In today’s digital age, it’s hard to avoid spending long hours staring at screens, whether it’s for work, social media, or entertainment. Unfortunately, this extended screen time can often lead to neck pain, commonly known as “tech neck” or “text neck”. Tech neck refers to the discomfort or pain caused by poor posture when using digital devices, such as smartphones, tablets, and computers. The good news is that with a few simple physiotherapy tips, you can reduce the risk of developing tech neck and promote better posture.
The physiotherapists at Triangle Physiotherapy can help you with the neck pain that is associated with extended use of digital devices.
What Causes Neck Pain from Digital Devices?
The main culprit behind neck pain associated with digital devices is poor posture. When we use our devices, we often find ourselves slouching or looking down for extended periods, which places unnecessary strain on the neck muscles and spine. Over time, this repetitive motion can lead to muscle tension, discomfort, and even long-term damage.
Several factors contribute to this issue, including:
- Forward head posture: When you lean your head forward to look at your device, the muscles in the neck and upper back work harder to hold your head in position, leading to strain.
- Slouching: Sitting or standing with a rounded back and shoulders can cause the neck to overcompensate, increasing pressure on the muscles and joints.
- Screen height and distance: If your screen is too low or too far from your eyes, it forces you to look down or strain your neck to see clearly.
Common Symptoms of Tech Neck from Screen Use
Neck pain related to digital devices can present itself in various ways, including:
- Stiffness and soreness: You may notice tightness in your neck, shoulders, or upper back after using your devices for extended periods.
- Headaches: Tension in the neck muscles can trigger headaches, particularly around the base of the skull.
- Pain with movement: You might feel discomfort or limited mobility when trying to turn your head or tilt your neck.
- Numbness or tingling: In some cases, pressure on the nerves in the neck can cause sensations of numbness or tingling in the arms or hands.
How to Prevent Neck Pain from Digital Devices
The good news is that neck pain from digital devices can be prevented with some mindful changes to your posture and daily habits. Here are a few physiotherapy tips to help you avoid tech neck:
- Maintain Proper Posture: Always aim to keep your head aligned with your spine. Your ears should be over your shoulders, and your shoulders should be back, not hunched forward. Keep your screen at eye level to avoid tilting your head downward.
- Take Regular Breaks: Avoid sitting in the same position for too long. Follow the 20-20-20 rule: every 20 minutes, take a 20-second break and look at something 20 feet away to give your eyes and neck a break.
- Use Ergonomic Setups: Set up your workstation so that your screen is at eye level, and your chair provides proper lumbar support. If you’re using a phone or tablet, consider holding it at eye level or using a stand to prevent looking down.
- Stretch and Strengthen: Incorporate neck and shoulder stretches into your daily routine to relieve tension and promote flexibility. Strengthening exercises for the upper back can also improve posture and support the neck muscles.
- Adjust Screen Time: Reducing the amount of time spent on screens can help lower your risk of neck pain. If you’re working long hours on a computer, try to schedule breaks to move and stretch regularly.
- Stay Hydrated: Dehydration can make muscles more prone to stiffness. Drinking plenty of water can help keep your muscles healthy and prevent tightness.
Treatment for Neck Pain from Digital Devices
If you’re already experiencing neck pain, there are several treatment options available to help alleviate discomfort:
- Physiotherapy: A physiotherapist can assess your posture, identify any muscle imbalances, and recommend specific exercises to strengthen and stretch the muscles that support your neck.
- Massage Therapy: A massage therapist can help release tightness in the neck and upper back muscles, providing relief from tension.
- Hot or Cold Therapy: Applying a warm compress or ice pack to the neck can help reduce inflammation and ease muscle stiffness.
Preventing Text Neck Long-Term
To prevent recurring neck pain, it’s essential to incorporate good posture habits into your daily routine and practice regular stretches and strengthening exercises. Additionally:
- Avoid prolonged screen use: Try to limit the amount of time you spend hunched over devices, especially for tasks that require sustained focus.
- Optimize your workspace: Ensure your desk, chair, and screen setup are ergonomically sound to support good posture.
- Move frequently: Avoid sitting for extended periods without changing positions or stretching.
Neck pain from digital devices is a growing concern, but with the right prevention strategies, it’s entirely possible to avoid or minimize discomfort. By being mindful of your posture, taking regular breaks, and incorporating stretches and strengthening exercises into your routine, you can protect your neck and enjoy your screen time without the pain. If you’re already experiencing neck pain, consider consulting with a physiotherapist to develop a treatment plan that will get you back to feeling your best.
