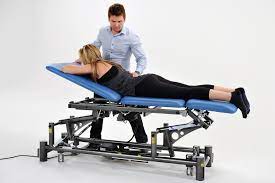
Ankle pain can be a major hindrance to our daily activities, making it difficult to walk, run, or even stand for extended periods. Whether it’s due to an injury, chronic condition, or overuse, finding effective solutions to alleviate ankle pain is crucial for restoring mobility and strength. In this article, we will explore some expert tips on effective physiotherapy exercises for ankle pain, aiming to not only relieve discomfort but also enhance the overall function of your ankle. So, if you’re looking for ways to regain control over your ankle health, keep reading to discover these useful exercises and start your journey towards pain-free movement.
Understanding Ankle Pain: Causes and Symptoms
Ankle pain can be a debilitating condition that affects individuals of all ages, from young athletes to the elderly. Understanding the causes and symptoms of ankle pain is crucial in order to find relief and prevent further injury.
The symptoms of ankle pain can vary depending on the underlying cause. Common symptoms include swelling, tenderness, and stiffness. Individuals may also experience difficulty walking or bearing weight on the affected ankle. In some cases, ankle pain can be accompanied by bruising or a visible deformity.
Understanding the causes and symptoms of ankle pain is the first step towards finding relief and restoring functionality. By seeking proper diagnosis and following the guidance of healthcare professionals, individuals can benefit from effective physiotherapy exercises for ankle pain.
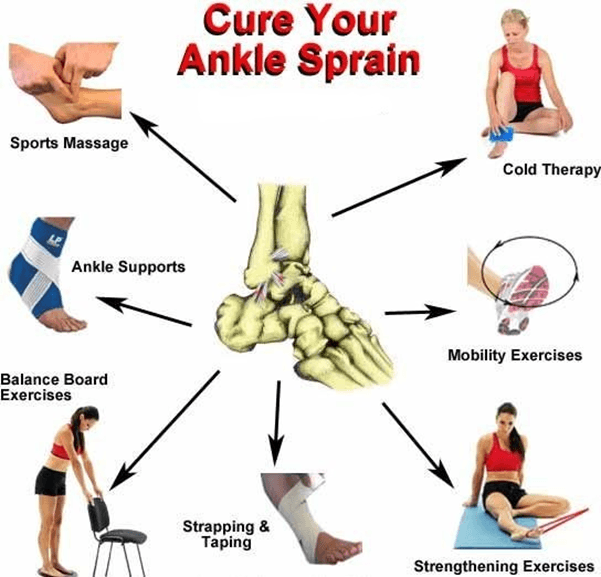
Importance of Physiotherapy in Ankle Pain Management
Physiotherapy plays a crucial role in the management of ankle pain. With the help of effective physiotherapy exercises specifically tailored to target the ankle, individuals can experience improvements in pain.
A key aspect of physiotherapy for ankle pain is restoring mobility. Through a range of exercises and techniques, physiotherapists work to increase the flexibility and motion of the ankle joint. These exercises may include stretching, range of motion exercises, and manual therapy techniques.
In addition to mobility, physiotherapy also focuses on enhancing the strength of the ankle muscles. Strengthening exercises, such as calf raises, ankle circles, and resistance band exercises, are often prescribed to improve the stability and support around the ankle joint. Stronger muscles can effectively help in absorbing shock and preventing further injuries.
Key Principles of Physiotherapy Exercises for Ankle Pain Relief
Physiotherapy Oakville exercises play a crucial role in providing relief from ankle pain. By incorporating specific exercises into a comprehensive treatment plan, individuals can restore mobility and strengthen their ankles, ultimately alleviating pain and preventing future injuries.
One key principle of effective physiotherapy exercises for ankle pain relief is restoring flexibility. Gentle stretches and range-of-motion exercises can help increase the flexibility of the ankle joint, which in turn improves overall joint function. Flexibility exercises may include ankle circles, toe curls, and calf stretches.
Additionally, proprioception exercises are integral to the rehabilitation process. Proprioception refers to the body’s ability to perceive its position in space. After an ankle injury, this sense may be disrupted, leading to balance issues and an increased risk of falls. Incorporating exercises that challenge balance and proprioception, such as standing on one foot or using a wobble board, can greatly improve overall stability and reduce ankle pain.
For optimal results and to ensure you are performing the exercises correctly, it is recommended to consult with your physiotherapist at Physiotherapy Oakville throughout your rehabilitation journey.
Strengthening Exercises for Ankle Stability and Support
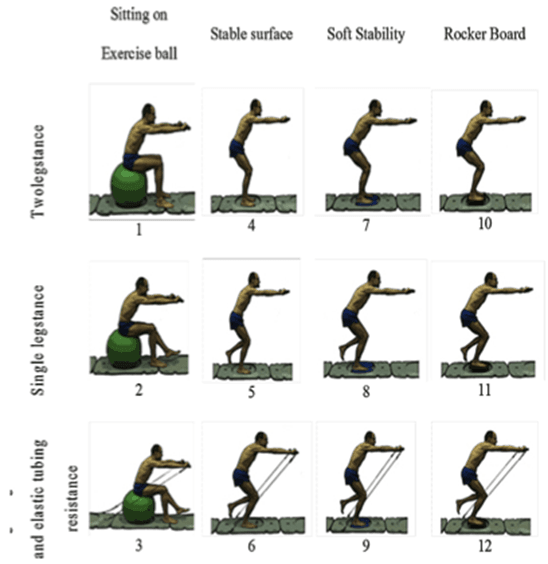
If you’re someone who has experienced ankle pain or instability, you understand the importance of having strong and stable ankles. Whether you’re an athlete or simply want to prevent injuries, implementing effective physiotherapy exercises for ankle pain is essential for restoring mobility and strength.
One of the most effective exercises for improving ankle stability is the single-leg balance. This exercise involves standing on one leg and maintaining your balance for a set amount of time. Not only does this exercise strengthen the muscles surrounding your ankle, but it also improves proprioception, which is your body’s ability to sense its position in space. By practicing this exercise regularly, you can enhance your ankle stability and prevent future injuries.
Lastly, calf raises are a great exercise to target the muscles in your lower leg, including those surrounding your ankle. Stand with your feet hip-width apart and lift your heels off the ground as high as possible, then slowly lower them back down. This exercise specifically targets the gastrocnemius and soleus muscles, which play a significant role in ankle stability and support.
Neuromuscular Exercises for Pain Management and Prevention
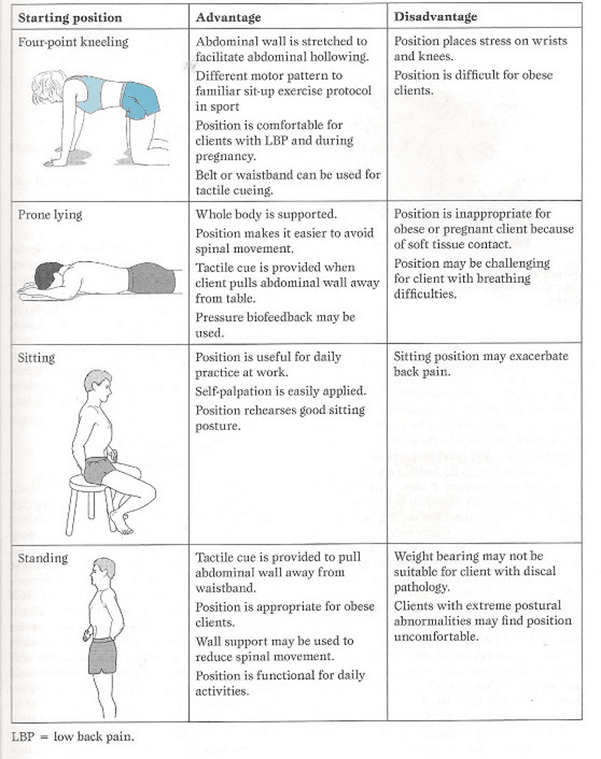
Neuromuscular exercises are gaining popularity in the field of pain management and prevention. These exercises focus on strengthening the connection between the nervous system and the muscles, helping to alleviate pain and improve overall mobility. One area where these exercises have shown promise is in the treatment of ankle pain.
