What Is Bell’s Palsy?
Bell’s palsy, also known as idiopathic facial palsy, is a sudden weakness or paralysis on one side of the face. It is caused by inflammation on the facial nerve, which is usually temporary.
What are the symptoms of Bell’s palsy?
- The most common symptom of Bell’s palsy is the sudden weakness or paralysis on one side of your face causing it to droop.
- Drooling.
- Eye issues such as excessive tearing or a dry eye.
- Altered taste.
- difficulty eating and drinking
- Sensitivity to sound.
- Pain in or behind your ear.
- Numbness in the affected side of your face.
- Dry mouth
What are the causes of Bell’s palsy and what Is the main cause of Bell’s palsy ?
Bell’s palsy is facial nerve paralysis of unknown cause but it’s often related to having a viral infection. Viruses that have been linked to Bell’s palsy include viruses that cause:
Some viruses which have been believed to be common Bell’s palsy causes are:
- Cold sores and genital herpes (herpes simplex)
- Chickenpox and shingles (herpes zoster)
- Mumps
- Flu
- Infectious mononucleosis (Epstein-Barr)
Other conditions that may cause Bell palsy are:
- HIV infection
- Lyme disease
- Middle ear infection
- Sarcoidosis
What is the best cure for Bell’s palsy and what happens If Bell’s palsy Is untreated?
Most people with Bell’s palsy fully recover even without treatment. But some medications or physiotherapy can help speed up Bell’s palsy recovery. Some studies showed that about one third of untreated Bell’s Palsy patients suffered from long term effects such as facial spasms and disfigurement, and chronic pain.
The best Bell’s palsy treatment will vary between individuals but most will be prescribed corticosteroids to reduce the facial nerve inflammation of the facial nerves. Some patients may be prescribed antiviral drugs like acyclovir to speed up the recovery process.
What Is The Best Treatment For Bell’S Palsy?
Bell’s palsy improves without treatment. Still, your healthcare provider may recommend one or more of these therapies for symptom relief and a faster recovery:
Another effective Bell’s palsy treatment is eye care which is crucial in protecting the eyes from injuries and irritants. If your eye does not close completely, the use of glasses or goggles is beneficial. An eye patch can be used at night.
Decompression surgery to ease nerve pressure eases pressure but it is rarely done because it may cause permanent nerve damage and loss of hearing.
Another beneficial treatment for Bell’s Palsy is Physiotherapy.
A registered physiotherapist can assist with providing education and support during recovery in order to reduce secondary complications.
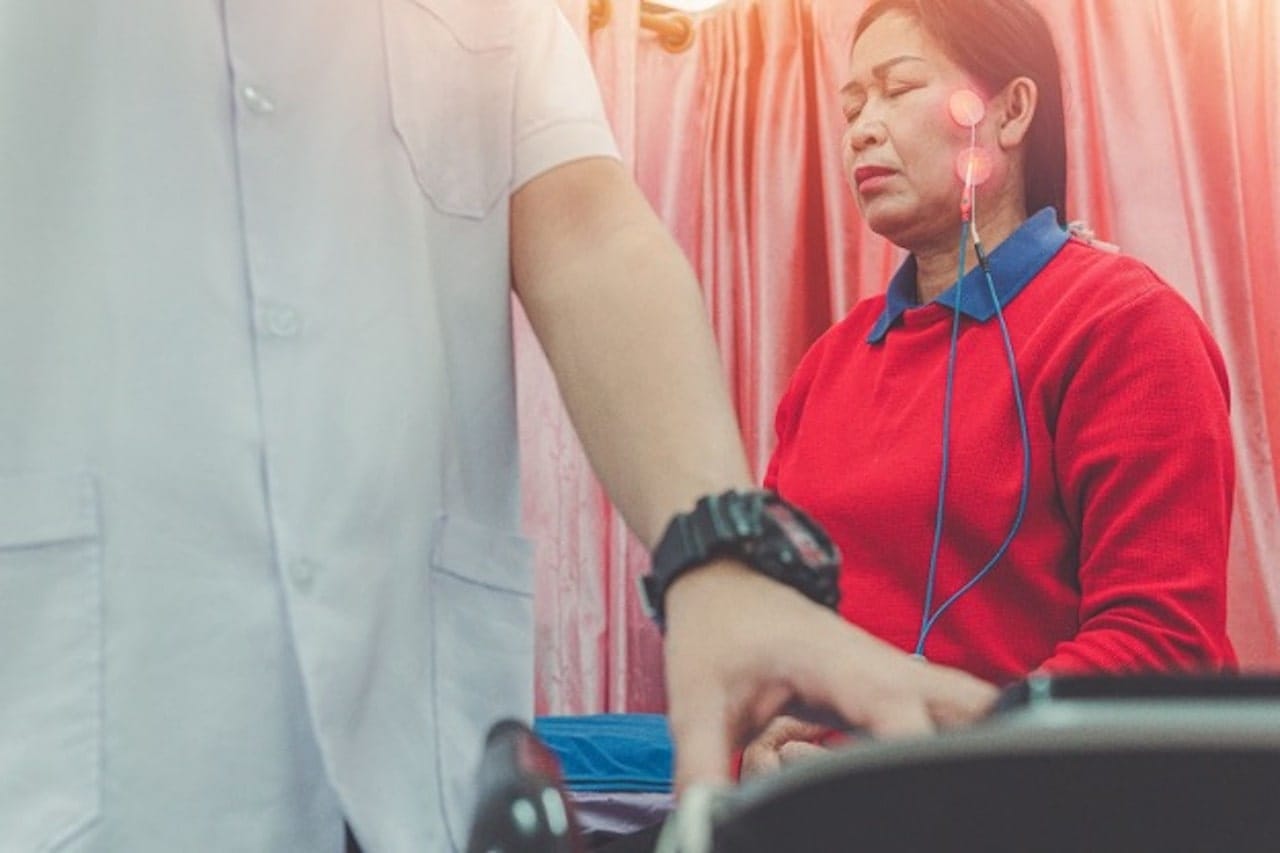
- Electrical muscle stimulation is used to stimulate the nerve fibers in order to help maintain some of the strength, which then promotes faster recovery,
- Daily exercise regimen
- Soft tissue massage can be applied to the head and face to help with aches and help stimulate repair of innervation for the facial muscles.
