repair itself, making it more susceptible to damage.
2. Genetics
- Family History: Genetic predisposition can play a significant role. If OA runs in your family, you might be more likely to develop it.
- Genetic Mutations: Certain genetic mutations can affect cartilage production and maintenance.
3. Joint Injuries
- Previous Injuries: Injuries such as fractures, ligament tears, or meniscus damage can increase the risk of OA.
- Repetitive Stress Injuries: Repeated stress or overuse of the knee joint, often due to occupational or recreational activities, can lead to OA.
4. Obesity
- Increased Joint Load: Excess body weight puts additional stress on the knee joints, accelerating cartilage breakdown.
- Inflammation: Fat tissue produces inflammatory chemicals that can contribute to joint damage.
5. Mechanical Factors
- Joint Alignment: Abnormal joint alignment, such as bowlegs or knock-knees, can increase stress on certain parts of the knee.
- Muscle Weakness: Weak muscles around the knee, particularly the quadriceps, can lead to increased joint stress.
6. Gender
- Higher Risk in Women: Women, especially those over 50, are more likely to develop knee OA compared to men. Hormonal differences might contribute to this increased risk.
7. Metabolic and Systemic Factors
- Metabolic Syndrome: Conditions like diabetes and metabolic syndrome are associated with an increased risk of OA due to systemic inflammation and metabolic disturbances.
- Inflammatory Diseases: Conditions such as rheumatoid arthritis can predispose individuals to secondary OA.
8. Lifestyle Factors
- Physical Activity: Both excessive and insufficient physical activity can affect joint health. High-impact sports can lead to joint injuries, while sedentary lifestyles can weaken muscles and joints.
- Diet: Poor nutrition can affect joint health. For example, deficiencies in vitamins D and C can impair cartilage maintenance and repair.
9. Joint Biomechanics
- Meniscus Tears: Damage to the meniscus can disrupt joint mechanics and contribute to OA.
- Ligament Damage: Injuries to ligaments, such as the ACL, can destabilize the knee and lead to abnormal wear patterns.
10. Inflammation
- Low-Grade Inflammation: Chronic low-grade inflammation can contribute to the breakdown of cartilage and other joint tissues.
Understanding these causes and contributing factors can help in the prevention and management of knee osteoarthritis, emphasizing the importance of maintaining a healthy lifestyle, avoiding joint injuries, and seeking early intervention for symptoms.
What are the most common symptoms of Knee OA?
Knee osteoarthritis (OA) typically presents with a range of symptoms that can vary in intensity from mild to severe. The most common symptoms include:
1. Pain
- Activity-Related Pain: Pain that worsens with activity or weight-bearing and improves with rest.
- Persistent Pain: Chronic pain that may be present even at rest or during the night in more advanced stages.
2. Stiffness
- Morning Stiffness: Stiffness in the knee that is usually worse in the morning or after periods of inactivity and typically lasts less than 30 minutes.
- Post-Activity Stiffness: Stiffness that occurs after prolonged sitting or resting.
3. Swelling
- Joint Swelling: Swelling around the knee joint due to inflammation or increased production of joint fluid.
- Effusion: Accumulation of excess fluid within the knee joint, leading to noticeable swelling.
4. Reduced Range of Motion
- Limited Flexibility: Difficulty bending or straightening the knee fully.
- Loss of Motion: Progressive decrease in the knee’s range of motion over time.
5. Grinding Sensation (Crepitus)
- Audible Cracking or Popping: A sensation of grinding, cracking, or popping sounds when moving the knee, often due to roughened cartilage surfaces.
6. Weakness or Instability
- Feeling of Giving Way: A sensation that the knee might buckle or give out, often due to muscle weakness or joint instability.
- Muscle Weakness: Weakness in the muscles surrounding the knee, particularly the quadriceps.
7. Deformity
- Joint Deformities: Changes in the shape of the knee joint, such as bowlegged (varus) or knock-kneed (valgus) appearance, due to uneven wear and joint damage.