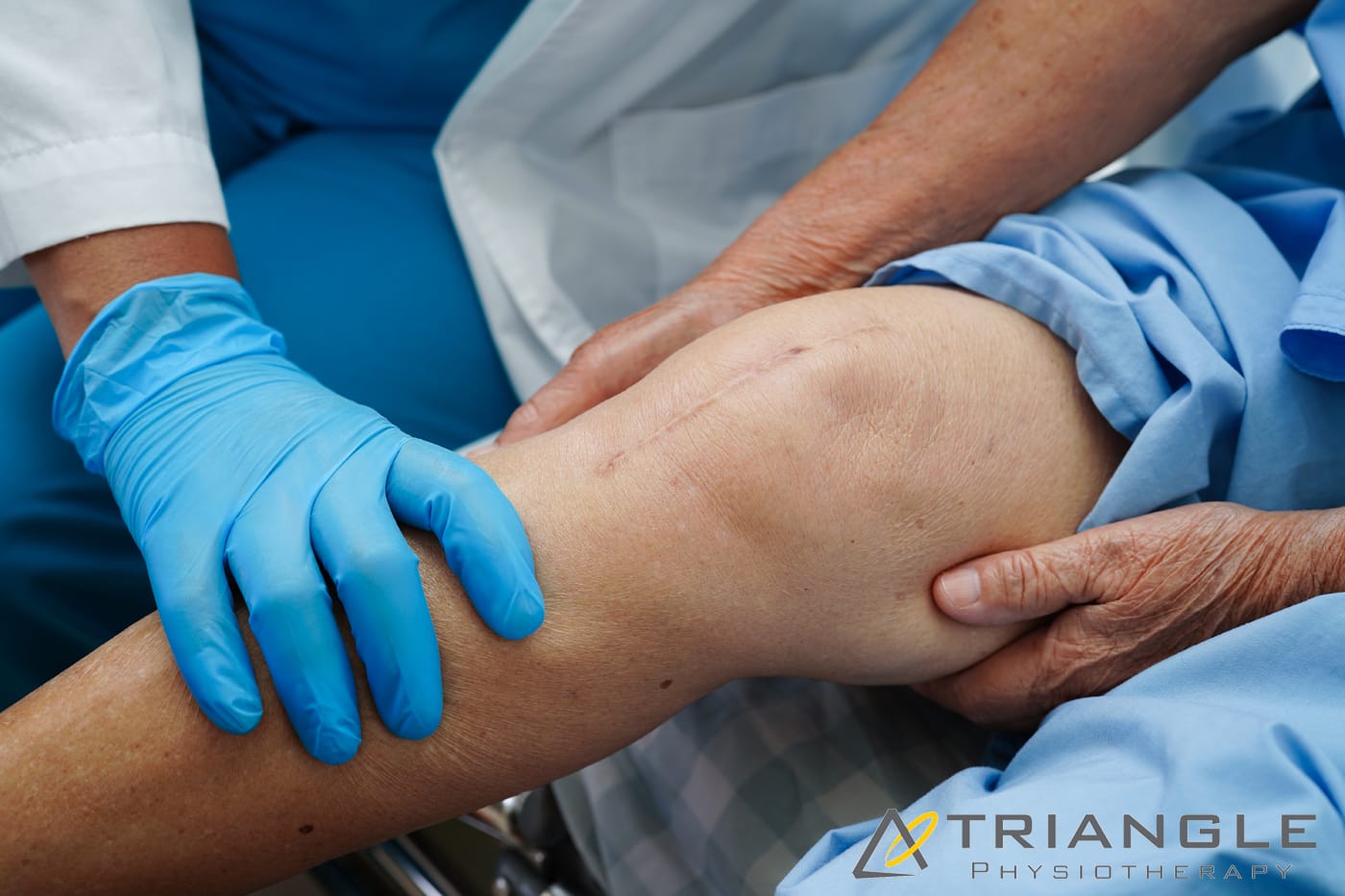
Recovering from orthopedic surgery is a crucial phase that sets the foundation for long-term mobility and quality of life. While surgery is a significant step toward healing, the recovery process often requires dedicated effort and guidance. This is where physiotherapy plays a vital role, helping patients regain strength, flexibility, and overall function. Triangle Physiotherapy can help you with your recovery journey post-surgery and safely transition back into your daily activities and sports.
Understanding Recovery from Surgery
Post-operative recovery involves more than just healing the surgical site; it encompasses rebuilding strength, restoring movement, and managing pain. Many patients face challenges like stiffness, weakness, and discomfort during this phase. Physiotherapy provides a structured approach to recovery, focusing on individualized treatment plans tailored to each patient’s specific needs. Engaging in physiotherapy early can significantly enhance recovery outcomes.
Neuromuscular Exercises for Recovery after Surgery
Neuromuscular exercises are designed to improve muscle coordination, strength, and balance. These exercises are particularly important after orthopedic surgery, as they help re-educate the muscles surrounding the surgical area. Examples include balance exercises, proprioceptive training, and targeted movements that activate specific muscle groups. By strengthening these muscles, patients can alleviate pain and improve stability, reducing the risk of future injuries.
Mobility Incorporation
Maintaining mobility is crucial during the recovery process. Physiotherapists incorporate mobility exercises, such as stretching and gentle range-of-motion activities, to help patients regain flexibility and prevent stiffness. Activities like yoga or tai chi may also be recommended, as they promote relaxation and enhance overall well-being. Incorporating mobility into daily routines not only aids in recovery but also encourages a healthier lifestyle.
Progressive Resistance Exercises
As recovery progresses, progressive resistance exercises become essential. These exercises gradually increase the intensity of strength training, allowing patients to build endurance and strength safely. Utilizing resistance bands, weights, or bodyweight, physiotherapists design programs that align with each patient’s recovery stage. This gradual approach ensures that patients do not overexert themselves while still making meaningful gains.
Prevention
Preventing future injuries is a significant aspect of post-operative care. Physiotherapists educate patients on proper body mechanics, ergonomics, and strategies to avoid movements that could lead to re-injury. By addressing risk factors and instilling healthy habits, patients can enhance their resilience and reduce the likelihood of setbacks.

FAQs
Can a physiotherapist help with my recovery?
Absolutely! Physiotherapists specialize in rehabilitation, offering tailored exercises and strategies to facilitate recovery from surgery.
What should I expect during my first visit to Triangle Physiotherapy?
During your first visit, you’ll undergo a thorough assessment where your physiotherapist will evaluate your condition, review your medical history, and discuss your recovery goals. A personalized treatment plan will be created based on this information.
How many sessions will I need?
The number of sessions varies based on your specific surgery and recovery progress. Some patients may see improvement in a few sessions, while others might require ongoing therapy. Your physiotherapist will provide an estimate during your assessment.
Do I need a referral to see a physiotherapist?
No, you do not need a referral to access physiotherapy services. You can book an appointment directly, unless your insurance requires it for billing purposes.
How soon can I expect pain relief?
Many patients report improvements within a few sessions, but the timeline can vary depending on individual circumstances and the nature of the surgery.
How can I ensure a smooth recovery?
Engaging in physiotherapy, following your rehabilitation plan, and incorporating exercises into your daily routine are essential for a successful recovery. Listening to your body and communicating with your physiotherapist will also help you stay on track.
Learn More About Pre and Post-Surgery Physiotherapy at Triangle Physiotherapy
Physiotherapy is integral to post-orthopedic surgery recovery. By understanding the recovery process, incorporating targeted exercises, and prioritizing prevention, patients can regain their independence and improve their quality of life. If you’re preparing for surgery or currently in recovery, consider the invaluable support that physiotherapy can offer.
If you would like to know more about how we can help you with your pre or post-surgery rehab, call us to schedule an initial assessment today!
Chronic pain, a persistent discomfort that lasts for more than three months, can significantly impact quality of life. Unlike acute pain, which typically results from an injury and subsides as the body heals, chronic pain persists for months or even years, often without a clear cause.
Effective management requires a multifaceted approach, including understanding the condition, seeking professional help, and incorporating lifestyle changes.