Recovery from Bell’s Palsy
In general, people whose paralysis is less severe tend to start to improve with or without treatment after a few weeks, with complete recovery of facial function within six months. If symptoms start to improve within the first 21 days, chances are there will be complete recovery with no residual facial muscle weakness.
At Physiotherapy Oakville, we understand the importance of early intervention and personalized care in facilitating recovery. Scientific studies have shown that timely physiotherapy can enhance the recovery process for facial paralysis, minimizing residual muscle weakness and improving overall outcomes. By joining Physiotherapy Oakville, you gain access to expert physiotherapists who provide evidence-based treatments tailored to your specific condition, supporting a faster and more complete recovery.
What are the complications Of Bell’s palsy?
Some of the complications of Bell’s palsy are:
- Irregular regrowth of nerve fibers and irreversible damage to your facial nerve which can result in synkinesis. Synkinesis is a condition in which moving one part of your face causes involuntary contraction of another.
- Excessive eye dryness on your affected side, which can lead to eye infections or even vision loss.
- Some people don’t fully recover and are left with long term facial paralysis and drooping.
Bell’s Palsy versus Stroke
Cause
The cause of Bell’s palsy is uncertain but some viruses like herpes zoster, herpes simplex, and mumps have been believed to be connected to Bell’s palsy.
Stroke is caused by high blood pressure, heart disease, high cholesterol, previous stroke.
Diagnosis
Bell’s palsy does not require any specific testing. Your doctor may ask you to perform specific facial movements such as eyebrow raising, frowning, smiling, and eyes closing. At times, EMG or MRI may be conducted to rule out stroke.
Diagnosing strokes is dependent on several factors. Some imaging scans are used to assess the brain and its blood supply.
Treatment
Treatment of Bell’s palsy are corticosteroids and antiviral medications, pain medications, and physiotherapy.
There is a more complex approach in treating stroke and its treatment is dependent on the type of stroke.
Our More Locations
Physiotherapy Etobicoke | Physiotherapy Oakville | Physiotherapy North York | Physiotherapy Toronto | Physiotherapy Lawrence Park | Physiotherapy Mississauga | Physiotherapy Queens Quay | Physiotherapy Mississauga Erin Mills | Physiotherapy Liberty Village
Click HERE to book an appointment with a physiotherapist at one of our eight locations.
- Physiotherapy Etobicoke – Triangle Physiotherapy Etobicoke
- Oakville Physiotherapy Clinic – Triangle Physiotherapy Oakville
- Physiotherapy North York – Triangle Physiotherapy North York
- Mississauga Physiotherapy Clinics – Triangle Physiotherapy Mississauga
- Downtown Physiotherapy Clinics – Triangle Physiotherapy King West
- Uptown Physiotherapy Clinics – Triangle Physiotherapy Lawrence Park
- Physiotherapy Clinic Downtown Toronto – Triangle Physiotherapy Queens Quay
- Physiotherapy Clinics Mississauga – Triangle Physiotherapy Erin Mills
“Addressing Bell’s Palsy and related back pain requires a comprehensive approach, including specialized stretches and physiotherapy. Triangle Physiotherapy offers expert services across the GTA, including Physiotherapy in Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, and Liberty Village. Our experienced physiotherapists can help you manage symptoms and improve your quality of life through personalized treatment plans.”
Shoulder Prehabilitation (prehab) involves the process of implementing a physical, psychological, nutritional intervention before an individual goes into surgery. The goal behind prehab programs is to maximize an individual’s physical and psychological fitness/health before surgery in order to reduce pain, increase physical function and allow you to return to your normal activities sooner following surgery.
Although there is limited evidence regarding shoulder prehab programs, there is promising and growing evidence that suggests prehab programs for hip, knee, and spinal surgery may improve pain, function and reduce the total cost of healthcare spending in the post-operative period.
Also Read, Physiotherapy Clinics in Etobicoke
Types of Surgeries for Shoulder
- Reverse arthroplasty
- Total shoulder arthroplasty/replacement
- Rotator cuff repair
- SLAP repair
- Bicep tendon repair
- Tenotomy
What Prehab Programs look like:
Most prehab programs can be anywhere from 2-8 weeks leading up to surgery and could potentially involve:
1) Exercise training (2-3x/week)
- Strengthening and stabilization exercises for the rotator cuff and muscles supporting your shoulder blade
- Home exercise program tailored to your needs
- Exercise training 1 on 1 with a physical therapist
2) Education: information delivered regarding
- Shoulder anatomy and mechanics
- Pain science education
- The process of your operative procedure
- Patient-therapist expectations
- Post-operative protocol
- Detailed exercise program and technique
Also read, Best Physiotherapist near Mississauga
3) Nutritional support
- Consultation with a registered dietician
- Detailed nutrition programs to optimize physical and mental health
- Nutritional supplements as indicated
4) Psychological support
- Consultation with psychologist/ psychotherapist
- Anxiety and stress reduction
- Cognitive-behavioral therapy
- Relaxation techniques
- Coping strategies for surgery
Shoulder Prehab is a set of exercises and movements designed to strengthen and condition the shoulder joint and surrounding muscles, helping to prevent injury or improve recovery from a previous injury. Prehabilitation may include:
- Shoulder rotator cuff strengthening exercises such as internal and external rotation with light weights.