8. Tenderness
- Joint Tenderness: Tenderness or pain when pressing on or around the knee joint.
9. Functional Impairment
- Difficulty with Activities: Challenges with everyday activities such as walking, climbing stairs, sitting, or standing due to pain and stiffness.
- Reduced Mobility: Decreased ability to perform normal daily activities and exercise.
10. Fatigue
- General Fatigue: Feeling of tiredness and reduced energy levels, often due to chronic pain and sleep disturbances.
These symptoms can significantly impact an individual’s quality of life and ability to perform daily activities. Early recognition and management of knee OA symptoms can help slow disease progression and improve function and comfort.
What are the treatment options for Knee OA?
The number 1 treatment option is conservative management (ie. Patient education, therapeutic exercise, activity modification, weight loss, bracing), surgery should be considered after a conservative approach (talk to your orthopaedic specialist for more information).
Physiotherapy can help by providing you with education about osteoarthritis, tailor an exercise program that is suitable for you, help you consider the best options for activity modifications, provide you with education on bracing, address psychosocial factors such as fear-avoidance, promote patient autonomy and get you back to doing the things you love to do!
Manual therapy- joint mobilization to help with stiffness. Muscle energy technique to help stretch surrounding muscles.
Modalities – heat/ice for pain relief, TENs/IFC for pain relief and inflammation control. Ultrasound for pain relief.
Exercises – help with improving mobility, ROM, strength, balance, aerobic capacity, promoting physical function, reducing knee pain and inflammation.
Click here to book an appointment with a physiotherapist at one of our eight locations.
- Physiotherapy Etobicoke – Triangle Physiotherapy Etobicoke
- Oakville Physiotherapy Clinic – Triangle Physiotherapy Oakville
- Physiotherapy North York – Triangle Physiotherapy North York
- Mississauga Physiotherapy Clinics – Triangle Physiotherapy Mississauga
- Downtown Physiotherapy Clinics – Triangle Physiotherapy King West
- Uptown Physiotherapy Clinics – Triangle Physiotherapy Lawrence Park
- Physiotherapy Clinic Downtown Toronto – Triangle Physiotherapy Queens Quay
- Physiotherapy Clinics Mississauga – Triangle Physiotherapy Erin Mills
Physiotherapy can be a highly effective treatment for managing knee osteoarthritis by improving mobility, reducing pain, and enhancing overall function. Whether you are looking for physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, or Liberty Village, there are experienced physiotherapists ready to help you manage osteoarthritis and improve your quality of life.
Physiotherapy and chiropractic care are both forms of manual therapy that focus on the treatment of musculoskeletal issues, but they have different approaches, philosophies, and techniques. Here’s a comparison of the two:
Physiotherapy
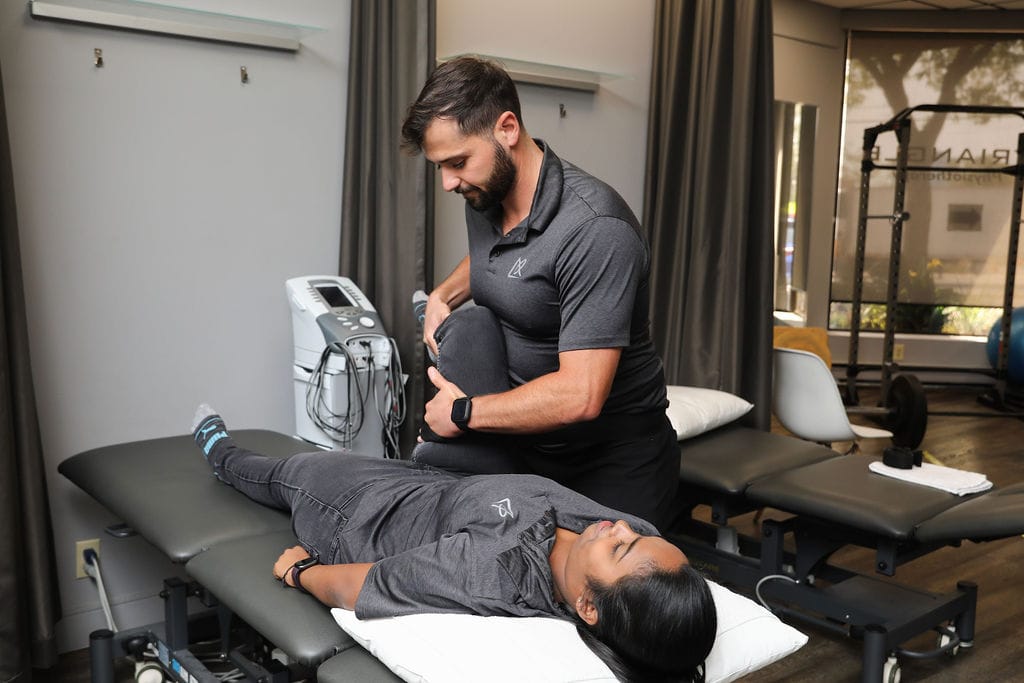
Approach:
- Holistic and comprehensive treatment aimed at restoring movement and function.