Understanding Chronic Pain
Chronic pain is often a complex issue with various underlying causes, such as injuries, illnesses, or neurological conditions. It can be a debilitating experience, leading to emotional distress, sleep disturbances, and social isolation. While there may not be a cure, effective management strategies can help individuals cope and improve their overall well-being.
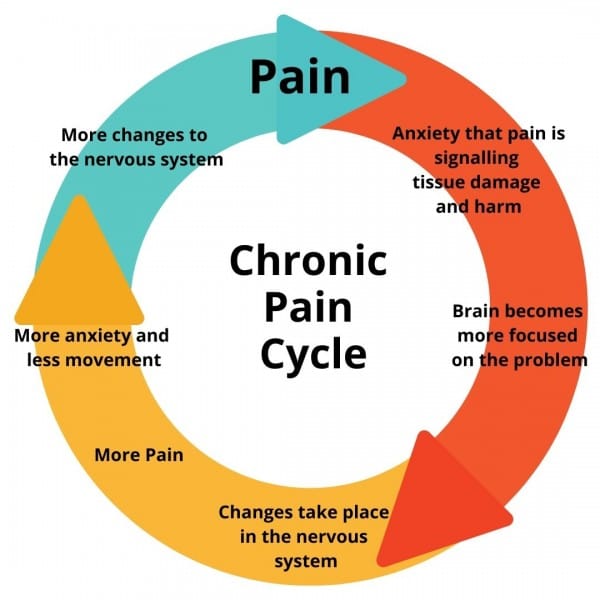
Picture Credit: Capital Area Physical Therapy and Wellness
The pain cycle refers to the self-perpetuating loop in which chronic pain leads to emotional, psychological, and physical responses that, in turn, intensify or prolong the pain. This cycle is common in individuals dealing with long-term pain and can be difficult to break without a comprehensive management plan.
Common Types of Chronic Pain:
- Lower Back Pain: Often caused by issues like herniated discs or spinal conditions.
- Arthritis Pain: Inflammation in the joints can cause persistent discomfort.
- Neuropathic Pain: This type of pain results from nerve damage, often felt as a burning or tingling sensation.
- Headaches and Migraines: Chronic headaches can disrupt daily life and often require specialized treatments.
- Fibromyalgia: A condition that causes widespread muscle pain and tenderness, often accompanied by fatigue.
Causes of Chronic Pain
Chronic pain can stem from a variety of causes, and sometimes, the exact cause remains unknown. Here are some common sources:
- Injuries: Past injuries, even when healed, can leave behind lingering pain.
- Medical Conditions: Diseases like arthritis, diabetes, and fibromyalgia are known to cause chronic pain.
- Nerve Damage: Neuropathic pain often arises from nerve injury or damage, such as after surgery or trauma.
- Inflammation: Conditions that cause inflammation, such as autoimmune diseases, can result in long-lasting pain.
- Psychological Factors: Stress, anxiety, and depression can exacerbate or even trigger chronic pain.
The Importance of Physiotherapy for Chronic Pain
Physiotherapy plays a crucial role in chronic pain management. A qualified physiotherapist can assess the root cause of the pain, develop a personalized treatment plan, and provide guidance on exercises and techniques to alleviate discomfort and improve function. Through targeted interventions, physiotherapy can help individuals regain strength, flexibility, and mobility, ultimately reducing pain and enhancing quality of life.
Managing Chronic Pain: Treatment Options
While chronic pain may not always be curable, it is manageable. A combination of therapies often yields the best results. Below are common methods used to treat and manage chronic pain:
1. Medications:
- Over-the-counter Pain Relievers: Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen or acetaminophen are often the first line of defense.
- Prescription Medications: In more severe cases, doctors may prescribe opioids, muscle relaxants, or antidepressants that also help relieve pain.
- Topical Treatments: Creams and patches containing pain-relief ingredients can be applied directly to the skin to ease localized pain.
2. Physiotherapy:
- Physiotherapy aims to strengthen muscles, improve flexibility, and reduce pain through movement. A tailored exercise plan can help prevent stiffness and alleviate chronic pain.
3. Cognitive Behavioral Therapy (CBT):
- Chronic pain can have a significant psychological impact. CBT helps patients manage their pain by changing the way they perceive and react to it. This therapy is also useful for dealing with anxiety and depression related to chronic pain.
4. Alternative Therapies:
- Acupuncture: This traditional Chinese medicine technique involves inserting thin needles into specific points of the body to reduce pain.
- Massage Therapy: Gentle massage can help relax muscles and reduce pain in some cases.
- Yoga and Meditation: Mind-body practices like yoga and meditation can help reduce stress, improve flexibility, and alleviate pain.
5. Lifestyle Changes:
While chronic pain can be difficult to prevent entirely, adopting healthy lifestyle habits can significantly reduce the risk and severity of symptoms. Regular exercise, a balanced diet, adequate sleep, and stress management techniques are essential components of a comprehensive approach. By addressing underlying health conditions and making positive lifestyle choices, individuals can improve their overall resilience and reduce the impact of chronic pain
For more information on how to reduce or manage chronic pain with physiotherapy, contact us at 416.207.9911 to make an appointment at one of our physiotherapy clinics:
Back pain is a common complaint that affects millions of people worldwide. It can range from a dull ache to sharp, debilitating pain. Understanding the causes, prevention strategies, and effective treatments is essential for managing this condition.
Understanding Back Pain
Back pain can arise from various sources, including poor posture, muscle strains, or injuries. Other factors such as age, obesity, and sedentary lifestyles can also contribute. Often, back pain stems from the muscles, ligaments, or discs in the spine becoming strained or injured. In some cases, underlying conditions like arthritis or herniated discs can cause chronic pain.
The good news is that the physiotherapists at Triangle Physiotherapy can help you manage back pain and prevent recurrence.
Importance of Physiotherapy when you have Back Pain
Physiotherapy plays a crucial role in both treating and preventing back pain. A physiotherapist can assess your condition, provide tailored exercises, and educate you on proper movement techniques. They can also help manage pain through modalities like heat therapy, ultrasound, or electrical stimulation. Early intervention can prevent the escalation of back issues and promote a quicker recovery.
What can I do if I have Back Pain?
The best thing you can do for any type of pain is to stay active. Whether it is walking, running or yoga, find an activity that keeps you moving.