- Scapular stability exercises to improve posture and reduce stress on the shoulder joint.
- Stretching to improve flexibility and range of motion.
- Plyometric exercises to improve power and explosiveness.
- Core stability exercises to improve overall body control and stability.
Prehabilitation should be performed regularly, especially if you have a history of shoulder injuries or plan to participate in overhead activities such as weightlifting or throwing. By taking care of your shoulder before it becomes a problem, you can help prevent injury and improve your performance.
Click HERE to book an appointment with a physiotherapist at one of our eight locations.
- Physiotherapy Etobicoke – Triangle Physiotherapy Etobicoke
- Oakville Physiotherapy Clinic – Triangle Physiotherapy Oakville
- Physiotherapy North York – Triangle Physiotherapy North York
- Mississauga Physiotherapy Clinics – Triangle Physiotherapy Mississauga
- Downtown Physiotherapy Clinics – Triangle Physiotherapy King West
- Uptown Physiotherapy Clinics – Triangle Physiotherapy Lawrence Park
- Physiotherapy Clinic Downtown Toronto – Triangle Physiotherapy Queens Quay
- Physiotherapy Clinics Mississauga – Triangle Physiotherapy Erin Mills
Shoulder prehabilitation is essential for preventing injuries and optimizing recovery, especially for those undergoing surgery or managing shoulder pain. If you’re looking for professional physiotherapy services for shoulder prehabilitation, there are several clinics in physiotherapy Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, and Liberty Village. These locations offer specialized care to help you strengthen your shoulders and maintain overall joint health.
One of the most common runners’ complaints is Shin splints (also known as Medial Tibial Stress Syndrome (MTSS)). The word shin splints describes pain/discomfort that gets worse during running or exercise around the front of the lower shin. Shin splints are usually developed by overuse, and a registered physiotherapist will do a detailed assessment to diagnose shin splints and develop a treatment plan to resolve them.
Shin splints are painful and uncomfortable but here are a few tips to effectively manage them.

Woman suffering from an ankle injury while exercising. Running sport injury concept.
Rest
Shin splints are considered an overuse injury. In the short term, rest will help the pain, and it is advised to rest for a period of time before beginning to run again. Start with shorter, slower distances instead of jumping right back into long distances when you start running again. Start running once a week and work up to twice a week if you usually run 3 days a week.
Also read, Best physsiotherapy clinic in Oakville
Ice
Place ice packs on your shins for a few minutes at a time. Icing will not treat your shin splints but will help effectively manage your pain after running.
Change up your workout routine
Adding resistance training to your workout routine can help reduce your pain by helping your muscles & tendons increase their capacity. Incorporating other types of aerobic exercise into your routine, like cycling, rowing, or the elliptical in place of running, can also help. Shin splints commonly come from the impact from running on hard or uneven surfaces. Replacing running with a different type of exercise once a week can help.
Stretching, warm-ups and cool-downs
Stretch your calves and shins before running to increase the flexibility in your legs. Warm-up before your workout to prepare your muscles and cool down at the end of it to help your muscles recover.
Also read, Best Physiotherapy Clinic in Missisuaga
Footwear & Orthotics
Think about how long you have had your running shoes. Good shoes are important as they act as shock absorbers every time your foot hits the ground. If the sole of the shoe is worn, shoes lose their shock absorption. Try a new pair of shoes with more cushioning and see how you get on.
Also, consider seeing a chiropodist for a pair of orthotics. Custom orthotics can help align and stabilize your foot and ankle, taking stress off of your lower leg. They can also be beneficial if you have flat feet.
Our physiotherapists at Triangle Physiotherapy can help resolve your shin splints and get you back to running or any other sport that you may love! Call us to book your assessment or book online here.
If you’re suffering from shin splints, professional physiotherapy can help with pain management and recovery through targeted exercises and treatments. For those in need of physiotherapy services, there are reputable clinics in physiotherapy Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, and Liberty Village. These locations offer expert care to help you recover from shin splints and get back to your daily activities pain-free.
We’ve all heard how good running can be for you. Running helps to lose weight, prevent disease, lower stress, strengthen joints, manage blood pressure… the list goes on and on. But there’s a suprising problem you may be experiencing if you’re a long distance runner. It’s called leaky gut. I know, it sounds gross, but if you’re a runner then it’s something to keep in mind. How do you know if you have a leaky gut? Read on to find out common symptoms and how to treat it.
What is leaky gut, anyway?
Leaky gut, also known as intestinal permeability, is a dysfunction in the lining of our intestine. Our intestinal walls are only one cell layer thick. Their job is to absorb nutrients and prevent bacteria from getting into our bloodstream. When the cells of the gut lining start to separate and let bacteria enter the bloodstream, we get what we call leaky gut. This can lead to all kinds of health issues, including:
- allergies
- asthma
- autoimmune disease
- eczema
- psoriasis
- rheumatoid arthritis
- food sensitivities
- irritable bowel syndrome
- Crohn’s disease
- ulcerative colitis
- thyroid problems
- acne
- nutrient deficiencies
- depression and other mood disorders
Also read, Physiotherapy Treatment in Mississuaga
How does running lead to leaky gut?
It’s actually not just running that can lead to leaky gut. Powerlifters and people who do cross-fit are at risk, too. Same goes for anyone who does vigorous strength training or heavy exercise. The gut lining becomes more permeable due to the amount of stress put on your body by these types of activity. High physical stress leads to higher metabolic demands. Endurance sports do appear to have the most profound effect on leaky gut though, which is why you might be more concerned if you’re a marathon runner, cyclist, or triathlete.
When you exercise, plant-derived carbohydrates are digested and fermented by the gut. This can create some harmful byproducts that play a role in creating leaks in your gut. Once you have a leaky gut, toxins are more easily able to cross from your intestines into your bloodstream.