Effective physiotherapy exercises for ankle pain involve restoring mobility and strength to the affected area. These exercises may include ankle stretches, balance training, and resistance exercises. The goal is to target the specific muscles and ligaments surrounding the ankle joint, improving stability and range of motion.
Another exercise that can be beneficial is heel raises. This exercise involves standing on the edge of a step or curb and raising your heels as high as possible. This works the muscles in your calves, which can help support and stabilize the ankle joint.
Resistance band exercises are also effective in strengthening the ankle. These exercises involve using a resistance band to provide resistance during ankle movements, such as flexion, extension, inversion, and eversion. These movements help to target and strengthen the muscles that support the ankle joint.
Progressive Resistance Training for Ankle Strength and Functionality
Progressive resistance training is a highly beneficial approach for improving ankle strength and functionality. Whether you’re recovering from an injury or simply looking to enhance your athletic performance, incorporating effective physiotherapy exercises for ankle pain is crucial for restoring mobility and strength.
One of the most effective exercises for ankle strength is the calf raise. This exercise targets the muscles in the calves and ankles, helping to build strength and stability. Begin by standing with your feet hip-width apart, and then slowly rise onto the balls of your feet. Hold this position for a few seconds before slowly lowering your heels back down. To intensify the exercise, try performing it on a step, allowing your heels to drop below the level of the step before rising back up.
Another great exercise for ankle strength is the ankle dorsiflexion exercise. This exercise focuses on strengthening the muscles that enable you to flex your ankles upwards. Sit on a chair with your feet flat on the ground and place a resistance band around the ball of your foot. While keeping your heel on the ground, slowly pull your toes towards you against the resistance of the band. Hold for a few seconds and then release. Repeat this movement for several repetitions, gradually increasing the resistance as you progress.
Additionally, incorporating balance and proprioception exercises into your progressive resistance training routine can further enhance ankle strength and functionality. Exercises like single-leg stance or standing on an unstable surface, such as a balance board or foam pad, can help improve your body’s awareness of its position in space and challenge the stabilizing muscles around the ankle.
Incorporating Stretching and Flexibility Exercises in Your Routine
Incorporating stretching and flexibility exercises into your daily routine is essential not only for athletes but for anyone looking to improve their overall fitness and well-being.
The first step towards addressing ankle pain and improving flexibility is to consult with a physiotherapist who can assess your specific needs and design a personalized exercise plan. Common exercises used in physiotherapy for ankle pain include calf stretches, ankle rotations, and plantar fascia stretches. These exercises target the muscles and ligaments surrounding the ankle, increasing flexibility and reducing pain.
Tips for Safely Performing Physiotherapy Exercises for Ankle Pain
If you’re suffering from ankle pain and looking for effective ways to restore mobility and strength, physiotherapy exercises can be extremely beneficial. However, it’s important to approach these exercises with caution and prioritize safety to avoid further injury. Here are some tips to help you safely perform physiotherapy exercises for ankle pain.
First and foremost, always consult a professional physiotherapist before starting any exercise routine. They can assess your condition and recommend specific exercises that are best suited for your individual needs. This will ensure that you’re performing the right exercises and avoiding any that may exacerbate your pain.
It’s crucial to start slow and gradually progress as your ankle gains strength and flexibility. Avoid pushing yourself too hard or performing exercises that cause excessive pain. Remember to listen to your body and give it time to heal. Taking breaks in between exercises and giving yourself time for rest and recovery is equally important.
Conclusion
Don’t let these physical conditions ever ride on you. You can consult any of our locations of Triangle Physiotherapy or simply Book An Appointment online.
“Ankle pain can be managed effectively with the right physiotherapy exercises. At Triangle Physiotherapy, we provide expert care across the GTA, including Physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, and Liberty Village. Our experienced physiotherapists are here to help you regain strength and mobility in your ankles.”
Whether you’re a seasoned marathon runner or a casual jogger, incorporating strength and flexibility exercises into your training routine is crucial for improving performance, preventing injuries and enhancing overall strength and endurance. As a runner, you rely on your muscles and joints to propel you forward mile after mile, making it essential to maintain balance, strength, and mobility throughout your body. To help you reach your running goals and stay injury-free, we’ve compiled a list of the top 10 best exercises for runners and put them in the following categories:
Strength-building and injury-prevention exercises
Strength Training
Strength training is crucial for runners as it helps improve muscle strength and endurance, enhances running capacity, and reduces the risk of injury. These exercises target major muscle groups, including squats, lunges, deadlifts, calf raises, and core exercises such as planks and bridges.
Hip Strengthening Exercises
Strong hips are essential for maintaining proper running form and preventing injuries such as hip raises, clamshells, lateral leg raises, and hip abduction/adduction exercises.
Dynamic Warm-Up Exercises
Dynamic warm-up exercises for runners help increase blood flow, improve flexibility, and prepare the muscles for running. These include movements such as leg swings, high knees, butt kicks, lunges with a twist, and leg circles.
Plyometric Exercises
Plyometric exercises help develop power and explosive strength, which can improve running speed and efficiency like box jumps, jump squats, bounding, and skipping.
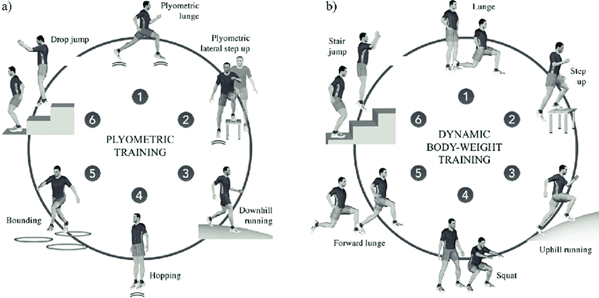
Balance and Stability Exercises
Improving balance and stability can enhance running efficiency and reduce the risk of falls and injuries with exercises like single-leg squats and stability ball exercises.
Flexibility and Mobility Work
Maintaining good flexibility and mobility is important for preventing muscle tightness and reducing the risk of injury with stretching exercises for major muscle groups such as leg swings and hip circles.
Cross-Training
Cross-training activities such as cycling, swimming, and yoga can complement running by providing low-impact cardio, and targeting different muscle groups.
Recovery Exercises
Include exercises focused on recovery, such as foam rolling and gentle stretching, to help alleviate muscle soreness and promote faster recovery between runs.
Injury Prevention Exercises
It is important to pay attention to areas prone to injury for runners, such as the IT band, Achilles tendon, and shin muscles. Runners should Perform exercises specifically targeting these areas, such as IT band stretches, calf raises, and shin strengthening exercises.
Postural Exercises
Maintaining proper posture while running is important for efficiency and injury prevention. This means Incorporating exercises that target postural muscles, including rows, shoulder blade squeezes, and chest stretches.
Recommended Exercises For Runners
- Squats: Squats are a powerhouse, compound exercise for runners, targeting the quadriceps, hamstrings, glutes, and core muscles. By strengthening these muscles, squats improve running efficiency, power, and stability, helping you maintain proper form and reduce the risk of injury.
- Lunges: Lunges are excellent for building lower body strength and stability, particularly in the quadriceps, hamstrings, glutes, and calves. They also help improve balance and coordination, essential for navigating uneven terrain during runs.
- Planks: Planks are a staple core exercise that helps strengthen the entire core, including the abdominals, obliques, and lower back muscles. A strong core is essential for maintaining proper running posture and stability, reducing the risk of lower back pain and other injuries.