- Utilizes evidence-based practices.
Philosophy:
- Focuses on the body as a whole and treats a wide range of conditions, including musculoskeletal, neurological, and cardiovascular issues.
- Emphasizes rehabilitation, prevention, and overall well-being.
Techniques:
- Exercises and stretches to improve mobility and strength.
- Manual therapy, including massage and mobilization of joints.
- Electrotherapy, ultrasound, and other modalities for pain relief and inflammation reduction.
- Education and advice on posture, ergonomics, and lifestyle changes.
Conditions Treated:
- Musculoskeletal pain (e.g., back, neck, shoulder).
- Post-operative rehabilitation.
- Sports injuries.
- Pelvic Health
- Cancer Rehab
- Vestibular Conditions
- Neurological disorders (e.g., stroke, Parkinson’s disease).
- Chronic conditions (e.g., arthritis).
Qualifications:
- Requires a degree in physiotherapy and registration with provincial regulatory body.
- Involves extensive training in anatomy, physiology, and pathology.
Chiropractic

Approach:
- Primarily focuses on the diagnosis and treatment of mechanical disorders of the spine.
- Utilizes spinal adjustments and manipulations.
Philosophy:
- Based on the principle that spinal health affects overall health and well-being.
- Emphasizes the relationship between the spine and nervous system.
Techniques:
- Spinal manipulations and adjustments to restore joint function and support the nervous system.
- Manual adjustments often performed with a high-velocity thrust.
- May include advice on exercise, diet, and lifestyle.
Conditions Treated:
- Back and neck pain.
- Headaches and migraines.
- Joint pain (e.g., hips, knees).
- Sciatica and other nerve-related issues.
Qualifications:
- Requires a Doctor of Chiropractic (DC) degree and registration with provincial regulatory body.
- Involves training in anatomy, physiology, and specialized chiropractic techniques.
Key Differences between Physiotherapy and Chiropractic
- Scope of Practice:
- Physiotherapists: Treat a broader range of conditions affecting various body systems.
- Chiropractors: Primarily focus on spinal health and its impact on overall health but can also treat other musculoskeletal conditions.
- Techniques Used:
- Physiotherapists: Employ a wide variety of techniques including exercise, manual therapy, and electrotherapy.
- Chiropractors: Primarily use spinal adjustments and manipulations but are also trained in treating other joints.
- Philosophical Focus:
- Physiotherapists: Emphasize holistic rehabilitation and prevention.
- Chiropractors: Emphasize the importance of spinal alignment for overall health.
- Educational Path:
- Physiotherapists: Typically require a Bachelor’s or Master’s degree in physiotherapy.
- Chiropractors: Require a Doctor of Chiropractic degree.
When to Choose Each
- Physiotherapy: Suitable for a wide range of conditions, particularly when rehabilitation, exercise, and a holistic approach are needed.