Also read, Physiotherapy Treatment in Oakville
Endurance exercise can also increase our secretion of pro-inflammatory cytokines. This means that more inflammation is happening in the gut, which can throw off the balance of good bacteria versus bad bacteria in the intestines.
If you know me, you know I don’t like talking about health issues without some scientific studies to back up what I’m saying. So let’s take a look at one. Researchers looked at LPS (lipopolysaccharide) levels in athletes. They chose to look at LPS because it is a toxin found in bacteria. They measured LPS from blood samples of 29 athletes before, immediately after, one hour after, two hours after, and 16 hours after a triathlon. What they found was that LPS in the blood increased immediately after the race. But guess what? LPS was even higher than that one hour later. This demonstrated that there was an increase in leaky gut both during and after intense exercise.
I think I might have a leaky gut… now what?
Don’t hang up your running shoes just yet, folks. There might be a solution to those leaks in your gut. Remember how I mentioned that the balance between good and bacteria in the gut can get thrown off? Well, one way to help restore that balance is by taking probiotics. Probiotics are known as the good, healthy bacteria that we want and need in our gut. There are many different strains of probiotics. The two that have been shown to be most helpful with leaky gut is called Lactobacillus and Bifidobacterium. These strains help cells of the intestinal wall to tighten up the gaps between them.
A study demonstrated that probiotic supplements reduced LPS levels in the blood. This led to less leaky gut as well as an increase in the amount of time it took to reach fatigue while exercising in hot temperatures. This means that probiotics could actually help to improve athlete performance, too!
If you are a runner and suspect you may have a leaky gut, don’t wait until deteriorating health issues come along. Act now by calling the clinic to book your appointment with Dr. Corina Kibsey, ND today.
Runners often face various issues that can benefit from targeted physiotherapy to prevent injuries and improve performance. If you need professional physiotherapy care, consider visiting clinics in physiotherapy Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, and Liberty Village. These clinics offer specialized services tailored to the needs of runners, helping them stay healthy and achieve their fitness goals.
Our knees support the weight of our bodies with each step we take. When we begin to experience knee pain, it can be very debilitating, especially if the pain is severe. Some common causes of knee pain are: joint strain or damage, patellar maltracking, obesity, poor foot biomechanics, and many others. In some cases, severe osteoarthritis (OA) can be the cause of the knee pain. While exercises are extremely beneficial in building muscular support and managing the effects of the OA, a knee brace can be a good intervention to provide support and delay any surgical intervention. It can help to reduce swelling and pressure on the joints and can shift weight away from the damaged and painful areas of the joint. This can significantly improve a person’s mobility by decreasing their pain.
What is Osteoarthritis?
Osteoarthritis (OA) is the most common joint condition. At its core, it is the deterioration of the cartilage which lines our joints and makes movement fluid and pain-free. While mild OA is a normal age-related change, severe OA involves a significant reduction in the amount of lubricating fluid (known as synovial fluid) within the joint. This can cause significant pain with movement, stiffness, and imbalance because of a more bone-on-bone type of feeling.
Also read, Best Physiotheraoy clinic in Mississauga
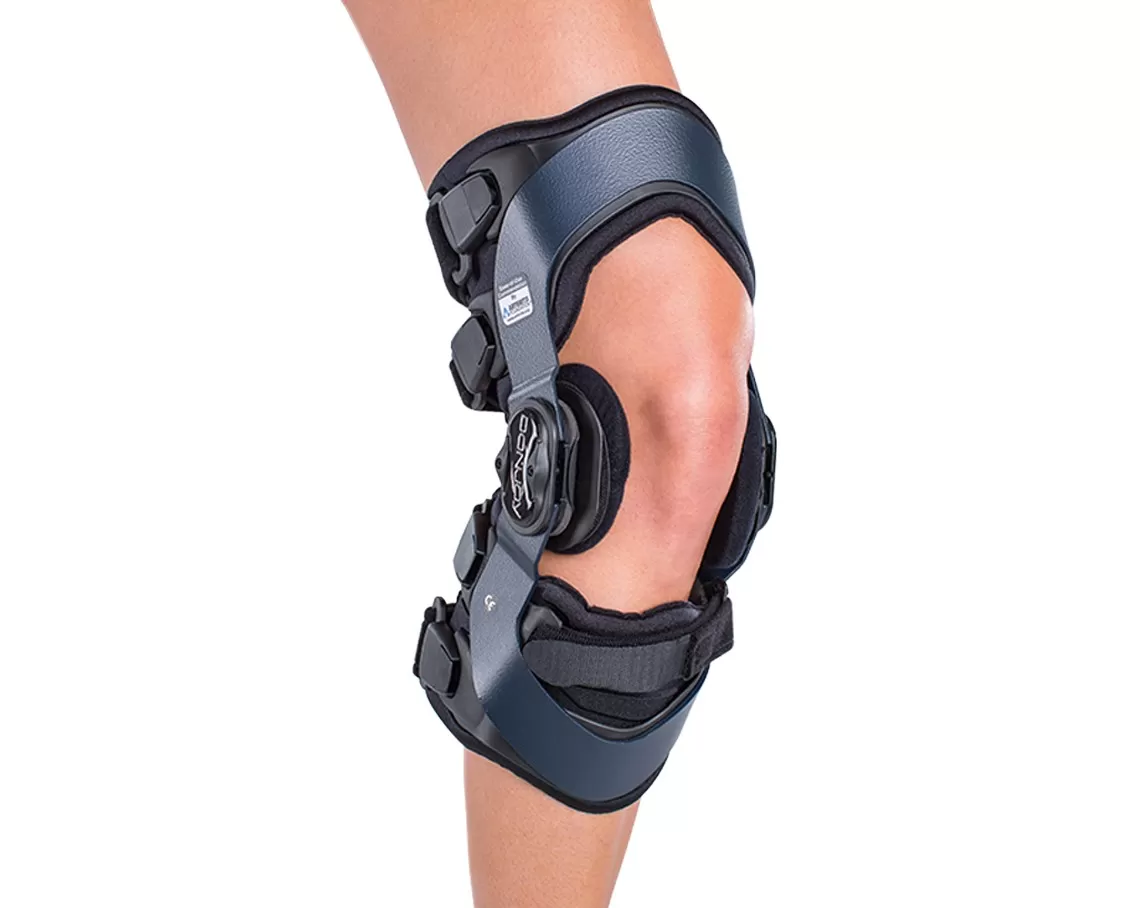
Knee brace for Osteoarthritis
As mentioned above, a knee brace can be a good management option for dealing with the effects of OA. A good knee brace will offer the support you need in order to balance and evenly distribute your weight in order to have a more comfortable walk or run. Material used to make braces can be plastic, metal, or sometimes composite materials. In addition, synthetic rubber is used for positioning and padding. It’s made in way so that your skin can breathe while your knees are supported.