- Hip Flexor Stretch: Runners often have tight hip flexors due to the repetitive motion of running. Hip flexor stretches help alleviate tightness and improve hip mobility, allowing for a more fluid and efficient running stride.
- Glute Bridges: Glute bridges target the gluteal muscles, which play a crucial role in running propulsion and stability. Strengthening the glutes helps improve running power and reduces the risk of common injuries like IT band syndrome and knee pain.
- Calf Raises: Calf raises strengthen the calf muscles, which are heavily involved in the push-off phase of running. Strong calves help generate power and speed while reducing the risk of calf strains and Achilles tendon injuries.
- Single-Leg Deadlifts: Single-leg deadlifts are excellent for improving balance, stability, and hamstring strength. They also help correct muscle imbalances between the left and right legs, reducing the risk of overuse injuries.
- Side Leg Raises: Side leg raises target the hip abductor muscles, which are essential for stabilizing the pelvis during running. Strengthening these muscles helps prevent knee valgus (inward collapse) and IT band syndrome.
- Back Extensions: Back extensions strengthen the lower back muscles, which are crucial for maintaining proper posture and spinal alignment during running. A strong lower back helps reduce the risk of back pain and improves running efficiency.
- Foam Rolling: Foam rolling is an effective way to release tight muscles and fascia, improve blood flow, and reduce muscle soreness after running. Incorporating foam rolling into your routine can help prevent injuries and improve overall recovery.
By Incorporating these top 10 best exercises for runners into your training routine, you can enhance your running performance, prevent injuries, and improve overall strength, flexibility, and endurance. Remember to start slow, listen to your body, focus on proper form, and gradually increase intensity and volume as your strength and endurance improve. Consult with a Physiotherapist or ask for GAIT Analysis if you have any concerns or specific training goals.
Happy running!
How do I book an appointment with a physiotherapist near me?
Click HERE to book an appointment with a physiotherapist or chiropractor at one of our eight locations.
- Physiotherapy Etobicoke – Triangle Physiotherapy Etobicoke
- Oakville Physiotherapy Clinic – Triangle Physiotherapy Oakville
- Physiotherapy North York – Triangle Physiotherapy North York
- Mississauga Physiotherapy Clinics – Triangle Physiotherapy Mississauga
- Downtown Physiotherapy Clinics – Triangle Physiotherapy King West
- Uptown Physiotherapy Clinics – Triangle Physiotherapy Lawrence Park
- Physiotherapy Clinic Downtown Toronto – Triangle Physiotherapy Queens Quay
- Physiotherapy Clinics Mississauga – Triangle Physiotherapy Erin Mills
Incorporating the right exercises into your routine can help improve your running performance and prevent injuries. If you’re looking for professional support, consider physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, or Liberty Village. Expert physiotherapists in these locations can create tailored exercise programs to enhance your strength, flexibility, and endurance as a runner.
Frozen shoulder, also known as adhesive capsulitis, is a condition characterized by stiffness and pain in the shoulder joint. It can significantly limit range of motion and impact daily activities. While it can be a challenging condition to manage, there are exercises and tips that can help provide relief and improve mobility. In this article, we’ll explore some easy exercises and practical tips for alleviating frozen shoulder symptoms.
Understanding Frozen Shoulder
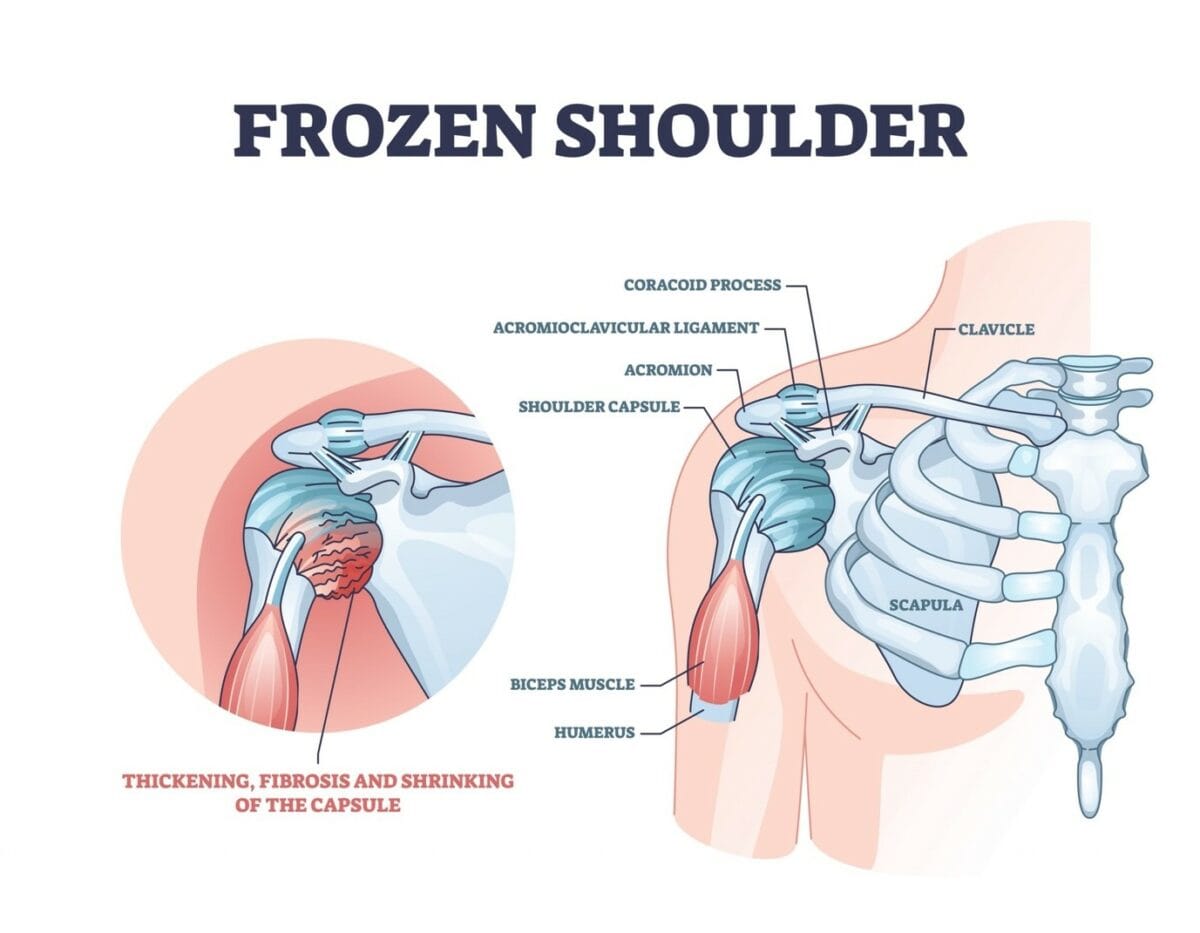
Before diving into exercises and tips, let’s briefly understand what frozen shoulder is. Frozen shoulder occurs when the connective tissue surrounding the shoulder joint becomes inflamed and thickened, leading to stiffness and reduced mobility. The exact cause is often unknown, but factors such as injury, surgery, prolonged immobility, or underlying medical conditions can contribute to its development.
Frozen shoulder typically develops gradually and progresses through three stages:
- Freezing Stage: During this initial stage, individuals experience increasing shoulder pain and stiffness. Range of motion becomes limited, making it difficult to perform daily activities such as reaching overhead or behind the back.
- Frozen Stage: In the frozen stage, shoulder stiffness and pain may plateau, but the range of motion remains significantly restricted. Activities that require lifting or rotating the arm may be particularly challenging, and pain may persist, especially at night.
- Thawing Stage: The thawing stage is characterized by a gradual improvement in shoulder mobility and a reduction in pain. Range of motion gradually returns to normal or near-normal levels over time, although this process can take several months to years.
Easy Exercises for Frozen Shoulders
Pendulum Stretch
This exercise helps loosen the shoulder joint and improve range of motion.