- Chiropractic Care: Beneficial for conditions specifically related to spinal health and when spinal adjustments are indicated.
Ultimately, the choice between physiotherapy and chiropractic care may depend on the specific condition being treated, the patient’s preferences, and the recommendations of healthcare professionals. In some cases, a combination of both therapies might be the most effective approach.
Click here to book an appointment with a physiotherapist or chiropractor at one of our eight locations.
- Physiotherapy Etobicoke – Triangle Physiotherapy Etobicoke
- Oakville Physiotherapy Clinic – Triangle Physiotherapy Oakville
- Physiotherapy North York – Triangle Physiotherapy North York
- Mississauga Physiotherapy Clinics – Triangle Physiotherapy Mississauga
- Downtown Physiotherapy Clinics – Triangle Physiotherapy King West
- Uptown Physiotherapy Clinics – Triangle Physiotherapy Lawrence Park
- Physiotherapy Clinic Downtown Toronto – Triangle Physiotherapy Queens Quay
- Physiotherapy Clinics Mississauga – Triangle Physiotherapy Erin Mills
Deciding between physiotherapy and chiropractic care depends on your specific needs and conditions. Both can offer significant benefits for pain management and overall health. If you are considering physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, or Liberty Village, there are expert physiotherapists available to guide you toward the best treatment approach for your unique situation.
Working and studying from home can take a toll on your body and mind, making it crucial to incorporate some daily movement. Simple actions like walking around your workspace while on a call or standing up while having a snack can help reduce sedentary behavior. Additionally, daily stretching can prevent issues such as “tech neck” and back pain.
How often should you stretch working from home?
When working from home, it’s beneficial to stretch regularly to prevent stiffness and discomfort. Here are some general recommendations:
- Every 30-60 Minutes: Aim to take a short break to stand up, move around, and do some stretches. This helps prevent prolonged periods of inactivity and reduces the risk of musculoskeletal issues.
- Mini Breaks: Take a few minutes every hour to do some simple stretches or walk around. This can help improve circulation and reduce muscle tension.
- Daily Stretching Routine: Incorporate a more comprehensive stretching routine at least once a day, focusing on areas prone to tension such as the neck, shoulders, back, and hips.
By following these guidelines, you can maintain flexibility, reduce the risk of pain, and improve overall well-being while working from home.
What stretches can I do at my desk?
Tricep Stretch
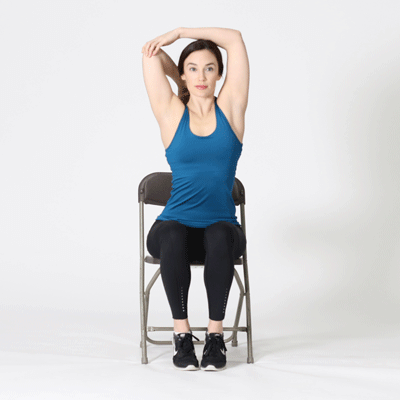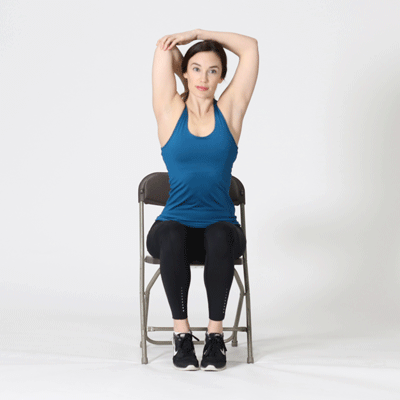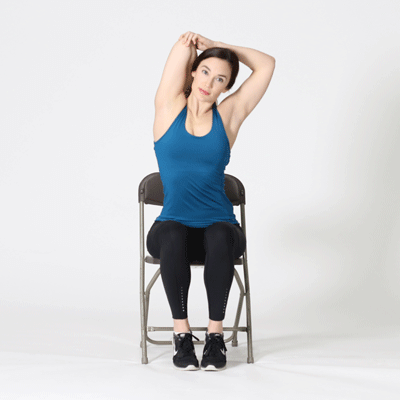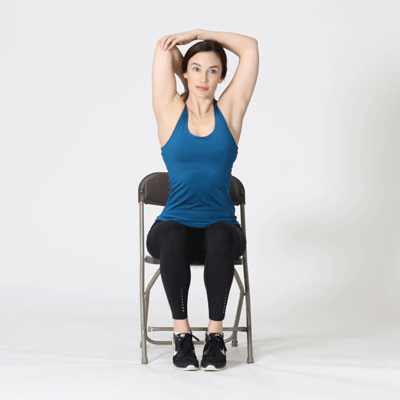
Neck Stretch

Upper Body and Arm Stretch

Trunk Rotation Stretch

Shoulder Shrug Stretch

Stretch Courtesy: https://uwaterloo.ca/campus-wellness/blog/post/desk-stretches
If you are experiencing persistent neck pain, back pain or discomfort, it is advisable to consult a physiotherapist, for proper evaluation and guidance.