Also read, Best Physiotherapy Clinic in Oakville
Types of knee braces in osteoarthritis
There are three styles of braces: Basic, Compression and Unloader for three different levels of support.
- Basic braces are for those who suffer from mild pain that worsens with activity and motion. Most people wear them while exercising or walking/running for long periods of time.
- Compression sleeves/advanced braces provide support for moderate osteoarthritic pain. They are generally worn during exercise in order to keep the joints warm and hold the knees in proper alignment.
- Unloader braces are for severe osteoarthritis. They are worn when a person is suffering from severe pain due to their knee OA and will physically unload the joint, causing less pressure to go through it.
We at Triangle physiotherapy will assess you knee joints and develop a complete treatment plan for you. Our expert physiotherapists can help you choose the correct knee brace to manage your OA. Book your appointment now and feel some relief so you can get back to your normal life as soon as possible!
Visit Here: http://www.trianglephysiotherapy.com
Using a knee brace can help manage osteoarthritis pain and improve mobility, but combining it with physiotherapy provides the best results. For personalized physiotherapy care, consider clinics in physiotherapy Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, and Liberty Village. These locations offer specialized treatment plans to support knee health and enhance your quality of life.
- Bones and joints
- Ligaments and tendons
- Muscles
- Nerves
- Blood vessels
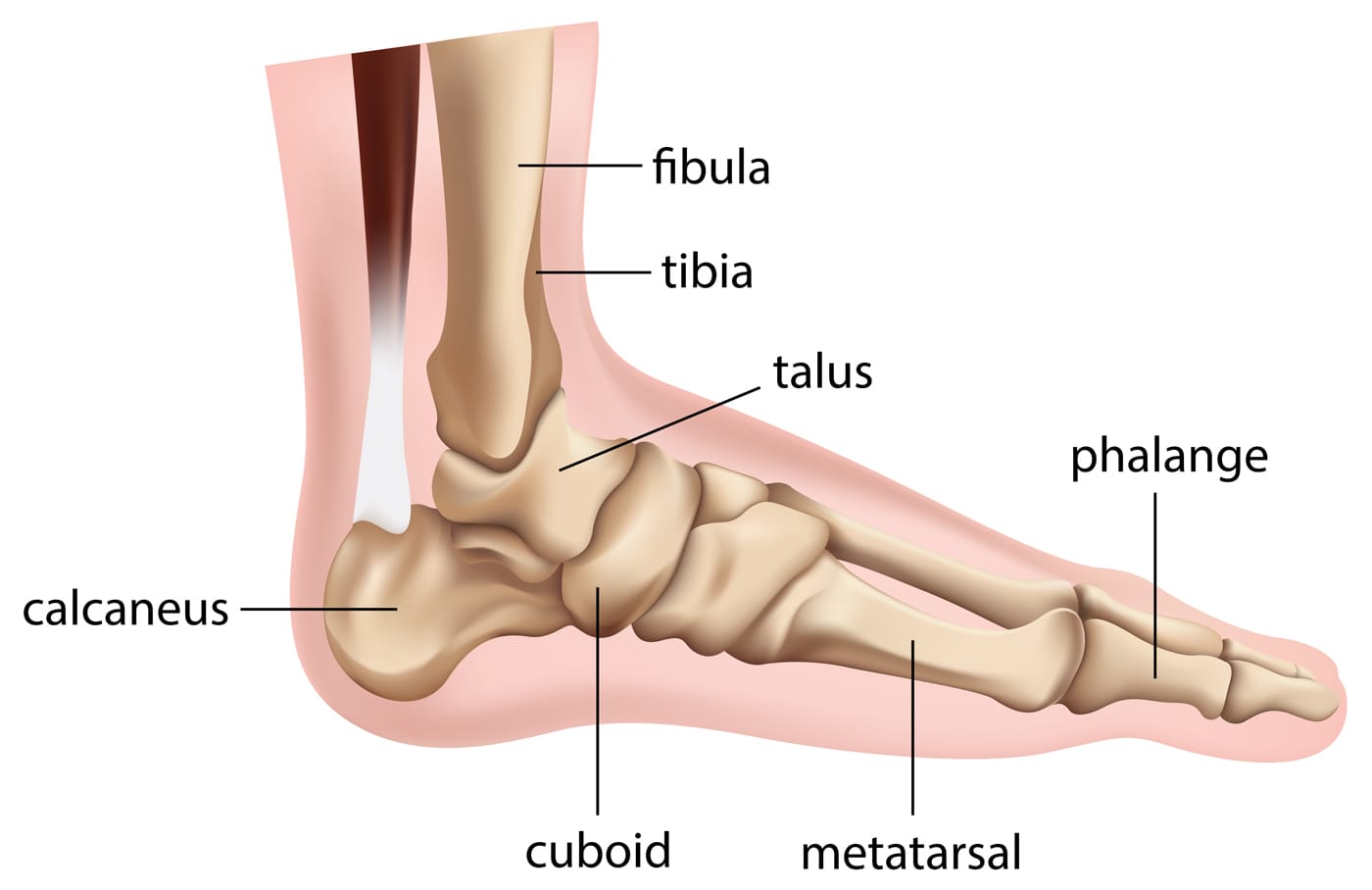
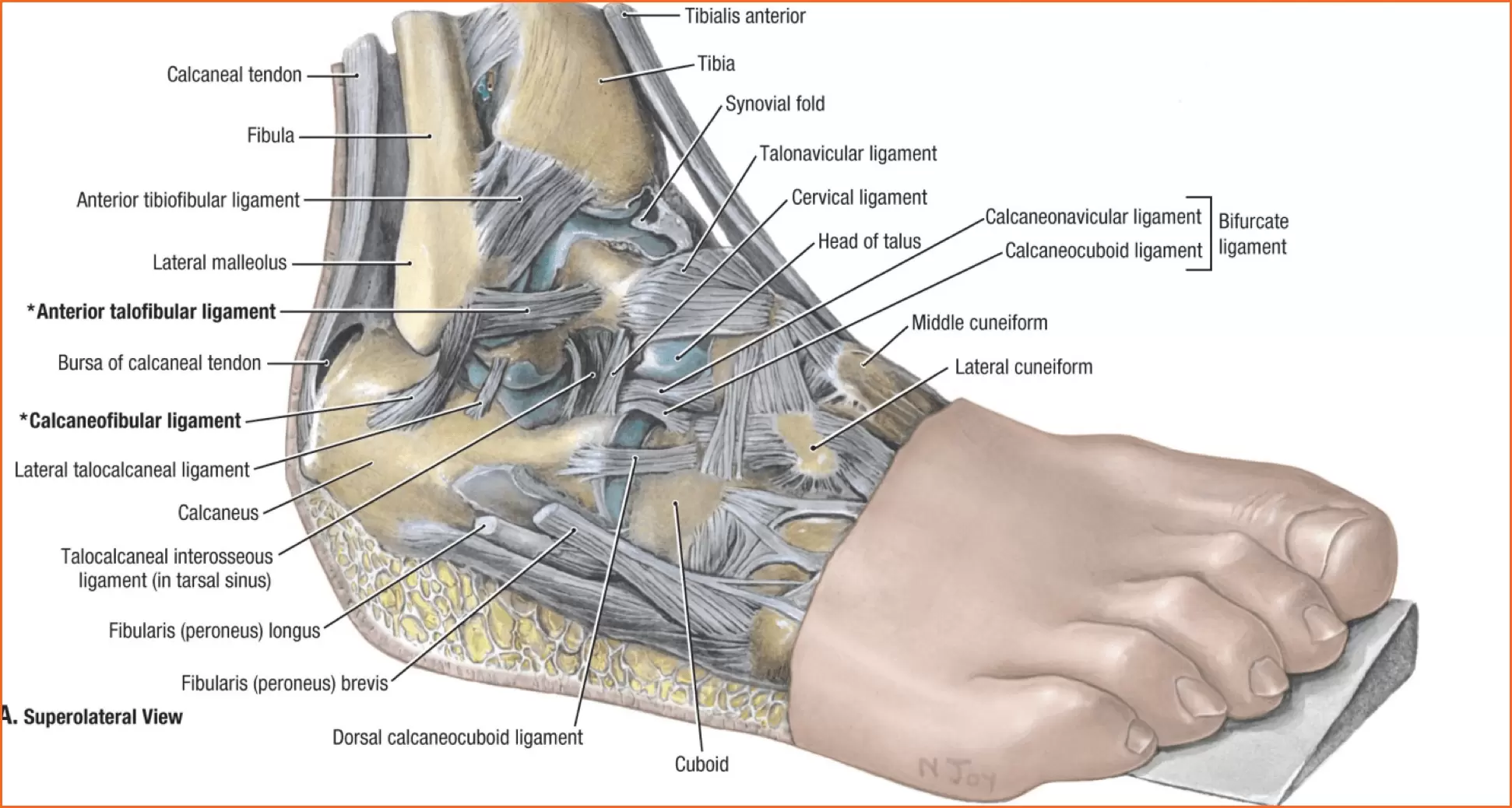