- Stand or sit with your unaffected arm supported on a table or chair.
- Lean forward slightly and let your affected arm hang down.
- Gently swing your arm in small circles, forward and backward, for 5-10 minutes.
- Perform 10-15 circles in each direction gradually increasing the range of motion
Towel Stretch
This stretch targets the shoulder capsule and helps improve flexibility.
- Hold a towel behind your back with one hand and grab the other end with your opposite hand.
- Gently pull the towel upward with your top hand while gently pushing downward with your bottom hand.
- Hold the stretch for 15-30 seconds, then relax.
- Repeat several times, gradually increasing the stretch as tolerated.
Wall Walk
This exercise helps stretch the shoulder muscles and increase range of motion.
- Stand facing a wall with your fingertips touching the wall at waist height.
- Slowly walk your fingers up the wall, raising your arm as high as possible without causing pain.
- Hold the stretch for a few seconds, then walk your fingers back down.
- Repeat for 5-10 repetitions, gradually increasing the height as your mobility improves.
Cross-Body Stretch
- Use your unaffected arm to gently pull the affected arm across your body.
- Hold the stretch for 15-30 seconds, feeling a gentle stretch in the shoulder.
- Repeat on the other side.
- Perform 2-3 sets on each side, alternating between arms.
Practical Tips for Managing Frozen Shoulders:
- Apply Heat: Using a heating pad or warm towel on the affected shoulder can help relax tight muscles and increase blood flow, reducing stiffness and discomfort.
- Practice Good Posture: Maintaining proper posture throughout the day can prevent further strain on the shoulders and promote better alignment and mobility.
- Avoid Overuse: Be mindful of activities that aggravate shoulder pain and limit repetitive movements or heavy lifting that could worsen symptoms.
- Stay Active: While rest is important for healing, gentle exercise and movement can help prevent stiffness and promote recovery. Incorporate low-impact activities like walking or swimming into your routine.
- Seek Professional Help: If symptoms persist or worsen despite home remedies, consider seeking guidance from a healthcare professional or a physical therapist.
While frozen shoulder can be a frustrating and painful condition, incorporating easy exercises and practical tips into your daily routine can help alleviate symptoms and improve mobility. By including gentle exercises, practicing good habits, and seeking appropriate medical care when needed, individuals with frozen shoulders can improve mobility, reduce pain, and regain function in their shoulders.
However one should Remember to start slowly and gradually increase the intensity of exercises as tolerated. If symptoms persist or worsen, one should consult a physiotherapist for further evaluation and treatment options. With patience and consistent effort, relief from frozen shoulder is attainable.
Click here to book an appointment with a physiotherapist at one of our eight locations.
- Physiotherapy Etobicoke – Triangle Physiotherapy Etobicoke
- Oakville Physiotherapy Clinic – Triangle Physiotherapy Oakville
- Physiotherapy North York – Triangle Physiotherapy North York
- Mississauga Physiotherapy Clinics – Triangle Physiotherapy Mississauga
- Downtown Physiotherapy Clinics – Triangle Physiotherapy King West
- Uptown Physiotherapy Clinics – Triangle Physiotherapy Lawrence Park
- Physiotherapy Clinic Downtown Toronto – Triangle Physiotherapy Queens Quay
- Physiotherapy Clinics Mississauga – Triangle Physiotherapy Erin Mills
Managing frozen shoulder can be more effective with the right exercises and expert guidance. If you’re seeking support, consider physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, or Liberty Village. Experienced physiotherapists in these locations can provide tailored exercise plans and treatments to help you regain mobility and reduce pain.
Vertigo is a common vestibular disorder characterized by a sensation of spinning or dizziness, often accompanied by nausea, sweating, and balance problems. It can significantly impact daily life and lead to falls and injuries if not properly managed. While vertigo can have various underlying causes, including inner ear issues, vestibular migraines, and neurological conditions, physiotherapy can play a crucial role in managing symptoms and improving balance. In this article, we’ll explore some effective physiotherapy tips for individuals dealing with vertigo and how these exercises can help them regain their balance and quality of life.
Understanding Vertigo
Vertigo is a symptom rather than a condition itself and is often caused by disturbances in the inner ear or the vestibular system, which controls balance and spatial orientation. Common causes of vertigo include benign paroxysmal positional vertigo (BPPV), vestibular neuritis, Meniere’s disease, and vestibular migraines. Symptoms of vertigo can vary in severity and duration, ranging from mild, intermittent episodes to constant and debilitating dizziness. Vertigo signs such as dizziness, nausea, and imbalance can significantly affect daily activities and quality of life.
Physiotherapy for Vertigo
Physiotherapy for vertigo, known as Vestibular Rehabilitation Therapy (VRT), focuses on exercises and techniques to improve balance, reduce dizziness, and enhance vestibular function.
Vestibular Rehabilitation Therapy (VRT)
VRT is a specialized form of physiotherapy designed to improve balance and reduce vertigo symptoms through targeted exercises and maneuvers.
These exercises aim to promote adaptation and compensation within the vestibular system, helping the brain adjust to changes in balance and spatial orientation.
Common VRT exercises include gaze stabilization exercises, balance training, habituation exercises, and sensory integration techniques.
VRT is tailored to each individual’s specific needs and may include the following components:

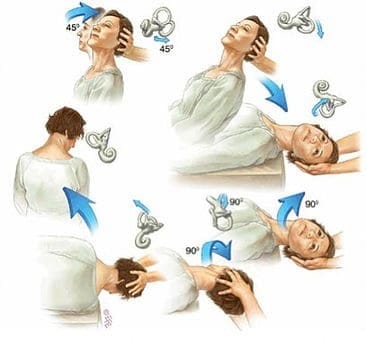
Canalith Repositioning Maneuvers (CRM)
Canalith repositioning maneuvers, such as the Epley maneuver for BPPV, are effective in treating certain types of vertigo caused by displaced calcium crystals in the inner ear.
A trained and qualified physiotherapist can perform these maneuvers to help reposition the crystals and alleviate symptoms of dizziness and spinning.
Gaze Stabilization Exercises
Gaze stabilization exercises aim to improve visual focus and stability during head movements, which can help reduce dizziness and improve balance.
Examples of gaze stabilization exercises include tracking moving objects with the eyes or performing head movements while maintaining focus on a stationary target.
Balance Training
Balance training exercises help improve stability and reduce the risk of falls in individuals with vertigo.
These physiotherapy exercises for vertigo focus on improving proprioception, coordination, and postural control through activities such as standing on one leg, walking in tandem, and using balance boards or stability balls.
A physiotherapist can provide personalized balance training exercises tailored to the individual’s specific needs and level of impairment.
Vestibular Habituation Exercises
Habituation exercises involve gradually exposing individuals to movements or stimuli that provoke vertigo symptoms in a controlled manner.
Over time, repeated exposure helps desensitize the vestibular system and reduce the intensity and frequency of vertigo episodes.
Examples of habituation exercises include head movements, visual tracking exercises, and simulated motion activities.
Lifestyle Modifications
In addition to physiotherapy interventions, certain lifestyle modifications can help manage vertigo symptoms and improve overall quality of life. These may include avoiding triggers such as sudden head movements or excessive visual stimuli, practicing stress management techniques, staying hydrated, and maintaining a healthy diet and sleep routine.
Physical therapy, specifically vestibular rehabilitation therapy, offers valuable tools and techniques for individuals struggling with vertigo. By addressing underlying vestibular dysfunction and improving balance and stability, physical therapists empower individuals to regain their independence and confidence in daily activities. If you’re experiencing vertigo symptoms, consider consulting with a physical therapist at Physiotherapy Oakville trained in vestibular rehabilitation to develop a personalized treatment plan tailored to your needs. With the right guidance and support, relief from vertigo is within reach, allowing you to find your balance and reclaim your life.