Neuromuscular Exercises for Pain
Neuromuscular exercises focus on improving the communication between your brain and muscles, enhancing coordination and strength. These exercises can be particularly effective for back pain by stabilizing the spine and improving posture. Common neuromuscular exercises include:
- Bird-Dog: This exercise enhances core stability while promoting balance.

- Plank: Planks engage the entire core, supporting your back muscles.

- Bridge: This helps strengthen the glutes and lower back, essential for overall stability.

Progressive Resistance Training
Incorporating progressive resistance training into your routine can significantly reduce back pain. This type of training involves gradually increasing the weights you lift, which helps build muscle strength and endurance. Stronger muscles support your spine better, reducing the likelihood of injury. Focus on exercises that target your back, core, and lower body, such as deadlifts and rows, while ensuring you maintain proper form.
Incorporating Mobility into Your Daily Routine
Mobility exercises enhance flexibility and range of motion, which can alleviate back pain. Simple stretches like hamstring stretches, spinal twists, and hip flexor stretches can make a significant difference. Incorporate these into your daily routine—perhaps after waking up or during breaks at work. Mobility should be part of your lifestyle, not just an exercise program.
Tips for Safely Performing Exercises
Safety is paramount when exercising, especially if you’re managing back pain. Here are some tips to keep in mind:
- Warm-Up: Always start with a warm-up to prepare your muscles.
- Listen to Your Body: If an exercise causes pain, stop immediately.
- Use Proper Form: Focus on technique over weight to prevent injuries.
- Consult Professionals: Work with a trainer or physiotherapist, especially if you’re new to exercise or recovering from an injury.
Prevention
Preventing back pain is often more effective than treating it after it occurs. Here are some key strategies to help you avoid back issues:
- Maintain Good Posture: Be mindful of how you sit, stand, and lift objects. Keeping your back straight and your shoulders back can significantly reduce strain on your spine.
- Stay Active: Regular physical activity strengthens your back and core muscles, providing better support for your spine.
- Ergonomic Workspace: If you work at a desk, ensure your workstation is set up to promote good posture. Use chairs that offer proper lumbar support and position your computer screen at eye level.
Back pain can be a challenging and frustrating condition, but understanding its causes and implementing preventive measures can lead to relief. Always prioritize safety and seek professional guidance when needed. With the right approach, you can manage and reduce back pain, leading to a healthier, more active lifestyle.
Read also: Rehabilitation for Low Back Pain – Source: Physio Pedia
An ACL tear can be a significant setback, especially for athletes and active individuals. The ACL (anterior cruciate ligament), located in the knee, plays a crucial role in stabilizing and allowing movement. When it’s torn, physiotherapy becomes essential for a successful recovery. In this guide, we’ll explore the causes of ACL tears, prevention strategies, and the various physiotherapy techniques that can aid in recovery.
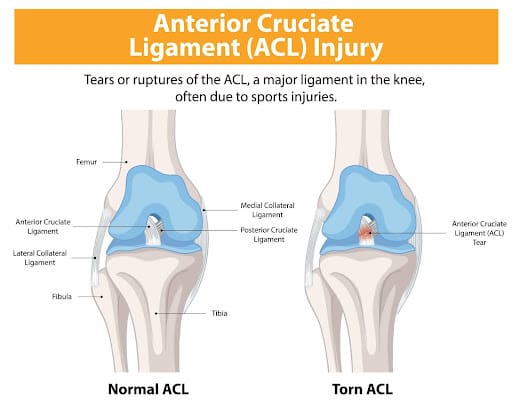
Causes of ACL Tears
What It Is: The ACL is a ligament in the knee that helps stabilize the joint and control movement. An ACL tear is a common knee injury, particularly in sports.
Common Causes:
- Sudden Stops and Starts: Rapid changes in direction or sudden stops can put excessive stress on the ACL.
- Direct Impact: A blow to the knee or a collision, common in contact sports like football or basketball, can cause the ACL to tear.
- Improper Landing: Landing awkwardly from a jump or fall can also strain the ACL.
Prevention Strategies
How to Reduce Risk: While not all ACL tears can be prevented, taking certain measures can significantly lower your risk.
- Strength Training: Strengthen the muscles around your knee, including the quadriceps, hamstrings, and calf muscles, to provide better support and stability.
- Proper Technique: Learn and practice proper techniques for jumping, landing, and pivoting to reduce stress on your knee.
- Warm-Up: Always warm up before engaging in sports or strenuous activities to prepare your muscles and joints for the demands ahead.
Resistance Exercises
Purpose: Resistance exercises help build strength in the muscles surrounding the knee, which is crucial for stabilizing the joint and aiding recovery. The ones mentioned below are to be performed in the latter stages of rehab, with professional help.
Examples:
- Squats: Perform squats with proper form to strengthen the quadriceps, hamstrings, and glutes.
- Leg Press: Use a leg press machine to work on lower body strength while controlling the range of motion.
- Lunges: Lunges help in building strength and balance in the legs, targeting various muscle groups around the knee.
How to Do Them Safely: Start with light weights or bodyweight, gradually increasing the resistance as your strength improves. Focus on maintaining proper form to avoid additional strain.

Neuromuscular Exercises
Purpose: Neuromuscular exercises enhance the communication between your brain and muscles, improving coordination and balance.
Examples:
- Balance Boards: Standing on a balance board helps improve stability and proprioception (awareness of your body’s position in space).
- Single-Leg Stands: Practice standing on one leg to strengthen stabilizing muscles and improve balance.
- Agility Drills: Incorporate ladder drills or cone drills to enhance agility and neuromuscular control.
How to Do Them Safely: Start with easier exercises and gradually progress to more challenging ones as your balance and coordination improve.

Progressive Exercises
Purpose: Progressive exercises are designed to gradually increase in difficulty, helping to build strength and endurance while avoiding overexertion.
Examples:
- Step-Ups: Begin with low steps and gradually increase the height as your strength and stability improve.
- Resistance Bands: Use resistance bands to add progressive resistance to leg exercises, adjusting the band’s tension as needed.
- Cycling: Start with short, low-resistance cycles and progressively increase duration and resistance.
How to Do Them Safely: Follow a structured program that gradually increases the intensity and complexity of exercises to prevent overuse injuries.