Ankle bones
The ankle joint consists three bones: The ankle bone (Talus), shin bone (Tibia), which holds the Talus at the lower end along with a parallel thinner bone (Fibula) and the heel bone (calcaneus). The talus has a socket-like structure which allows it to work like a one-directional hinge.
Aslo read, Physiotherapy Clinic in Etobicoke
Ligaments and Tendons
Ligaments and Tendons serve similar functions but in slightly different ways. While they are both referred to as “soft tissue” structures, ligaments attach bones to bones while tendons attach muscles to bones. Both of them are made of collagen fibers.
Muscles
Muscles work by stretching and contracting, which allows us to walk, run and jump. Below are some of the most prominent muscles of the lower leg:
- The peroneals (peroneus longus and peroneus brevis) are located on the outside edge of the ankle and are mainly responsible for bending the foot down and out.
- The calf muscles (gastrocnemius and soleus) connect to the calcaneus by the Achilles tendon. When the calf muscles tighten, they bend the ankle down.
- The tibialis posterior muscle supports the arch of the foot and helps turn the foot inward.
- The tibialis anterior pulls the ankle upward.
Also read, Physiotherapy Clinic in Mississuaga
Nerves
The nerves on the outer edge and front part of the ankle control muscle movement and provide sensation to the top and outside edge of the foot.
Blood Vessels
There are many arteries which supply blood to the ankle such as the dorsalis pedis, tibial artery, etc. Without adequate blood supply, the muscles of the ankle would not be able to function and would cause significant impairments.