Click here to book an appointment with a physiotherapist at one of our eight locations
- Physiotherapy Etobicoke – Triangle Physiotherapy Etobicoke
- Oakville Physiotherapy Clinic – Triangle Physiotherapy Oakville
- Physiotherapy North York – Triangle Physiotherapy North York
- Mississauga Physiotherapy Clinics – Triangle Physiotherapy Mississauga
- Downtown Physiotherapy Clinics – Triangle Physiotherapy King West
- Uptown Physiotherapy Clinics – Triangle Physiotherapy Lawrence Park
- Physiotherapy Clinic Downtown Toronto – Triangle Physiotherapy Queens Quay
- Physiotherapy Clinics Mississauga – Triangle Physiotherapy Erin Mills
Physiotherapy can be highly effective in managing vertigo and improving balance. If you’re looking for physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, or Liberty Village, there are experienced physiotherapists available to help you regain stability and enhance your quality of life.
Recovering from post-cycling tiredness is essential to optimize your performance and prevent injuries. There are some exercises and stretches to help you rejuvenate and relieve tired muscles after cycling. Before we talk about these exercises in detail let us discuss what is post cycling tiredness.
What is post cycling tiredness
Post-cycling tiredness, also known as post-ride fatigue or post-exercise fatigue, refers to the feeling of tiredness, lethargy, and muscle soreness that cyclists may experience after completing a cycling workout or ride. It is a common phenomenon that occurs as a result of the physical and physiological demands placed on the body during cycling exercise.
Several factors contribute to post-cycling tiredness:
- Muscle Fatigue: Cycling engages multiple muscle groups, including the quadriceps, hamstrings, calves, glutes, and core muscles. The repetitive pedalling motion and varying terrain can lead to muscle fatigue and soreness, especially during longer or more intense rides.
- Depletion of Energy Stores: Cycling is an endurance activity that requires sustained energy expenditure. As cyclists pedal, they utilize glycogen stores in the muscles and liver for fuel. After a ride, glycogen stores may become depleted, leading to feelings of fatigue and exhaustion.
- Fluid and Electrolyte Loss: Sweating is a natural response to exercise, and cyclists can lose significant amounts of fluid and electrolytes during rides, particularly in hot or humid conditions. Dehydration and electrolyte imbalances can contribute to feelings of fatigue and weakness post-ride.
- Muscle Damage and Inflammation: Cycling, especially over challenging terrain or at high intensities, can cause micro-tears in muscle fibres and induce inflammation in the muscles. This process, known as muscle damage, is a natural part of the muscle repair and adaptation process but can also contribute to feelings of soreness and exhaustion.
- Central Nervous System Fatigue: Prolonged or intense cycling efforts can also lead to fatigue at the central nervous system level. The brain and central nervous system play a crucial role in regulating muscle contractions, coordination, and mental focus during exercise. Fatigue at the central nervous system level can manifest as mental fatigue, decreased motivation, and impaired coordination post-ride.
Overall, post-cycling tiredness is a normal physiological response to the demands of cycling exercise. While it can be uncomfortable, it is typically temporary and can be managed with adequate rest, hydration, nutrition, and recovery strategies. Proper post-ride recovery practices and exercises including stretching, foam rolling, hydration, nutrition, and rest, can help cyclists minimize post-cycling tiredness and optimize their recovery for future rides.
Exercises and stretches to help you relieve tired muscles after cycling
Foam Rolling:
- Use a foam roller to massage tight muscles and release tension accumulated during cycling. Focus on areas such as the quadriceps, hamstrings, calves, and glutes.Roll slowly over each muscle group, pausing on any tender spots or trigger points to apply gentle pressure and encourage relaxation.
Static Stretches:
- Perform static stretches to improve flexibility and relieve muscle tightness. Hold each stretch for 20-30 seconds and repeat 2-3 times on each side.
Quadriceps Stretch:
- Stand tall and bring one heel towards your glutes, grabbing the ankle with your hand and gently pulling it towards your buttocks.
Hamstring Stretch:
- Sit on the floor with one leg extended and the other bent. Lean forward from the hips, reaching towards your toes while keeping your back straight.
Calf Stretch:
- Stand facing a wall with one foot forward and the other foot back. Lean forward, keeping the back heel on the ground, until you feel a stretch in the calf of the back leg.
Hip Flexor Stretch:
- Kneel on one knee with the other foot forward, and gently push your hips forward until you feel a stretch in the front of the hip.
Leg Elevation:
- Lie on your back with your legs extended against a wall or elevated surface. Relax your muscles and allow gravity to assist in draining fluid build-up from your legs, reducing swelling and fatigue. Elevating your legs helps improve circulation and promotes faster recovery by reducing muscle soreness and fatigue.
Low-Intensity Cardio:
- Engage in low-intensity cardiovascular activities such as walking, swimming, or gentle cycling to promote blood flow and flush out metabolic waste products from your muscles.
- Keep the intensity low to allow your body to recover without adding additional stress to fatigued muscles.
Deep Breathing and Relaxation:
- Practice deep breathing exercises and relaxation techniques to promote mental and physical relaxation. Find a quiet space, close your eyes, and focus on slow, deep breaths to reduce stress and tension in your body.
- Incorporate mindfulness or meditation practices to help calm your mind and promote overall relaxation and well-being.
Hydration and Nutrition:
- Drink plenty of water to stay hydrated and replenish fluids lost during exercise. Consume a balanced meal or snack containing carbohydrates and protein to refuel your muscles and support recovery.
Foods rich in antioxidants, such as fruits, vegetables, and nuts, can help reduce inflammation and promote recovery from exercise-induced oxidative stress.
Incorporate these exercises and recovery strategies into your post-cycling routine to help alleviate tiredness, promote muscle recovery, and restore your body’s balance and energy levels. Consider integrating Physiotherapy in Oakville as part of your recovery plan to further enhance these benefits. Listen to your body, and adjust the intensity and duration of your recovery activities based on your individual needs and preferences. Happy Cycling!
Frequently Asked Questions
- What is post-cycling tiredness?
- Post-cycling tiredness refers to the fatigue, lethargy, and muscle soreness experienced after a cycling workout, resulting from the physical and physiological demands of cycling.
- What causes post-cycling tiredness?
- Factors include muscle fatigue, depletion of energy stores, fluid and electrolyte loss, muscle damage and inflammation, and central nervous system fatigue.
- Why is foam rolling recommended after cycling?
- Foam rolling helps massage tight muscles, release tension, and improve recovery by focusing on areas like the quadriceps, hamstrings, calves, and glutes.
- How do static stretches aid in recovery?
- Static stretches improve flexibility, relieve muscle tightness, and should be held for 20-30 seconds to effectively stretch the muscle.
- What’s the proper way to perform a quadriceps stretch?
- Stand tall, bring one heel towards your glutes, grab the ankle, and gently pull it towards your buttocks.
- How does a hamstring stretch work?
- Sit with one leg extended, the other bent, and lean forward from the hips towards your toes, keeping your back straight.
- What is the benefit of calf stretches?
- Calf stretches improve flexibility in the calf muscles, essential for cyclists to relieve tightness and promote recovery.
- Why is hip flexor stretching important?
- Hip flexor stretches help alleviate tightness in the front of the hip, common in cyclists due to the cycling posture.
- How does leg elevation help in post-cycling recovery?
- Elevating legs aids in draining fluid buildup, reduces swelling and fatigue, and improves circulation for faster recovery.
- What role does hydration and nutrition play in recovery?
- Staying hydrated and consuming a balanced meal or snack post-ride replenishes fluids, refuels muscles, and supports overall recovery.
Recovering from cycling fatigue can be enhanced with the right post-cycling exercises and guidance. For personalized support, consider physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, or Liberty Village. Expert physiotherapists in these locations can provide tailored recovery plans to help you stay active and reduce tiredness effectively.