Stretching and Strengthening
Purpose: Stretching maintains flexibility and prevents stiffness, while strengthening exercises build the muscle support necessary for knee stability.
Examples:
- Hamstring Stretch: Gentle stretching of the hamstrings can help maintain flexibility and reduce tension in the knee.
- Quadriceps Stretch: Stretch the quadriceps to keep the front of the thigh flexible and balanced.
- Strengthening Exercises: Incorporate exercises like leg lifts and bridges to build muscle strength around the knee.
How to Do Them Safely: Perform stretching exercises slowly and hold each stretch for 20-30 seconds. Strengthening exercises should be done with controlled movements and proper form.
Mobility Routine
Purpose: A mobility routine focuses on improving the range of motion and function of the knee joint.
Examples:
- Knee Circles: Perform gentle knee circles to increase flexibility and mobility.
- Heel Slides: Lie on your back and slide your heel towards your buttocks to improve knee flexion.
- Straight Leg Raises: Lift your leg while keeping it straight to maintain and improve knee range of motion.
How to Do Them Safely: Ensure you’re performing exercises within a comfortable range of motion and avoid pushing through pain.
Tips for Safely Performing Activities
How to Stay Safe: As you recover and resume activities, following these tips can help prevent re-injury and ensure a safe return to your routine.
- Listen to Your Body: Pay attention to any pain or discomfort and modify your activities as needed.
- Gradual Return: Ease back into your regular activities and sports gradually to allow your knee to adjust.
- Use Supportive Gear: Consider using a knee brace or support during high-impact activities for added stability.
- Seek Professional Guidance: Work with a physiotherapist to develop a personalized rehabilitation program and get advice on technique and progression.
Physiotherapy Treatment of an ACL Sprain
A physiotherapist will examine both knees, comparing the injured knee to the uninjured one. During this exam, the physiotherapist will check your injured knee for signs of swelling, deformity, tenderness, fluid inside the knee joint, and discoloration. If the patient does not have too much pain and swelling, a physiotherapist will then evaluate the knee’s range of motion and will pull against the ligaments to check their strength. During the exam, the patient will have to bend their knee and the physiotherapist will gently pull forward or push backward on their lower leg where it meets the knee.
Based on the results of the patient’s exam, diagnostic tests may need to be performed to further evaluate the condition of the patient’s knee. These tests may include standard X-rays to check for ligament separation from bone or fracture. Tests may also include an MRI scan or a camera–guided knee surgery (arthroscopy). The expected duration of recovery depends on the severity of the patient’s knee sprain, their rehabilitation program, and what type of sports the patients play. In general, milder sprains heal within 2-4 weeks, whereas other types may take 4-12 months.
Looking to have an ACL Injury treated? Schedule an appointment today!
Contact our clinic to book an appointment with one of our physiotherapists to help you recover from your ACL injury!
Our Mississauga Physiotherapy Clinics are located at:
Pregnancy is a remarkable journey filled with joy and anticipation. However, it also brings various physical challenges, one of the most common being back pain. This blog explores the causes of pregnancy back pain and how physiotherapy can provide relief. We’ll delve into the benefits of pelvic health physiotherapy in Mississauga and the holistic approach it offers to expecting mothers.

Causes of Pregnancy Back Pain
Hormonal Changes
During pregnancy, the body produces a hormone called relaxin, which helps to loosen the ligaments in the pelvic area to prepare for childbirth. While necessary, this increased flexibility can lead to instability and back pain.
Weight Gain
The additional weight gained during pregnancy puts extra strain on the spine. This added pressure can cause discomfort and pain, particularly in the lower back.
Postural Changes
As the baby grows, the center of gravity shifts forward, leading to changes in posture. This can result in muscle strain and back pain as the body adjusts to the new alignment.
Stress
Emotional stress can cause muscle tension in the back, leading to pain. It’s essential to manage stress effectively during pregnancy to minimize its impact on physical health.
How Physiotherapy Can Help with Pregnancy Back Pain
Personalized Treatment Plans
Physiotherapy in Mississauga offers personalized treatment plans tailored to the specific needs of pregnant women. These plans focus on alleviating back pain through targeted exercises and techniques.
Pain Relief Techniques
Physiotherapists use a variety of techniques to relieve pregnancy back pain, including manual therapy, massage, and specific exercises designed to strengthen the back and core muscles.
Pelvic Health Physio in Mississauga
Pelvic health physiotherapy is a specialized branch of physiotherapy that focuses on the pelvic floor muscles, which play a crucial role during pregnancy and childbirth. Pelvic health physiotherapists in Mississauga helps in:
- Strengthening Pelvic Floor Muscles: Exercises to enhance the strength and function of these muscles.
- Improving Posture: Guidance on maintaining proper posture to reduce back strain.
- Breathing Techniques: Techniques to manage pain and improve overall comfort during pregnancy.
Benefits of Physiotherapy for Pregnancy Back Pain
Reducing Pain and Discomfort
Regular physiotherapy sessions can significantly reduce back pain and discomfort, improving the quality of life for expecting mothers.
Enhancing Mobility
Physiotherapy helps maintain and improve mobility, making daily activities easier and more comfortable.
Preparing for Childbirth
Pelvic physio in Mississauga not only alleviates back pain but also prepares the body for childbirth by strengthening the pelvic floor muscles and improving overall physical readiness.
Postpartum Recovery
Physiotherapy continues to be beneficial postpartum, aiding in the recovery process and helping new mothers regain their strength and mobility.
What do I do next?
Find the Right Physiotherapist in Mississauga


When looking for physiotherapy in Mississauga, it’s essential to find a qualified and experienced physiotherapist who specializes in pregnancy and pelvic health. Our Locations in Mississauga have trained and experienced pelvic health physiotherapists with advanced training in pelvic health including Labour and Delivery Prep.
Pregnancy back pain is a common but manageable condition. With the right approach, such as physiotherapy in Mississauga, expecting mothers can find relief and improve their overall well-being. Pelvic health physiotherapists at Triangle Physiotherapy in Mississauga offers specialized care that addresses the unique challenges of pregnancy, providing a holistic approach to pain management and preparation for childbirth. By incorporating physiotherapy into their prenatal care routine, pregnant women can enjoy a more comfortable and healthy pregnancy journey.