We have 6 clinics located across the GTA: Etobicoke, Oakville, Mississauga, North York, and Toronto (King Street West and Yonge Street. If you are suffering from foot or ankle problems you may benefit from treatment. Don’t suffer any longer! Call or email us today and we will be happy to answer all of your questions.
You can book an appointment for Ankle Anatomy: Click here to book an appointment
Understanding ankle anatomy is crucial for preventing injuries and ensuring proper treatment. If you need expert physiotherapy services to help manage ankle conditions or injuries, consider visiting clinics in physiotherapy Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, and Liberty Village. These locations provide comprehensive care and customized treatment plans to support your recovery and maintain ankle health.
Winter is on its way out and spring is almost upon us. With the warmer change in weather, we shake off our desire to hibernate and become more active, doing activities we haven’t done in months! However, we sometimes rush into things too quickly and can put too much pressure on our feet, leading to the development of various foot problems. Orthotics might be the answer for you as they can help change the way your foot makes contact with the ground and can take pressure off high-pressure areas in the foot.
What are Orthotics?
Orthotics are insoles that you use inside your shoes that help rectify biomechanical problems of the foot. They are usually made of a combination of rubber, metal, plastic, leather, or any other synthetic material. Our feet have so many muscles, bones, and joints that abnormal biomechanics of how they’re moving can result in numerous foot problems along with pain in your knee, lower back, hip or leg.
Also read, Physiotherapy Clinics in Mississuaga
How can Orthotics correct foot conditions?
- Orthotics help balance pressure placed on the feet by redistributing the weight appropriately
- They help stabilize the heel
- Support the arch of the feet
- Provides cushioning to delicate and inflamed areas of the feet that arise from too much walking, jogging, running, etc.
There are generally two options when it comes to selecting orthotics: over-the-counter orthotics and custom-made orthotics. Over-the-counter orthotics are available at your local pharmacy and big box store and they can be used with your regular shoes to correct trivial problems. However, because they are prefab, generalized products, there is a possibility that they might make your foot pain worse due to it not being the right kind of support that you need. Custom made orthotics work best because they are tailor-made to correct the problems specific to your feet. Check out our earlier blog on the most popular kinds of Orthotics for further detail.
Also read, Physiotherapy Clinic in Oakville
Here’s a tip
Orthotics can still benefit you even if you don’t suffer from any foot issues but are an active participant in sports. If your foot is dealing with stress and impact, or if you have recently gained weight, orthotics will help you walk better!
Put your best foot forward and in the right direction!
We at Triangle Physiotherapy will quite literally help you get back on your feet! Our Chiropodist can advise you on how to look after your feet and what type of shoes or orthotics to opt for. Book an appointment with our Chiropodist today at any of our 6 clinics located across the GTA: Etobicoke, Oakville, Mississauga, North York, Toronto (King Street West) and Yonge Street. If you have any questions regarding any kind of foot conditions, please call or email us and we will be happy to help you!
Orthotics can be highly effective in managing various foot-related conditions, providing support and alignment to improve comfort and mobility. If you are looking for physiotherapy services to complement your orthotic treatment, there are clinics available in physiotherapy Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, and Liberty Village. These locations offer specialized care and customized treatment plans to address your foot health needs.
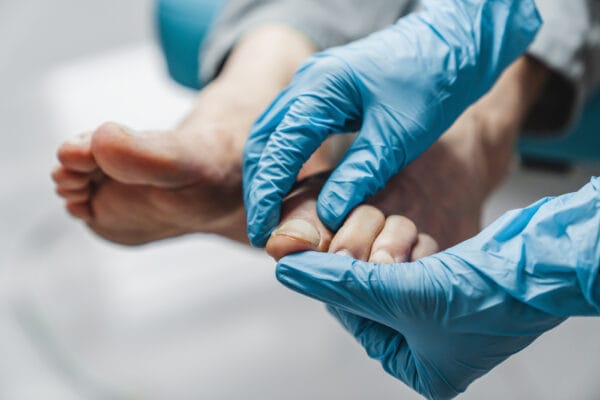
Our feet are likely the most used body parts of all of our limbs. Be it sitting or standing, we are always using our legs in one way or the other. In fact, the use of our feet and legs usually begins the moment we wake up. So it is safe to say that our feet play a vital role in our day-to-day life and as such, it is important to take good care of them. Our feet carry the entire weight of our body throughout the day. They undergo tremendous pressure with every step we take as they get compressed and endure repeated movement against our footwear. Over a period of time, pressure on certain parts of the foot can increase and the body compensates by adding extra layers of scar tissue and skin on parts of feet that undergo high pressure, such as the ball and heel & toes of the foot. This can cause there to be painful areas of pressure on the foot or the formation of callouses on areas of higher pressure on the foot.
Also read, Best Physiotherapy Clinic in Etobicoke
Why schedule an appointment with a Chiropodist?
Walking, running, sitting – everything involves your legs. A minor injury or pain can cause huge discomfort in your everyday life and can escalate to become a serious issue. For example, an ingrown toenail or an infection can be very painful and uncomfortable. Seeing a Chiropodist at an earlier stage will help immensely in preventing and managing these kinds of foot-related problems.
An appointment with a Chiropodist will involve a thorough assessment of your foot-related problem and treatment that will help alleviate the problem. Even without a significant ongoing foot issue, a visit to the Chiropodist can help you in preventing one from developing by gaining more insight into your walking pattern or providing education on correct foot care. They are trained to diagnose and treat a wide variety of foot-related conditions and are able to understand their patient’s needs in order to prevent and treat both acute and chronic conditions that involve the foot and lower limb functions.
Also read, Best Physiotherapy Clinic in Oakville
What do we treat at Triangle Physiotherapy?