Introduction
Physiotherapy stands as a cornerstone in the realm of healthcare, offering a holistic approach to the maintenance, rehabilitation, and enhancement of physical function. In Oakville, a city renowned for its commitment to health and wellness, physiotherapy emerges as a pivotal service for residents aiming to revitalize their health. This article delves into the profound benefits of physiotherapy in Oakville, highlighting its significance in fostering a community of well-being and vitality.
Understanding Physiotherapy
Physiotherapy, a science-driven profession, employs a variety of techniques and modalities to restore, maintain, and maximize physical strength, function, motion, and overall well-being. The historical roots of physiotherapy trace back centuries, evolving significantly to the comprehensive practice we recognize today.
The Science Behind Physiotherapy
The effectiveness of physiotherapy lies in its evidence-based approach, utilizing an understanding of anatomy, physiology, and the principles of biomechanics. It plays a crucial role in pain management, employing techniques like manual therapy, exercise, and electrotherapy to alleviate discomfort and enhance function.
Benefits of Physiotherapy
The advantages of physiotherapy extend beyond mere injury recovery. It is instrumental in enhancing mobility, managing chronic conditions, improving posture, and even preventing future physical issues. For athletes, physiotherapy is a staple in both recovery and performance enhancement.
Physiotherapy in Oakville: A Closer Look
Oakville’s physiotherapy landscape is distinguished by its quality of care and patient-centric approach. The city is home to leading clinics and therapists dedicated to providing tailored treatments that address individual health goals and concerns.
Specialized Physiotherapy Services in Oakville
Recognizing the diverse needs of its community, Oakville offers specialized physiotherapy services catering to various demographics, including children, the elderly, athletes, and individuals with neurological conditions, ensuring comprehensive care for all.
Integrating Physiotherapy into Your Wellness Routine
Physiotherapy should not be viewed as a last resort for injury or illness but as a proactive measure in maintaining optimal health. Understanding when and how to incorporate physiotherapy into your life can significantly enhance your overall wellness.
Choosing the Right Physiotherapist
The key to a successful physiotherapy experience lies in selecting the right practitioner. Factors such as qualifications, specialization, and a patient-centered approach are critical in choosing a therapist that aligns with your health objectives.
Insurance and Physiotherapy in Oakville
Navigating the intricacies of insurance coverage for Physiotherapy Oakville residents. Understanding your policy and out-of-pocket expenses can ensure that you make the most of your benefits while seeking treatment.
The Future of Physiotherapy in Oakville
The field of physiotherapy is constantly evolving, with ongoing research and technological advancements shaping its future. Oakville’s commitment to healthcare innovation positions it as a leader in the advancement of physiotherapy practices.
Conclusion
Physiotherapy offers a pathway to enhanced health and wellness, playing a vital role in the lives of Oakville residents. By embracing its benefits and integrating it into our health routines, we can all contribute to a healthier, more vibrant community.
FAQ
How often should I attend physiotherapy sessions?
Frequency depends on your condition and goals. Your therapist will recommend a schedule tailored to your needs.
Can physiotherapy completely cure chronic conditions?
While not all chronic conditions can be cured, physiotherapy can significantly alleviate symptoms and improve quality of life.
What should I wear to my physiotherapy appointments?
Opt for comfortable, loose-fitting clothing that allows easy access to the area being treated and facilitates movement.
How long does it take to see results from physiotherapy?
Results vary depending on the individual and their condition. Some may notice improvements within a few sessions, while others may take longer.
Can children and elderly benefit from physiotherapy?
Absolutely. Physiotherapy offers benefits across all age groups, with specialized programs catering to the unique needs of children and the elderly.
Is physiotherapy only for injury recovery?
No, physiotherapy is also valuable for preventive care, managing chronic conditions, and enhancing overall physical well-being.
What are the risks of not seeking physiotherapy after an injury?
Foregoing physiotherapy can lead to prolonged recovery, decreased functionality, and an increased risk of re-injury.
By embracing the comprehensive benefits of physiotherapy, particularly in a community-focused city like Oakville, we can all take proactive steps towards maintaining and enhancing our health and well-being.
“Revitalizing your health with physiotherapy can lead to numerous benefits, from pain relief to improved mobility. Triangle Physiotherapy provides expert care across the GTA, including Physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, and Liberty Village. Our dedicated team is here to help you achieve your health and wellness goals through personalized physiotherapy treatments.”
Physiotherapy is a vital part of healthcare that focuses on physical rehabilitation, injury prevention, and the health and wellness of patients. Whether you’re dealing with a chronic condition, recovering from surgery, or looking to improve your physical performance, physiotherapy can offer significant benefits. Here are ten compelling reasons to consider joining Physiotherapy Oakville and experiencing these benefits firsthand.
1. Relief from Chronic Pain
Chronic pain, which can arise from various conditions such as arthritis or repetitive strain injuries, can be debilitating. Physiotherapists use a combination of treatments, including exercise, manual therapy, and education about pain management strategies to help alleviate this pain and improve your daily function.
2. Recovery After Surgery
Post-operative care is crucial for a successful recovery, especially after orthopedic surgeries like knee or hip replacements. Physiotherapists design customized rehabilitation programs to help you regain strength, mobility, and function, facilitating a quicker and more effective recovery.
3. Injury Rehabilitation
Physiotherapy is essential for the rehabilitation of injuries, whether they’re sports-related, accidental, or due to everyday activities. Through targeted exercises and therapies, physiotherapists help heal injured tissues, restore function, and prevent further injuries.
4. Support for Aging Adults
Aging can bring about various physical challenges, including joint wear and tear, reduced balance, and decreased strength. Physiotherapy offers strategies and treatments to help older adults maintain their independence, reduce pain, and manage age-related conditions.
5. Treatment for Neurological Disorders
For individuals affected by neurological conditions such as stroke, multiple sclerosis, or Parkinson’s disease, physiotherapy can play a significant role in rehabilitation. It aims to enhance function, improve mobility, and increase independence through personalized therapeutic exercises and techniques.
6. Balance Improvement and Fall Prevention
Balance issues can significantly increase the risk of falls, particularly in older adults. Physiotherapists utilize specific exercises to challenge and improve balance, enhancing stability and reducing the likelihood of falls.
7. Enhancement of Athletic Performance
Athletes at all levels can benefit from physiotherapy, not just for injury treatment but also for performance enhancement. Physiotherapists provide guidance on optimizing strength, flexibility, and technique to improve athletic performance and reduce the risk of sports injuries.
8. Pediatric Care
Children with developmental disorders, congenital conditions, or injuries can achieve better mobility and function through pediatric physiotherapy. Tailored to each child’s needs, this therapy focuses on enhancing movement patterns and addressing developmental challenges.
9. Management of Women’s Health Issues
Physiotherapy addresses specific women’s health concerns, including postnatal recovery, pelvic floor dysfunction, and lymphedema following breast cancer surgery. Specialized physiotherapists offer treatments and exercises to manage these conditions effectively.
10. Assistance with Respiratory Conditions
Physiotherapy also plays a role in managing respiratory conditions like asthma and chronic obstructive pulmonary disease (COPD). Through breathing exercises and techniques to clear mucus from the lungs, physiotherapy can help improve breathing and overall lung function.
Seeking the expertise of a physiotherapist can lead to significant improvements in your health and well-being. Whether you’re dealing with a specific medical condition, recovering from an injury, or simply looking to improve your physical capabilities, physiotherapy offers a wide range of benefits tailored to meet your individual needs.
Frequently Asked Questions
1. What conditions can physiotherapy treat?
Physiotherapy can treat a wide range of conditions including, but not limited to, chronic pain, sports injuries, post-surgical rehabilitation, neurological disorders (like stroke or Parkinson’s disease), respiratory conditions, pediatric conditions, women’s health issues, and age-related mobility problems.
2. Do I need a referral to see a physiotherapist?
In many places, you can see a physiotherapist without a referral (direct access). However, some insurance plans or healthcare systems may require a referral from a doctor for the services to be covered. It’s best to check with your insurance provider or local healthcare regulations.