Triangle Physiotherapy has 2 locations in Mississauga to help you with your pregnancy-related back pain:
Triangle Physiotherapy Square One
Triangle Physiotherapy Erin Mills
“At Triangle Physiotherapy, we have multiple locations across the GTA, including Physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, and Liberty Village. Our clinics are dedicated to providing specialized care for pregnancy-related back pain, ensuring that every expecting mother receives the best possible treatment.”
Spinal fusion surgery is a medical procedure used to permanently join two or more vertebrae in the spine, eliminating motion between them. The goal of the surgery is to reduce pain, correct deformities, or improve stability in the spine.
When would I need Spinal Fusion Surgery?
Spinal fusion surgery is typically recommended for various spine conditions, including:
- Degenerative disc disease: When the discs between vertebrae break down, causing pain.
- Spondylolisthesis: When one vertebra slips forward over the one below it.
- Spinal stenosis: Narrowing of the spinal canal, leading to nerve compression.
- Scoliosis: Abnormal curvature of the spine.
- Fractures: Vertebrae that are broken or dislocated.
- Tumors: Removal of tumors that affect spinal stability.
- Infections: Infections that have caused damage to the vertebrae.
When do I start physiotherapy after surgery?
The timing of when to start physiotherapy after spinal fusion surgery depends on several factors, including the specifics of the surgery, the patient’s overall health, and the surgeon’s recommendations.
What does post-surgery rehab involve?
Immediate Postoperative Period (0-6 Weeks)
- Initial Phase: Physiotherapy may start in the hospital within a day or two after surgery. The focus is on gentle movements and exercises to improve circulation and prevent complications.
- Activities:
- Breathing exercises to prevent lung complications.
- Gentle leg movements like ankle pumps to improve blood flow.
- Log rolling technique for safe movement in and out of bed.
- Short, frequent walks to promote circulation and reduce stiffness.
Early Rehabilitation Phase (6-12 Weeks)
- When: Typically, more structured physical therapy begins around 4 to 6 weeks after surgery, depending on the surgeon’s assessment.
- Goals: Gradually increase mobility, start gentle strengthening exercises, and improve functional movements.
- Activities:
- Range of motion exercises.
- Gentle strengthening exercises for the core and lower extremities.
- Walking programs to gradually increase distance and duration.
- Education on proper body mechanics and posture.
Late Rehabilitation Phase (3-6 Months)
- When: Around 3 months post-surgery, assuming there are no complications.
- Goals: Restore full function, enhance strength and endurance, and improve posture and body mechanics.
- Activities:
- More advanced strengthening exercises using resistance bands or light weights.
- Low-impact aerobic exercises like swimming or cycling.
- Balance and coordination exercises.
- Functional training for daily activities.
Long-Term Rehabilitation Phase (6-12 Months)
- When: After 6 months, the patient should continue with physiotherapy based on individual progress and goals.
- Goals: Achieve optimal strength, flexibility, and functional ability, and prevent recurrence of symptoms.
- Activities:
- Progressive resistance training.
- Gradual reintroduction of higher-impact activities, if appropriate.
- Sport-specific training for athletes.
- Ongoing education on maintaining spine health.
Key Points to Consider
- Surgeon’s Recommendations: Always follow the specific guidelines and timelines provided by the surgeon, as they know the details of the surgery and individual patient needs.
- Listen to Your Body: Avoid pushing through pain. Pain is a signal that something might be wrong, and it’s important to communicate any discomfort to the physiotherapist or surgeon.
- Individual Variation: Each patient’s recovery is unique. Factors such as age, overall health, and the complexity of the surgery will influence the timing and intensity of physiotherapy.
Starting physiotherapy at the right time is crucial for a successful recovery, and adhering to a structured rehabilitation program can significantly enhance outcomes after spinal fusion surgery.
Click here to book an appointment for post-surgery rehab with a physiotherapist at one of our eight locations.
- Physiotherapy Etobicoke – Triangle Physiotherapy Etobicoke
- Oakville Physiotherapy Clinic – Triangle Physiotherapy Oakville
- Physiotherapy North York – Triangle Physiotherapy North York
- Mississauga Physiotherapy Clinics – Triangle Physiotherapy Mississauga
- Downtown Physiotherapy Clinics – Triangle Physiotherapy King West
- Uptown Physiotherapy Clinics – Triangle Physiotherapy Lawrence Park
- Physiotherapy Clinic Downtown Toronto – Triangle Physiotherapy Queens Quay
- Physiotherapy Clinics Mississauga – Triangle Physiotherapy Erin Mills
General Information: The information provided on this blog is for general informational purposes only. While we strive to ensure the accuracy and relevance of our content, we make no guarantees about the completeness, reliability, or accuracy of the information.
Not Professional Advice: The content on this blog does not constitute professional advice. It is not a substitute for professional medical, legal, financial, or other professional advice. Always seek the guidance of a qualified professional with any questions you may have regarding your specific situation.
Recovering from spinal fusion surgery requires careful physiotherapy to restore mobility and strength. Whether you need physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, or Liberty Village, there are expert physiotherapists available to guide your recovery journey and help you regain your quality of life.
Hiking is a fantastic way to enjoy the great outdoors and stay fit, but it can also pose some risks. Whether you’re new to hiking or a seasoned backpacker, there are numerous factors to take into account before heading out on the trails. You need to evaluate your backpack’s weight, choose appropriate footwear, plan your food and hydration, check the weather, and map out your routes. Additionally, since hiking often takes you off the beaten path, it’s essential to take precautions against three common hiking injuries: knee pain, ankle sprains, and sore feet.
Is it necessary to warm up before hiking?

Yes, it is necessary to warm up before hiking. Warming up helps prepare your muscles and joints for physical activity, reducing the risk of injury. Here are some reasons why warming up is important before hiking:
Benefits of Warming Up Before Hiking
- Increases Blood Flow: A proper warm-up increases blood flow to your muscles, delivering oxygen and nutrients that help them perform better.
- Enhances Flexibility: Warming up loosens your muscles and increases your range of motion, making it easier to navigate uneven terrain.
- Reduces Injury Risk: Warm muscles are less prone to strains, sprains, and other injuries.
- Prepares Your Heart: Gradually increasing your heart rate helps prepare your cardiovascular system for the more strenuous activity of hiking.