Click here to book an appointment with a physiotherapist at one of our eight locations.
- Physiotherapy Etobicoke – Triangle Physiotherapy Etobicoke
- Oakville Physiotherapy Clinic – Triangle Physiotherapy Oakville
- Physiotherapy North York – Triangle Physiotherapy North York
- Mississauga Physiotherapy Clinics – Triangle Physiotherapy Mississauga
- Downtown Physiotherapy Clinics – Triangle Physiotherapy King West
- Uptown Physiotherapy Clinics – Triangle Physiotherapy Lawrence Park
- Physiotherapy Clinic Downtown Toronto – Triangle Physiotherapy Queens Quay
- Physiotherapy Clinics Mississauga – Triangle Physiotherapy Erin Mills
Incorporating simple stretches into your routine can help reduce back pain when working from home. For personalized guidance, you can seek physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, or Liberty Village, where experienced physiotherapists can create a tailored plan to support your back health and overall well-being.
Physiotherapy is often recommended before considering surgery for a variety of musculoskeletal conditions and injuries. The decision to try physiotherapy before surgery depends on several factors, including the nature and severity of the condition, the patient’s overall health, and the specific goals of treatment.
What are some of the scenarios where physiotherapy is considered before surgery?
Here are some common scenarios where physiotherapy is advised before opting for surgery:
- Chronic Pain Management:
- Conditions like chronic back pain, neck pain, or osteoarthritis can often be managed with physiotherapy. Techniques such as exercise, manual therapy, and education can help reduce pain and improve function.
- Rehabilitation after Injury:
- For injuries such as sprains, strains, and minor fractures, physiotherapy can aid in healing and restore mobility and strength without the need for surgical intervention.
- Degenerative Joint Diseases:
- For conditions like osteoarthritis, physiotherapy can help maintain joint function, improve strength, and reduce pain, potentially delaying or avoiding the need for joint replacement surgery.
- Sports Injuries:
- Many sports-related injuries, including tendonitis, ligament sprains, and muscle tears, can be effectively treated with physiotherapy. Rehabilitation programs can restore function and allow a safe return to activity.
- Postural and Muscular Imbalances:
- Conditions resulting from poor posture or muscular imbalances, such as certain types of shoulder impingement or knee pain, can often be corrected through targeted physiotherapy exercises and manual therapy.
- Non-Surgical Management of Disc Herniations:
- In cases of herniated discs causing back or neck pain, physiotherapy can help reduce symptoms through specific exercises and modalities, sometimes avoiding the need for surgical intervention.
- Rehabilitation of Neurological Conditions:
- For certain neurological conditions like stroke, multiple sclerosis, or Parkinson’s disease, physiotherapy plays a crucial role in managing symptoms and improving quality of life.
- Post-Surgical Rehabilitation:
- In cases where surgery is eventually necessary, pre-surgical physiotherapy (prehabilitation) can help strengthen the body, improve overall fitness, and enhance recovery post-surgery.