3. What should I expect during my first physiotherapy appointment?
During your first visit, the physiotherapist will conduct a comprehensive assessment, which includes discussing your medical history, the symptoms you are experiencing, and your treatment goals. They may also perform a physical examination to evaluate your condition further. Based on this assessment, they will develop a personalized treatment plan.
4. How long does a physiotherapy session last?
The duration of a physiotherapy session can vary but typically lasts between 30 to 60 minutes. The length of your session may depend on your specific condition, the treatments involved, and the policies of the physiotherapy clinic.
5. Will physiotherapy treatments hurt?
While physiotherapy aims to relieve pain and improve your condition, some treatments or exercises might cause discomfort, especially when recovering from an injury or surgery. Your physiotherapist will work with you to ensure treatments are manageable and will adjust your therapy plan as needed to keep discomfort to a minimum.
“Consulting a physiotherapist can significantly enhance your well-being, addressing a wide range of health concerns. Triangle Physiotherapy offers expert care across the GTA, including Physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, and Liberty Village. Our experienced team is dedicated to helping you achieve your health goals through personalized physiotherapy treatments.”
Introduction:
In the dynamic realm of healthcare, the significance of proper equipment cannot be overstated. Among the essential fixtures, therapy tables play a pivotal role in ensuring both patient comfort and effective treatment. In this comprehensive guide, we delve into the various types of therapy tables, the art of choosing the right one, and the manifold benefits they offer to healthcare professionals and patients alike.
Types of Types of Therapy Tables
There are many types of Therapy Tables some of which are In following:
- Massage Tables:
- Designed for massage therapy sessions.
- Typically padded for comfort.
- Adjustable height to accommodate different therapists and client preferences.
- Physical Therapy Tables:
- Specifically designed for physical therapy exercises and treatments.
- May include features like adjustable sections, traction, or tilting capabilities.
- Chiropractic Tables:
- Tailored for chiropractic adjustments and treatments.
- Often have adjustable sections and features to support spinal manipulations.
- Examination Tables:
- Used in medical settings for general examinations and evaluations.
- Usually have a flat, cushioned surface with adjustable height.
- Rehabilitation Tables:
- Designed for rehabilitation exercises and activities.
- Often equipped with features like straps, supports, and adjustable sections.
- Occupational Therapy Tables:
- Geared towards occupational therapy interventions.
- May have adjustable height and features to support various activities.
- Tilt Tables:
- Used for tilt table testing or therapy.
- Can be tilted to different angles to assist with specific therapeutic goals.
- Exam Table:
- Versatile Design: Exam tables serve as essential fixtures in medical examination rooms, offering a flexible solution for a range of examinations.
- Comfortable and Adjustable: Designed to provide a comfortable and adjustable surface, these tables support routine check-ups, consultations, and minor medical procedures for patients.
- Mat Tables:
- Low tables are designed for therapies conducted on mats.
- Suitable for activities where clients need to be closer to the ground.
- Gynecologist Table:
- Gynecologist tables designed for women’s health exams with adjustable features and specialized stirrups.
- Ensures optimal positioning, promoting comfort and accessibility for healthcare practitioners during gynecological exams.
Choosing the Right Therapy Table
Selecting the appropriate therapy table is a nuanced process that involves considering various factors. Healthcare providers must assess the specific needs of their practice and patient population. Factors to consider include:
- Functionality: Ensuring the table serves the intended purpose efficiently.
- Adjustability: Opting for tables with customizable features for diverse patient requirements.
- Durability: Investing in tables constructed with high-quality materials for long-lasting use.
- Hygiene and Maintenance: Choosing tables that facilitate easy cleaning and maintenance for infection control.
Benefits of Therapy Tables
- Enhanced Patient Comfort: Therapy tables are designed with patient comfort in mind, featuring padded surfaces and ergonomic designs that alleviate discomfort and anxiety during medical examinations or treatments.
- Facilitated Medical Procedures: Whether it’s a routine check-up or a specialized medical procedure, therapy tables provide a stable and adjustable platform, optimizing the ease with which healthcare professionals can perform their tasks.
- Improved Accessibility: Specialized tables, such as gynecologist tables, enhance accessibility for both patients and healthcare practitioners, ensuring examinations are conducted with precision and care.
- Efficient Patient Transport: Gurney beds streamline the process of patient transport within healthcare facilities, promoting efficiency and reducing the risk of injurie
- gynecologist table
- s for both patients and healthcare staff.
Conclusion
In conclusion, therapy tables are indispensable assets in the healthcare landscape. From gurney beds facilitating seamless patient transport to exam tables providing versatile examination solutions, and gynecologist tables catering to the unique needs of women’s health, the right therapy table can significantly impact the quality of patient care. By carefully considering the specific requirements of their practice, healthcare providers can choose tables that not only meet their needs but also contribute to an environment of enhanced patient well-being and comfort. As the healthcare industry continues to evolve, the role of therapy tables in delivering optimal care remains steadfast.
Golfer’s elbow and Tennis Elbow are both tendonitis. The difference is Golfer’s elbow occurs on the inner side of the elbow while Tennis Elbow occurs on the outer side of the elbow. Tennis elbow, also known as lateral epicondylitis is the inflammation of the tendon that connects the forearm muscles to a bony prominence on the outside of the elbow known as the lateral epicondyle. Golfer’s elbow, on the other hand, is known as medial epicondylitis because the inflammation is on the tendons which are attached to the medial epicondyle.
How Is Tennis Elbow Diagnosed?
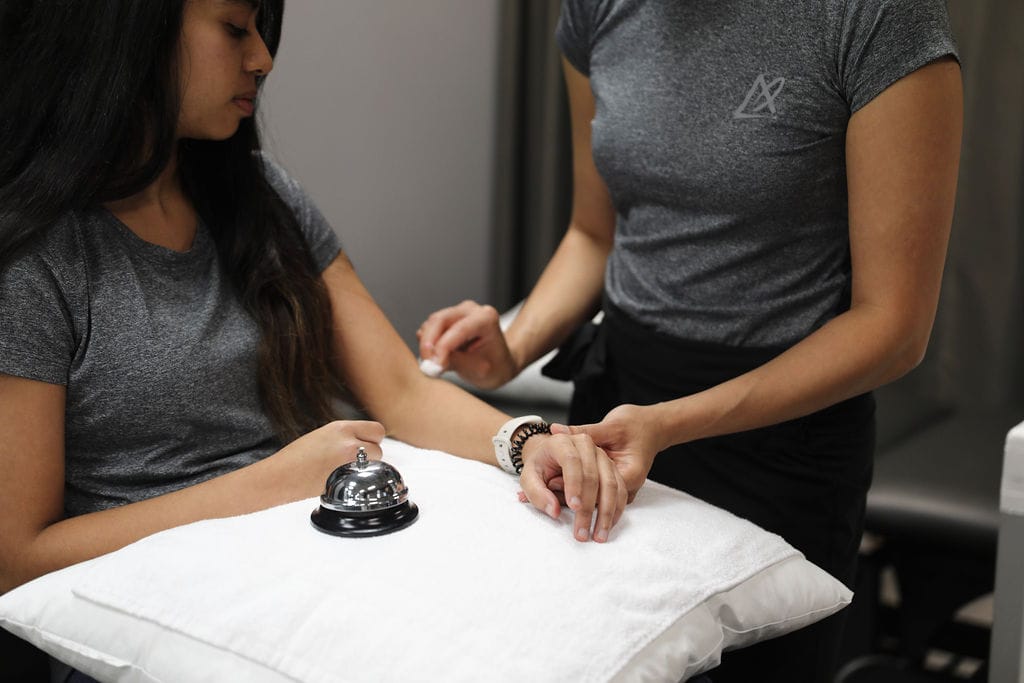
Your physiotherapist will evaluate tennis elbow by reviewing your medical history, performing and reviewing your medical history. A doctor may recommend a X-ray, EMG or MRI to assess the severity of the condition.