- Improves Performance: A good warm-up can improve your overall performance, making your hike more enjoyable and less exhausting.
What are some effective warm up exercises to do before hiking?
Effective Warm-Up Exercises
- Walking or Light Jogging: Start with 5-10 minutes of brisk walking or light jogging to get your blood flowing.
- Dynamic Stretches: Perform dynamic stretches like leg swings, arm circles, and torso twists to loosen up your muscles and joints.
- Ankle Rotations: Rotate your ankles in circles to prepare them for the uneven terrain.
- Hip Circles: Rotate your hips to loosen the hip joints, which are crucial for hiking.
- Calf Raises: Perform calf raises to warm up your calves, which are heavily used during hiking.
Taking a few minutes to warm up before you start your hike can make a significant difference in your overall hiking experience and help prevent injuries.
What are the most common hiking injuries?
Some of the most common hiking injuries are:
- Knee Pain
- Ankle Sprain
- Foot Pain
Knee Pain when Hiking
Knee pain is a common issue among hikers, especially on longer or more challenging trails. Here’s a comprehensive approach to understanding, preventing, and managing knee pain when hiking:
Causes of Knee Pain While Hiking
- Overuse and Strain: Continuous stress on the knee joint from uphill climbs, downhill descents, or long sessions of hiking.
- Improper Biomechanics: Poor hiking technique, such as improper foot placement or stride, can strain the knee joint.
- Previous Injuries: Past knee injuries or conditions like arthritis can flare up during hiking.
- Improper Gear: Worn-out or inappropriate footwear lacking proper cushioning and support.
Ankle Sprain when Hiking
An ankle sprain can be a painful and frustrating injury, especially when hiking in rugged terrain. Here’s how to understand, prevent, and manage ankle sprains while hiking:
Causes of Ankle Sprains While Hiking
- Uneven Terrain: Stepping on uneven surfaces, rocks, or roots can twist or roll the ankle.
- Fatigue: Muscles that support the ankle can become tired, leading to less stability and increased risk of injury.
- Inadequate Footwear: Wearing shoes or boots without proper ankle support or that are worn out.
Foot Pain when Hiking
Foot pain while hiking can be uncomfortable and distracting. Here’s how to understand, prevent, and manage foot pain effectively:
Causes of Foot Pain While Hiking
- Improper Footwear: Shoes or boots that are too tight, loose, worn out, or lacking proper cushioning and support.
- Overuse or Strain: Prolonged walking or hiking, especially on challenging terrain, can strain the muscles and joints of the feet.
- Blisters: Friction from improperly fitting shoes or moisture buildup can lead to painful blisters.
If you get injured while hiking, consult one of our physiotherapists who can help you with treating the injuries as well as advise and educate you on prevention so you can enjoy your outdoor activities without pain and discomfort.
Click here to book an appointment with a physiotherapist at one of our eight locations.
- Physiotherapy Etobicoke – Triangle Physiotherapy Etobicoke
- Oakville Physiotherapy Clinic – Triangle Physiotherapy Oakville
- Physiotherapy North York – Triangle Physiotherapy North York
- Mississauga Physiotherapy Clinics – Triangle Physiotherapy Mississauga
- Downtown Physiotherapy Clinics – Triangle Physiotherapy King West
- Uptown Physiotherapy Clinics – Triangle Physiotherapy Lawrence Park
- Physiotherapy Clinic Downtown Toronto – Triangle Physiotherapy Queens Quay
- Physiotherapy Clinics Mississauga – Triangle Physiotherapy Erin Mills
A rotator cuff tears are common injuries to the shoulder, involving a tear in one or more of the tendons of the rotator cuff muscles. It is one of the leading causes of shoulder pain and disability. The rotator cuff is a group of four muscles and their tendons that stabilize the shoulder and allow for its wide range of motion.
Understanding Rotator Cuff Tears: Causes and Symptoms
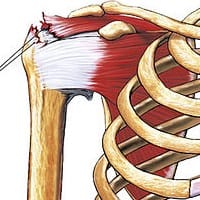
The rotator cuff is a group of four muscles and their tendons that stabilize the shoulder and allow for its wide range of motion. These muscles are:
- Supraspinatus
- Infraspinatus
- Teres minor
- Subscapularis
Types of Rotator Cuff Tears
- Partial Tear: This type of tear damages the tendon but does not completely sever it.
- Complete Tear: Also known as a full-thickness tear, this type involves the tendon being split into two pieces or pulled completely off the bone.
Causes
- Acute Injury: Sudden injuries, such as a fall on an outstretched arm or lifting something heavy with a jerking motion.
- Degenerative Wear and Tear: Gradual wear over time due to aging, repetitive stress from activities (like sports or certain jobs), or poor shoulder mechanics.
Symptoms
- Pain at rest and at night, particularly if lying on the affected shoulder
- Pain when lifting and lowering your arm or with specific movements
- Weakness in the shoulder
- Crackling sensation when moving the shoulder in certain positions
Importance of Physiotherapy in Rotator Cuff Tear Treatment
Physiotherapy plays a crucial role in the treatment and rehabilitation of rotator cuff tears. It can help in several ways, whether as a primary treatment for less severe tears or as a post-surgical rehabilitation strategy for more significant injuries. Here are some key points highlighting the importance of physiotherapy in rotator cuff tear treatment:
Pain Reduction
- Manual Therapy: Techniques such as massage and joint mobilization can help reduce pain and improve shoulder function.
- Modalities: Use of heat, ice, ultrasound, and electrical stimulation can help manage pain and inflammation.
Restoring Range of Motion
- Stretching Exercises: Specific stretches help maintain and gradually improve shoulder flexibility.
- Mobilization Techniques: Gentle mobilization can help increase the range of motion without causing further injury.
Strengthening Shoulder Muscles
- Strengthening Exercises: Focused on the rotator cuff and surrounding muscles, these exercises help restore strength and function to the shoulder.
- Progressive Resistance: Gradual increase in resistance helps to build muscle strength over time.
Improving Shoulder Stability
- Proprioceptive Training: Exercises that improve the body’s ability to sense the position and movement of the shoulder, enhancing stability.
- Functional Training: Exercises tailored to improve stability during daily activities and specific movements required in sports or work.