- Conservative Management First:
- For many conditions, especially those where surgery carries significant risks or has variable outcomes, conservative management with physiotherapy is often the first line of treatment to try less invasive options.
What are the benefits of trying physiotherapy before opting for surgery?
Trying Physiotherapy Oakville before opting for surgery offers numerous benefits, both physical and psychological. Here are some key advantages:
Physical Benefits of Physiotherapy
- Pain Reduction:
- Physiotherapy can effectively reduce pain through various techniques such as manual therapy, exercises, and modalities like heat or cold therapy, electrical stimulation, and ultrasound.
- Improved Mobility and Function:
- Targeted exercises and stretches can help improve range of motion, strength, and overall functional ability, allowing patients to perform daily activities with greater ease.
- Enhanced Healing and Recovery:
- Physiotherapy promotes natural healing by improving blood flow, reducing inflammation, and preventing further injury through proper movement patterns.
- Strengthening and Stabilization:
- Physiotherapists design personalized exercise programs to strengthen muscles and stabilize joints, which can prevent the need for surgery by addressing the underlying causes of pain and dysfunction.
- Injury Prevention:
- By improving posture, body mechanics, and muscle balance, physiotherapy can reduce the risk of future injuries.
- Management of Chronic Conditions:
- For chronic conditions like osteoarthritis, physiotherapy can help manage symptoms and slow the progression of the disease, potentially delaying or avoiding the need for surgery.
Psychological and Emotional Benefits
- Reduced Anxiety and Stress:
- The prospect of surgery can be daunting. Physiotherapy offers a non-invasive approach that can alleviate anxiety and stress related to surgical procedures and recovery.
- Increased Confidence and Empowerment:
- Patients often feel more in control of their health when actively participating in their treatment through physiotherapy, leading to improved mental well-being.
- Better Understanding of Condition:
- Physiotherapists educate patients about their condition and the mechanics of their body, providing them with knowledge and strategies to manage their symptoms effectively.
Economic and Practical Benefits
- Cost-Effective:
- Physiotherapy is generally less expensive than surgery and associated hospital stays, making it a cost-effective alternative for many patients.
- Reduced Recovery Time:
- While surgery often requires significant recovery time, physiotherapy allows patients to continue their daily activities with minimal interruption, enhancing their quality of life.
- Avoiding Surgical Risks:
- Surgery carries inherent risks such as infection, complications from anesthesia, and prolonged recovery periods. Physiotherapy avoids these risks by offering a non-invasive treatment option.
- Trial of Conservative Management:
- Trying physiotherapy first allows for the possibility that conservative management might be sufficient. If it proves ineffective, surgery can still be considered as a subsequent option.
Long-term Health Benefits
- Development of Healthy Habits:
- Physiotherapy encourages the adoption of healthy habits and exercises that can contribute to long-term well-being and prevent future issues.
- Maintenance of Physical Fitness:
- Ongoing physiotherapy helps maintain physical fitness, flexibility, and strength, contributing to overall health and resilience against other potential health issues.
Click here to book an appointment with a physiotherapist at one of our eight locations.
- Physiotherapy Etobicoke – Triangle Physiotherapy Etobicoke
- Oakville Physiotherapy Clinic – Triangle Physiotherapy Oakville
- Physiotherapy North York – Triangle Physiotherapy North York
- Mississauga Physiotherapy Clinics – Triangle Physiotherapy Mississauga
- Downtown Physiotherapy Clinics – Triangle Physiotherapy King West
- Uptown Physiotherapy Clinics – Triangle Physiotherapy Lawrence Park
- Physiotherapy Clinic Downtown Toronto – Triangle Physiotherapy Queens Quay
- Physiotherapy Clinics Mississauga – Triangle Physiotherapy Erin Mills
Trying physiotherapy before opting for surgery can be a beneficial step in managing pain and improving function. If you’re considering this approach, you can find expert physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, or Liberty Village to help you explore non-surgical options and make informed decisions about your health.