A physiotherapist can also conduct a detailed assessment of your elbow and the surrounding structures in order to create a personalized treatment plan for you. Special tests such as Cozen’s and Mills Test can also be used to diagnose Tennis elbow.
What are the complications of a Tennis Elbow?
Complications of Tennis elbow or lateral epicondylitis may include tendon rupture, recurrence of the injury, chronic pain, nerve entrapment in the forearm, and failure to improve despite both nonsurgical and no surgical treatment.
Cause of Tennis Elbow and Treatment
What causes a Tennis elbow and who might get a Tennis Elbow?
Some causes of Tennis elbow are:
- weak wrist muscles,
- use of tennis racquets that are too short,
- weakened muscles of the shoulder and wrist,
- repetitive hand motions,
- poor tennis technique,
- frequent use of hand tools,
- lifting heavy objects, and
- excessive gripping activities.
Despite the name, Tennis elbow is not only for tennis players although they tend to often develop tennis elbow because of the repetitive muscle use and gripping activities the sport entails. People whose professions involve repetitive use of the wrist and forearm are more likely to develop lateral epicondylitis.
Some professions, such as painters, dentists, plumbers, carpenters, musicians, and cooks, may develop Tennis elbow which can also be caused by the repetitive use of a keyboard and mouse.
What Is The Best Treatment For Tennis Elbows?
The majority of tennis elbow cases can be successfully treated without surgical intervention. How a tennis elbow is treated may vary depending on which medical professional you choose to see.
Research has shown that physiotherapy is the most effective treatment of the Tennis elbow.
Tennis Elbow Physiotherapy Treatment
- Therapeutic Ultrasound
- Acupuncture
- Tennis elbow treatment exercises
- Deep tissue massage
- Shockwave therapy
- Taping or brace
- TENS
- Modified activities
- Hot and cold packs
How does massage help heal Tennis elbow?
Tennis Elbow Massage Treatment helps improve circulation, stimulate collagen production, and increases mobility in the affected area.
What Can I Do To Prevent Tennis Elbow?
There are many ways to prevent Tennis elbow such as:
- Stretching regularly.
- Strengthening of the forearm muscles.
- Modifying activities that contribute to pain.
- Warming up before playing tennis and other sports and ensuring the stability of the wrist.
What are some Tennis elbow exercises which can be done at home to help prevent recurrence?
Specific Tennis elbow exercises to strengthen as well as stretch the muscles that are attached to the injured tendon will certainly help speed up healing which then increases its resistance to repetitive stress… Some of these Tennis elbow treatment exercises are Stress ball squeeze, finger stretch, wrist extension, flexion stretch, forearm extension, flexion, supination, and pronation strengthening exercises.
Are there any natural Tennis elbow treatments I can do at home while I wait to see a physiotherapist?
Resting and avoiding activities that aggravate your pain can be beneficial. You may also try to apply an ice pack for 15 mins three times a day.
What is the best treatment for chronic Tennis elbow?
The most effective treatment for chronic tennis elbow has always been physiotherapy and exercise. If physiotherapy does not fully heal it, however, steroid injections, braces, and surgery may also help.
Our physiotherapists in Toronto, Midtown Toronto, Mississauga, North York and Oakville can help you with tennis elbow. Book your appointment here.
“Effectively treating tennis elbow and golfer’s elbow requires specialized physiotherapy care. Triangle Physiotherapy offers expert services across the GTA, including Physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, and Liberty Village. Our experienced physiotherapists can help you recover from elbow pain and regain strength with personalized treatment plans.”
Things you need to know about active release technique (ART)
What is Active Release Therapy and how does ART help?
Active Release Techniques (ART) is a patented soft tissue technique that treats problems with muscles, tendons, fascia, ligaments, and nerves by using isolated pressure and movements on soft tissues to release adhesions. It is very effective in improving pain and increasing blood flow and healing soft tissues.
How does the active release technique work?
During an ART session, the therapists identify, isolate and target the affected areas by using their hands to locate an area with adhesion. They then apply traction to that specific area while the patient moves their body, in order to pull the muscle underneath. This technique helps break up the scar tissue which helps the area restore proper blood flow.
Active Release Therapy works by breaking up adhesions, which are a microscopic form of scar tissue. This can cause pain, weakness, reduced flexibility, and nerve damage.
What are the benefits of ART?
The active release technique is very beneficial for neck, lower back, shoulder, and knee pain.
List Of Benefits Of Art (Active Release Technique):
- Improve flexibility
- Reduces Pain
- Promotes faster recovery
- Enhances athletic performance
- Improves circulation
What injuries can you treat with Active Release Technique?
- Sciatica
- Ankle sprains
- Iliotibial Band Syndrome
- Hamstring strain
- Carpal Tunnel Syndrome
- Cubital Tunnel Syndrome
- TMJ Disorders
- Plantar fasciitis
- Neck and Low back pain
- Nerve Entrapment
- Radial Tunnel Syndrome.
- Repetitive strain injuries
- Shoulder impingement
- Medial and Lateral Epicondylitis
How Does ART Help?
The active Release Technique helps restore the function of soft tissue which helps prevent injuries and promotes faster recovery. Active Release Therapy helps break up adhesions which then aid in restoring normal tissue motion and function.
How effective is ART and Does the Active Release Technique Really Work?
Numerous studies show that ART is a highly effective soft tissue treatment. In fact, it has been extremely popular with athletes, especially in North America helps them train better and be injury free.
How Long Does Active Release Technique Take To Work?
The time it takes for Art to work varies depending on how long the individual has had the injury and other factors. Our chiropractor will create a treatment plan for you based on the assessment findings.
How To Do Active Release Technique
During Active Release Therapy (ART), a muscle is shortened and the therapist applies tension to the muscle while the patient moves the area to actively lengthen the muscle. This may cause some pain but this is normal because this technique works by increasing the nervous system’s tolerance to the stretch to a tight muscle.
Is Active Release Technique Covered By Insurance?
Active release therapy at our clinics is done by our registered chiropractors so it will cover your sessions if your insurance plan covers chiropractic care.
History of Active Release Technique
ART has been developed, refined, and patented by P. Michael Leahy, DC, CCSP. He developed this technique because he noticed that his patient’s symptoms seemed to be related to the changes in the soft tissue which he could palpate. This technique method focuses on relieving tension in the tissue caused by repetitive movement.
This technique revolves completely around the patient’s symptoms and aims to treat soft tissue mobility issues with tendons, ligaments, muscles, nerves, and fascia.
Dr. Leahy consistently helped heal 90% of his patients’ issues. In 1985, he first documented his work under the title of Myofascial Release, but later on, he patented it under the name Active Release Techniques. He is now teaching healthcare providers all over the world to use ART.
How Much Does Active Release Technique Cost?
ART is done by our chiropractors. The fees for chiropractic services are:
Initial session which is an hour long and includes assessment and assessment for $125.
A 30 minute follow up treatment session is for $95.
How Art Is Different Considered To Many Other Soft Tissue Techniques?
The main difference between Active Release Therapy and any other soft tissue techniques is that ART incorporates active movement into treatment. While the therapist presses on the affected area, the patient actively moves the affected structure.
Active Release Technique Vs Myofascial Release
- Is Active Release Technique the same As Myofascial Release?
Active Release Therapy is an advanced form of Myofascial release and its main goal is to break up adhesions which helps with the reduction of pain and increases the range of motion. It also helps reduce inflammation by improving circulation.
The main goal of Myofascial Release Therapy is to loosen the fascia and release restrictions to restore the range of motion and decrease pain.
In Myofascial Release Therapy, the therapist applies gentle but firm pressure to areas known as trigger point areas to release the tension.
Book your appointment for an ART session here.