Enhancing Surgical Outcomes
- Pre-Surgical Physiotherapy (“Prehabilitation”): Strengthening and conditioning the shoulder before surgery can lead to better post-surgical outcomes.
- Post-Surgical Rehabilitation: Structured physiotherapy is essential to restore function, strength, and range of motion after surgery. It also helps minimize scar tissue formation and adhesions.
Preventing Further Injury
- Education: Teaching proper shoulder mechanics and ergonomic principles to avoid movements that can exacerbate the injury.
- Exercise Regimen: Developing a long-term exercise plan to maintain shoulder health and prevent future injuries.
Tailored Rehabilitation Programs
- Individualized Plans: Physiotherapists create personalized treatment plans based on the specific nature of the tear, the patient’s overall health, and their functional goals.
- Goal Setting: Setting realistic and progressive goals to keep the patient motivated and track progress.
Long-Term Shoulder Health
- Maintenance Exercises: Developing a routine of exercises to be continued even after formal physiotherapy ends to maintain shoulder health.
- Lifestyle Modifications: Advice on modifications to daily activities and sports techniques to protect the shoulder.
In summary, physiotherapy is an integral part of the comprehensive management of rotator cuff tears, offering a non-invasive approach to pain relief, functional restoration, and long-term shoulder health. It provides a structured and supportive environment for recovery, whether used alone or in conjunction with surgical treatments.
Click here to book an appointment with a physiotherapist at one of our eight locations.
- Physiotherapy Etobicoke – Triangle Physiotherapy Etobicoke
- Oakville Physiotherapy Clinic – Triangle Physiotherapy Oakville
- Physiotherapy North York – Triangle Physiotherapy North York
- Mississauga Physiotherapy Clinics – Triangle Physiotherapy Mississauga
- Downtown Physiotherapy Clinics – Triangle Physiotherapy King West
- Uptown Physiotherapy Clinics – Triangle Physiotherapy Lawrence Park
- Physiotherapy Clinic Downtown Toronto – Triangle Physiotherapy Queens Quay
- Physiotherapy Clinics Mississauga – Triangle Physiotherapy Erin Mills
“Rotator cuff tears require expert treatment and rehabilitation to restore function and reduce pain. Triangle Physiotherapy offers specialized care across the GTA. Whether you’re seeking Physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, or Liberty Village, our experienced team is here to help you on your recovery journey.”
The choice between physiotherapy and massage therapy depends on your specific needs, goals, and health conditions. Here’s a detailed comparison to help you decide which might be better for you:
Physiotherapy

What it is:
- A healthcare profession focused on diagnosing, managing, and preventing movement disorders.
- Uses exercises, manual therapy, education, and modalities like ultrasound and electrical stimulation.
Benefits:
- Rehabilitation: Effective for recovering from injuries, surgeries, and chronic conditions like arthritis.
- Pain Management: Addresses the root cause of pain through various techniques and exercises.
- Improved Mobility: Helps restore function and movement, particularly after injury or surgery.
- Preventive Care: Offers strategies to prevent future injuries or manage chronic conditions.
- Customized Treatment: Tailors plans based on individual assessments and needs.
Common Conditions Treated:
- Musculoskeletal injuries (e.g., sprains, fractures)
- Neurological conditions (e.g., stroke, multiple sclerosis)
- Cardiopulmonary issues (e.g., chronic obstructive pulmonary disease)
- Post-surgical rehabilitation
Massage Therapy

What it is:
- A practice involving the manipulation of soft tissues (muscles, tendons, ligaments) to enhance well-being.
- Uses techniques like stroking, kneading, and applying pressure.
Benefits:
- Relaxation: Promotes overall relaxation and stress relief.
- Pain Relief: Alleviates muscle tension and pain.
- Improved Circulation: Enhances blood flow, which can aid in healing.
- Flexibility: Increases range of motion and reduces stiffness.
- Mental Health: Can improve mood and reduce symptoms of anxiety and depression.
Common Conditions Treated:
- Muscle tension and soreness
- Stress-related conditions
- Chronic pain (e.g., back pain, fibromyalgia)
- Sports injuries
- Headaches and migraines
Which is Better for You?
- For Injury Rehabilitation or Chronic Conditions:
- Physiotherapy is typically more suitable as it provides a structured approach to recovery, addressing the underlying causes of your condition.
- For Stress Relief and Muscle Tension:
- Massage Therapy can be highly effective if your primary goal is relaxation and relief from muscle tightness.
- For Pain Management:
- Both can be effective, but the choice depends on the cause of the pain. Physiotherapy is often better for pain related to injury or chronic conditions, while massage therapy can be great for muscle-related pain.
- For Improved Mobility and Function:
- Physiotherapy focuses on restoring function and movement, making it the better choice for mobility issues.
- For Preventive Care:
- Physiotherapy provides long-term strategies to prevent injuries and manage chronic conditions.
- For Overall Well-being and Relaxation:
- Massage Therapy is beneficial for enhancing general well-being, reducing stress, and promoting relaxation.
Combination of Both:
- In some cases, a combination of physiotherapy and massage therapy can be beneficial. For example, physiotherapy can address the underlying issues, while massage therapy can help manage symptoms and improve overall well-being.
Conclusion:
Consult with a healthcare professional to get a personalized recommendation based on your specific health needs and goals. They can help you decide the best course of action and whether one or a combination of both therapies is ideal for you.
Click here to book an appointment with a physiotherapist and massage therapist at one of our eight locations.
- Physiotherapy Etobicoke – Triangle Physiotherapy Etobicoke
- Oakville Physiotherapy Clinic – Triangle Physiotherapy Oakville
- Physiotherapy North York – Triangle Physiotherapy North York
- Mississauga Physiotherapy Clinics – Triangle Physiotherapy Mississauga
- Downtown Physiotherapy Clinics – Triangle Physiotherapy King West
- Uptown Physiotherapy Clinics – Triangle Physiotherapy Lawrence Park
- Physiotherapy Clinic Downtown Toronto – Triangle Physiotherapy Queens Quay
- Physiotherapy Clinics Mississauga – Triangle Physiotherapy Erin Mills
Choosing between physiotherapy and massage therapy depends on your specific needs and health goals. Both can be beneficial for pain relief and overall wellness. For those looking for physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, or Liberty Village, there are skilled practitioners available to help you decide the best approach for your situation.