Our Chiropodist is a highly skilled professional that is an expert in their field. At Triangle Physiotherapy, our registered Chiropodists diagnose, assess, and treat a wide range of foot-related health issues and abnormalities including but not limited to:
- Alignment and support to prevent or correct abnormalities in the lower limbs
- Abnormal gait patterns
- Foot pain
- Sports injuries
- Diabetic foot care
Also read, Best Physiotherapy Treatment in Mississauga
How to Contact Triangle Physiotherapy?
We have 8 clinics located across the GTA: Etobicoke, Oakville, Mississauga, North York, and Toronto (King Street West, Queens Quay, and Yonge Street. If you have any questions regarding what type of chiropody treatment may be appropriate for you, please call or email us and we will be happy to answer your questions. You can also Book an Appointment with a Chiropodist now.
Chiropodists play a vital role in managing foot and lower limb conditions, often collaborating with physiotherapists to provide comprehensive care. If you’re looking for professional physiotherapy services to complement chiropody care, consider clinics in physiotherapy Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, and Liberty Village. These locations offer expert care and personalized treatment plans to help you achieve optimal foot health.
It is always an inconvenience when our bodies don’t perform the way we want them to. It is especially worrisome when we don’t understand why we aren’t feeling at our best. Many times, the feeling of being “off” can be attributed to a vestibular problem. Vestibular disorders can affect a person in numerous ways, and often without any pattern. The vestibular system includes the parts of the inner ear and brain that help control balance and eye movements. It consists of five sensory organs that provide our brain with information about head position and movement.
People with vestibular disorders often experience problems with vertigo, dizziness, and visual disturbance. Although dizziness & vertigo can occur in people of any age, it is more common among older adults. The feeling of dizziness can be tough to manage and might cause someone to restrict their physical activities and social engagements in order to prevent an injury from a fall. Other typical, secondary problems that can arise from vestibular disorders are nausea/vomiting that reduced the ability to focus or concentrate and fatigue.

Evidence has shown that vestibular rehabilitation can be effective in improving symptoms related to many vestibular disorders. Symptoms due to vestibular disorders can reduce the quality of life and slow down all aspects of our daily routine.
Also read, Physiotherapy Clinic in Oakville
Some common symptoms are:
- Dizziness and imbalance
- Decreased in muscular strength and flexibility
- Increased joint stiffness
- Reduced on stamina
- Vision disturbance
- Hearing changes
- Psychological changes
Diagnosis and treatment are not always the only solution for vestibular disorders. It is important to understand some common, significant limitations in order to better manage them.
Also read, Physiotherapy Mississauga
Some common limitations are:
- Balance is commonly taken for granted until it is impaired
- People with vestibular disorders can suffer cognitive impacts, such as poor concentration, memory, and word recall
- People also restrict their movement and activity levels to avoid pain
It is important to note that most of these symptoms can also be caused by other conditions and should be discussed with a healthcare professional or a skilled physiotherapist. At Triangle Physiotherapy, with the help of our skilled team of physiotherapists, your vestibular issues can become a thing of the past!
Vestibular rehabilitation is crucial for managing vertigo and improving balance through targeted exercises and therapy. If you are in need of professional physiotherapy services for vestibular rehabilitation, consider clinics in physiotherapy Etobicoke, Oakville, North York, Toronto, Lawrence Park, Queens Quay, Erin Mills, Mississauga, and Liberty Village. These clinics offer expert care and personalized treatment plans to help you regain stability and enhance your quality of life.
What do we mean by Sports Injuries? Any sort of injury that is caused when we get too involved and carried away in the spirit of any sport. When the passion is high, and the energy is there we tend to suffer from small accidents related to Knee pain, Elbow, etc.
What qualifies as a Sports Injury?

It’s any type of injury that might arise from getting too involved and carried away in the spirit of any sport. In the heat of the moment during a sports game, it is easy to ignore smaller annoyances that might progress to become significant sources of pain.
Also read, Physiotherapy Oakville
So, what do many people do when they inevitably suffer a sports injury?
The most common answer is to go and visit a doctor. However, we tend to forget that the most effective and immediate assistance we can get is from a physiotherapist. Reducing swelling and providing pain relief are usually the first steps that a physiotherapist will take to promote recovery after an injury.
Advanced progression of the treatment plan usually involves techniques like stretching and providing range of motion and strengthening exercises that are meant to help the injured person regain strength and balance. The physiotherapist will also ensure that you don’t push yourself too far or too fast, thereby helping you prevent re-injury.
Below are some common questions and answers that might be relevant to you:
Who is better equipped to diagnose my injury – a doctor or a physiotherapist?
Both doctors and physiotherapists have the necessary skills to diagnose your injury. Interestingly the most important thing is that there is a DIAGNOSIS made!
Who is better equipped to manage/treat my injury – a doctor or a physiotherapist?
Well, it depends on the injury. For example, it is not uncommon for a physiotherapist to refer a patient to a doctor to ask for a prescription for some anti-inflammatory medication as these are not able to be prescribed by a physiotherapist. However, a physiotherapist will generally provide more detail regarding the injury, as well as provide manual treatment and prescribe a detailed exercise program for the patient that will help promote recovery.
Also read, Physiotherapy Clinic Mississauga
When do I need to consult a physiotherapist?
There are many other conditions apart from sports injuries that would require treatment from a physiotherapist. Some of them are:
- Any arthritic conditions
- Treatment of pelvic floor disorders
- Chronic/Overuse injuries
- Muscle or joint issues that might arise during pregnancy
- Vestibular conditions
- Various other muscle strains and sprains
Any of the above-mentioned problems should be treated immediately in order to prevent further aggravation of the condition! Seek the help of our specialists at any of our locations in Etobicoke, Oakville, North York, Mississauga & Toronto, and get rid of such dilemmas!